What is cervical cytology?
- EPA Announces First-Ever Regulation for “Forever Chemicals” in Drinking Water
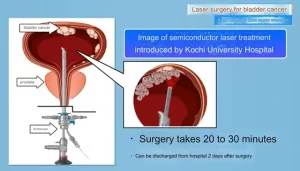
- Kochi University pioneers outpatient bladder cancer treatment using semiconductor lasers
- ASPEN 2024: Nutritional Therapy Strategies for Cancer and Critically Ill Patients
- Which lung cancer patients can benefit from neoadjuvant immunotherapy?
- Heme Iron Absorption: Why Meat Matters for Women’s Iron Needs
- “Miracle Weight-loss Drug” Semaglutide Is Not Always Effective
What is cervical cytology?
What is cervical cytology? Does abnormal TCT test cause cervical cancer? Cervical cancer screening is not complicated.
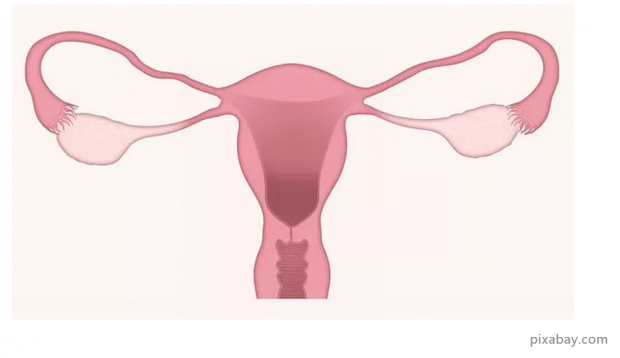
Cervical cancer is a common gynecological malignant tumor, and its incidence ranks second among female malignant tumors, which seriously threatens the life and health of patients. But cervical cancer is a preventable and curable disease. With the popularization of screening, cervical cancer can be detected and treated early, and the mortality rate has dropped significantly.
01 Cervical cancer screening methods
Cervical cancer screening is not complicated. The first is cervical cytology (TCT) and HPV testing. If the screening finds abnormal cervical squamous epithelial cells, or high-risk HPV positive, further colposcopy is needed.
The colposcopy can directly observe the cervix and its pathological changes. At the same time, the cervix tissue can be taken from the pathological area with multiple clamps and sent for pathological examination. Pathological examination is the most reliable method for diagnosing cervical lesions and is called the “gold standard”.
02 What is TCT inspection?
TCT, or liquid-based thin-layer cytology, is currently the most commonly used method for cervical cancer screening. The detection rate of cervical cancer cells by TCT can reach more than 60%, and it can also find precancerous lesions and microbial infections, such as molds, trichomoniasis, and chlamydia.
Compared with the traditional Pap smear, the TCT test no longer coats the retained cells on a glass slide, but collects them in a bottle filled with liquid. The advantage is that it can retain enough cells to avoid insufficient cells during the test. . Therefore, the satisfaction of specimens and the detection rate of abnormal cervical cells are significantly improved.
03 TCT results and significance
(1) No intraepithelial diseased cells or malignant cells (NILM): cervical health
(2) Atypical squamous cells of ambiguous significance (ASC-US):
Under the microscope, I saw squamous epithelial cells that were different from the usual ones, but I couldn’t determine whether these cells were really abnormal. You need to check for HPV. If there is a high-risk HPV infection, colposcopy is required. If there is no high-risk HPV infection, it can be reviewed regularly.
(3) High-grade squamous intraepithelial lesions (ASC-H) are not excluded for atypical squamous epithelial cells with unclear significance:
On the basis of ASC-US, although the degree of cell abnormality cannot be clearly defined, it tends to have high-grade lesions and requires a colposcopy to take a biopsy to confirm the diagnosis.
(4) Low-grade squamous intraepithelial lesion (LSIL):
Cervical squamous epithelial cells may have low-grade lesions, and further colposcopy is needed.
(5) High-grade squamous intraepithelial lesion (HSIL):
Suspicious high-grade lesions occurred in cervical squamous epithelial cells, which requires further colposcopy to confirm the diagnosis.
(6) Squamous cell carcinoma (SCC):
Cervical squamous cells may have become cancerous.
(7) Atypical glandular cells (AGC):
Glandular epithelium may have lesions. Such cells may originate from the cervix, endometrial lining, fallopian tube lining, etc. Further colposcopy + cervical canal scraping are required, and gynecological ultrasound examination is required to confirm the diagnosis.
In short, the sensitivity and specificity of a single cytology test is not high, and it is not enough to diagnose cervical cancer. Cervical cytology combined with HPV testing, as well as colposcopy and cervical biopsy, can determine whether he has cervical cancer.
(source:internet, reference only)
Disclaimer of medicaltrend.org