Proved: Nuts can prevent cancer!
- Did Cloud Seeding Unleash a Deluge in Dubai?
- Scientists Identify Gut Bacteria and Metabolites that Lower Diabetes Risk
- OpenAI’s Model Matches Doctors in Assessing Eye Conditions
- UK: A Smoke-Free Generation by Banning Sales to Those Born After 2009
- Deadly Mutation: A New Monkeypox Variant Emerges in the DRC
- EPA Announces First-Ever Regulation for “Forever Chemicals” in Drinking Water
Proved: Nuts can prevent cancer!
Proved: Nuts can prevent cancer!. Every 20g/day increase in nut intake reduces the risk of cancer by 10%.
Highlights of the latest news:
- Eat more nuts to make the gastrointestinal tract healthier, which can significantly reduce the risk of digestive system cancer.
- Different types of obesity have different cancer risks! A high body mass index increases the risk of colorectal cancer in men, while a high waist-to-hip ratio increases the risk of colorectal cancer in women.
01 Nuts can significantly reduce the risk of digestive system cancer
Cancer is one of the main causes of death in human beings and seriously endangers public health. According to the analysis of the International Agency for Research on Cancer (IARC) under the World Health Organization, with the rapid population growth and aging, the global cancer burden is expected to increase 29.5 million cancer cases and 16.4 million cancer-related deaths by 2040 .
Adhering to a healthy diet has been proven to reduce the risk of certain cancers by 4%-57%. Nuts contain a variety of nutrients that are beneficial to human health, such as unsaturated fatty acids, dietary fiber, vitamins, and minerals.
In the past few decades, many epidemiological studies have investigated the relationship between nut intake and different cancer risks, but failed to reach a consensus. In order to further assess the relationship between nuts and cancer risk, researchers from Tongji Hospital of Huazhong University of Science and Technology conducted a meta-analysis of the latest relevant literature and recently published it in Cancer Epidemiology, Biomarkers and Prevention, an authoritative journal in the cancer field. The results showed that eating nuts is negatively associated with cancer risk, especially cancers of the digestive system.

Figure 1. Article title and author information
The researchers comprehensively searched all prospective studies on the association between nuts and cancer risk included in the Web of Science and PubMed databases as of June 2019. Finally, 33 studies that met the analysis criteria were included, including a total of 50,879 cancer cases. Of these, 13 studies were conducted in the United States, 16 studies were conducted in Europe, and 4 studies were conducted in Asia.
The analysis found that eating nuts was significantly associated with reducing overall cancer risk (RR=0.90; 95%CI, 0.85-0.95, P=0.028). Subgroup analysis according to the classification of digestive system cancer and non-digestive system cancer showed that eating nuts was significantly associated with a reduction in the risk of digestive system cancer [risk ratio (RR)=0.83; 95%CI 0.77-0.89, P=0.036]. There is no obvious correlation with digestive cancer.
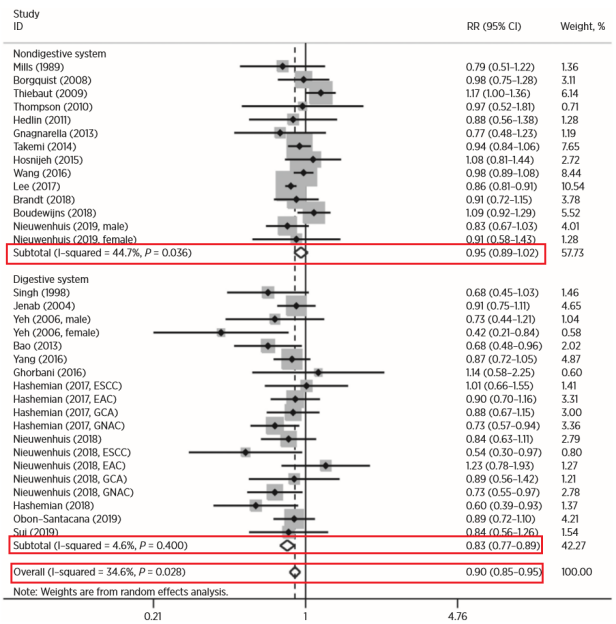
Figure 2. Nuts consumption and cancer risk analysis
Subgroup analysis according to race showed that there is a significant correlation between nut intake and cancer risk among Asians and North Americans, but not among Europeans. A subgroup analysis based on follow-up time showed that studies with longer follow-up time (10-20 years and 20 years) showed a significant decrease in cancer risk, while studies with a follow-up time of less than 10 years did not. Among the three common nuts (peanuts, tree nuts, and peanut butter), eating only tree nuts can significantly reduce the risk of cancer (RR=0.86; 95%CI 0.77–0.97).
Consistent with the above results, eating nuts has a protective effect on most gastrointestinal cancers, including colorectal cancer (RR=0.81; 95%CI 0.68-0.96), pancreatic cancer (RR=0.84; 95%CI 0.73-0.98) and Gastric cancer (RR=0.79; 95%CI 0.68-0.91).
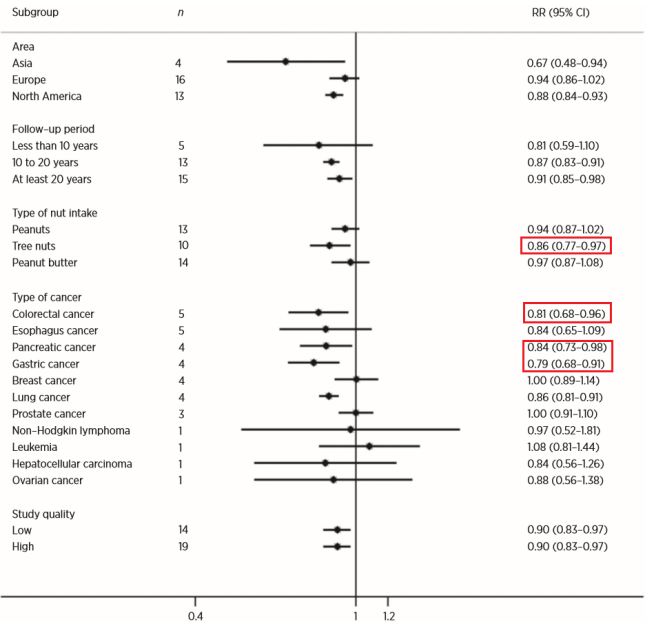
Figure 3. Analysis of different subgroups
Further analysis of the linear dose relationship between nut intake and cancer found that with the increase in daily nut intake, cancer risk decreased in a linear dose-dependent manner, and every increase in nut intake by 20g/day, cancer risk decreased 10% (RR=0.90; 95%CI, 0.82-0.99).
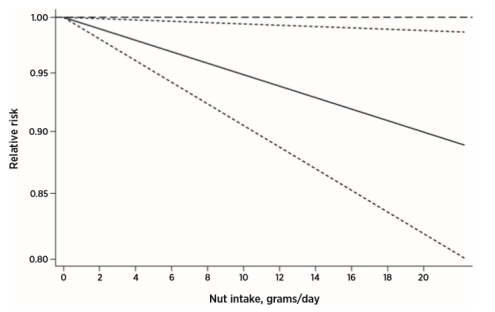
Figure 4. Analysis of the linear dose relationship between nut intake and cancer risk (solid line indicates relative risk)
Nuts, especially tree nuts, have a protective effect on cancer and can reduce the risk of cancer, especially the risk of cancer in the digestive system. For every increase of 20g/day, the risk of cancer will be reduced by 10%. Common tree nuts include walnuts, hazelnuts, almonds, and pine nuts.
02 Be alert! Being overweight or obese increases the risk of colorectal cancer
Colorectal cancer (CRC) is a common malignant tumor of the digestive system. In recent years, its morbidity and mortality have shown a continuous upward trend. Overweight or obesity has been proven to be one of the main risk factors for colorectal cancer, and different types of obesity and gender have different effects on the risk of CRC. Studies have suggested that body mass index (BMI, an indicator of total fat) and waist-to-hip ratio (WHR, an indicator of abdominal fat) have different effects on the risk of CRC for men and women.
In order to further explore the relationship between different types of obesity, gender and CRC risk, researchers from the International Agency for Research on Cancer (IARC) of the World Health Organization and the University of Bristol in the United Kingdom conducted a clinical study. And recently published in the well-known medical journal BMC Medicine, the results show that the higher the BMI, the higher the risk of colorectal cancer in men; the higher the WHR, the higher the risk of colorectal cancer in women.

Figure 5. Article title and author information
A total of 125,915 participants were included in the study, of which 58,221 were colorectal cancer patients in the observation group, and 67694 were normal people who did not suffer from colorectal cancer in the control group. The collected data analyzed the specific association between obesity location and gender and CRC risk, and explored whether obesity-related metabolites and single nucleotide polymorphism (SNP) gene variants can explain these associations.
The results show that a higher BMI is associated with a higher total CRC risk. For every increase in BMI of 4.8kg/m2, the total risk of CRC increases by 16% [risk ratio (OR)=1.16, 95%CI 1.07-1.26]; for men, every increase in BMI by 4.2kg/m2 increases the risk of CRC23 %[OR=1.23, 95%CI 1.08-1.38]; for women, for every increase of 5.2kg/m2 in BMI, the risk of CRC increased by 9% [OR=1.09, 95%CI 0.97-1.22].
A higher WHR is associated with a higher total CRC risk. For every 0.09 increase in WHR, the total CRC risk increases by 28% [OR=1.28, 95%CI 1.16-1.42]; for men, every 0.07 increase in WHR increases the CRC risk by only 5% (OR=1.05, 95%CI) 0.81-1.36); but for women, for every 0.07 increase in WHR, the risk of CRC increases by 25% (OR=1.25, 95% CI 1.08-1.43).
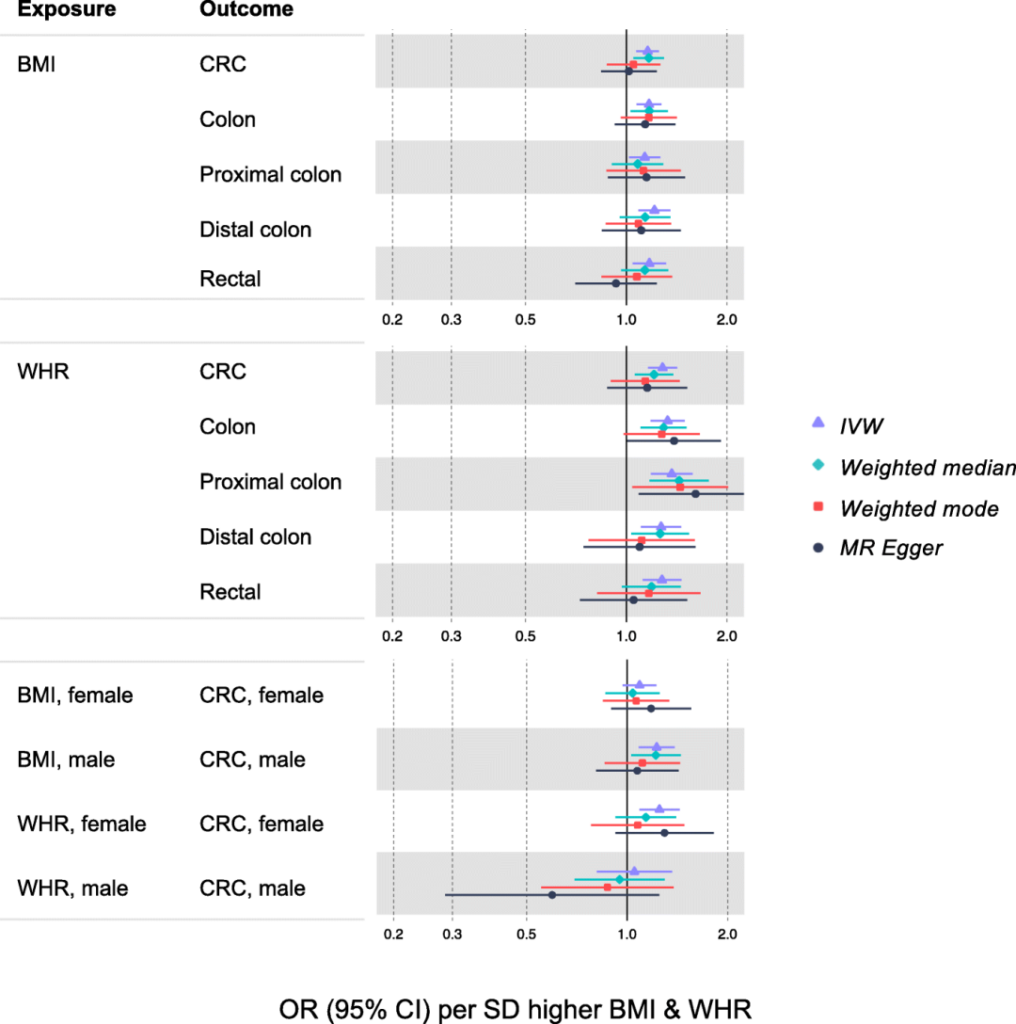
Figure 6. The correlation between BMI and WHR and CRC risk
The study also found that changes in 104 metabolites are related to BMI or WHR, such as total lipids, high-density lipoproteins, low-density lipoproteins, monounsaturated fatty acids, lactic acid and pyruvate. However, analysis shows that these changes are not enough to explain the association between obesity and CRC, and further research is still needed.
Both total fat and abdominal fat increase are significantly associated with an increased risk of colorectal cancer. Among them, the body mass index has a stronger correlation with the risk of colorectal cancer in men, and the waist-to-hip ratio has a stronger correlation with the risk of colorectal cancer in women.
Therefore, to maintain a healthy weight, in addition to paying attention to body mass index, it is also necessary to pay attention to waist-to-hip ratio. Increased abdominal fat will also increase the risk of colorectal cancer, especially for women.
(source:internet, reference only)
Disclaimer of medicaltrend.org



