The long history of the birth of mRNA vaccines
- Statins Lower Blood Lipids: How Long is a Course?
- Warning: Smartwatch Blood Sugar Measurement Deemed Dangerous
- Mifepristone: A Safe and Effective Abortion Option Amidst Controversy
- Asbestos Detected in Buildings Damaged in Ukraine: Analyzed by Japanese Company
- New Ocrevus Subcutaneous Injection Therapy Shows Promising Results in Multiple Sclerosis Treatmen
- Dutch Man Infected with COVID-19 for 613 Days Dies: Accumulating Over 50 Virus Mutations
The long history of the birth of mRNA vaccines
The long history of the birth of mRNA vaccines. Since mRNA was successfully extracted for the first time in 1960, we have obtained an epoch-making COVID-19 mRNA vaccine by modifying the mRNA after 60 years of research. This technology is playing great significance at a speed we did not expect.
In addition to medical professionals who have already seen its potential, Bill Gates and Musk in the non-medical field have also begun to pay attention to the investment layout of this technology. Tesla CEO Musk said not long ago: “The future of medicine is mRNA. Basically you can use mRNA to cure everything. It is like a computer program, you can program it to perform any operation you need. You can even All can become butterflies.”

What is mRNA therapy?
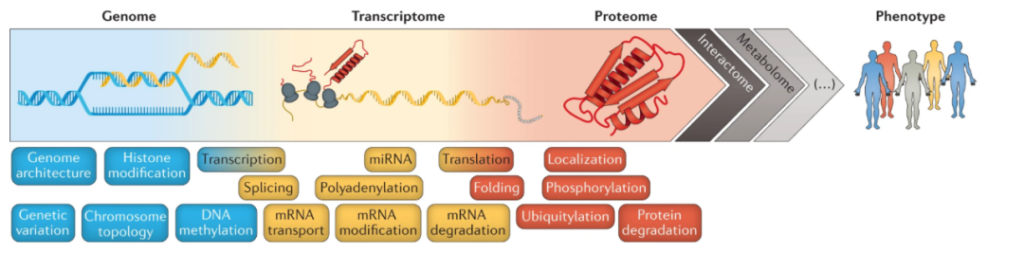
Picture gene expression process
Our body is functioned by thousands of proteins that coordinate with each other. Simply put, mRNA is like a general manual. Cells only need to process and synthesize proteins according to this manual. By customizing the mRNA sequence, we can get any protein we want, whether it is an immunoprotective antibody or a catalytic enzyme. Before the advent of the era of mRNA drug therapy, the traditional protein drug design was to directly use genetically engineered cells to express the target protein in large quantities in vitro, and then separate and purify it into pharmaceutical preparations for in vivo administration. The process was time-consuming and cumbersome. The emergence of mRNA therapy is equivalent to using cells in the body as a factory for protein expression and transferring the expression process in vitro to the body, thus greatly shortening the development time. This is a technological innovation that is different from the traditional drug treatment research and development process. Some scientists commented that the realization of mRNA technology is equivalent to the first time that we have used bioengineering technology to transfect humans.
The birth of mRNA therapy starts from twenty years ago.
Hungarian scientist Katalin Karikó, born in 1955, has been conducting research on RNA at the University of Pennsylvania in the 1990s. However, under the circumstances at the time, RNA research was difficult to carry out. Usually scientists can only isolate a small amount of RNA from a sample, and the mRNA obtained during the isolation process is easily destroyed by RNA degrading enzymes in the skin and the air. She has been actively trying to use mRNA therapy to treat diseases for a long time, but no one is interested in her work, and she has repeatedly failed in the process of applying for funds from the government, which has caused her research project to be in a precarious state for several years. . In 1995, due to the continuous inability to apply for project funds, Carrico was demoted after six years of working in Pennsylvania and missed the opportunity to become a full-time professor at the school.
Katalin Karikó
The turning point came in 1997, when Kaliko met Drew Weissman, an immunologist who was also a professor in Pennsylvania. Drew is a young American scientist who was doing AIDS vaccine research in Fauci’s laboratory at the NIH Institute. He was Anthony Fauci, the public health spokesperson of the US government during the epidemic.

Drew Weissman and Katalin Karikó
The biggest bottleneck encountered in Carrico’s research process is that whether it is natural RNA or artificially synthesized in vitro, it will activate the response of human immune cells without exception, resulting in RNA before it can be translated into protein. Degraded. The specific mechanism is that due to the different degrees of evolution of different species such as mammals, bacterial viruses, etc., RNA has a variety of modification methods. The human immune system can determine whether the RNA is a foreign pathogen through subtle sensing of different modifications. And decide whether to launch an immune attack.
In 2005, with the assistance of Weissman, Kaliko discovered that when they modified uridine, one of the components of RNA, a surprising thing happened. The modified mRNA could evade the signal recognition of the immunosensor. Solve the biggest problem in RNA application research. They applied for a patent at that time and published this breakthrough research in Immunity (10.1016/ j.immuni.2005.06.008), which was the birth of RNA therapy.
Since then, research on RNA therapy has been published one after another, and this field has gradually attracted the attention of scientists in various fields. Among the many subsequent studies on RNA, the most influential one was the work of a Canadian stem cell biologist Derrick Rossi (Derrick Rossi). In 2005, when Carrico and Weissman’s research was published in Immunity, Rossi was a postdoctoral fellow at Stanford University. When he read this article, he was keenly aware of the far-reaching impact of this technology, and even predicted that the discovery of Carricko and Weissman was worthy of the Nobel Prize in Chemistry.

Derrick Rossi
In 2007, Rossi became an assistant professor at Harvard Medical School. He used Carrico and Weissman’s method of modifying mRNA uridine to conduct RNA application research on stem cells, trying to reprogram somatic cells into embryonic stem cells . After more than a year of exploration, one day Rossi’s postdoc called him to the microscope. An exciting scene appeared. The cell culture dish under the microscope was full of embryonic stem cells they wanted to get after reprogramming. . In 2010, Rossi’s research was named one of the top ten medical breakthroughs in Time magazine.
One day in May 2010, Rossi’s friend introduced him to MIT professor Robert Langer. Lange was only 43 years old when he was elected a member of the American Academy of Sciences, and no one has surpassed him. At the same time, he is also a well-known biotechnology entrepreneur, with outstanding talents in the fields of biotechnology and drug development. He holds thousands of patents, promotes the launch of new drugs by major pharmaceutical companies, is the most cited engineer in history, and won the Charles Stark Draper Prize, the Nobel Prize known as an engineer.
When Rossi and Lange had a short two-hour conversation, Lange immediately realized with his keen intuition that this is not just an innovative method that can only be used to transform stem cells, it has great prospects. Lange believes that this technology can be used to compile almost all the proteins he wants. He thought carefully for a while and said to Rossi, “This technology can be used in other fields besides reprogramming stem cells, such as drugs, vaccines, etc. ; It can treat almost all diseases, thereby saving thousands of lives.”
Robert Langer
Rossi had never thought of applying this technology in fields other than stem cells, but after talking with Lange, he could hardly suppress the great excitement and joy in his heart. After returning home, he said to his wife, “We may Founding the most successful company ever!” Three days later, Noubar Afeyan, CEO of the flagship investment group of the famous Cambridge venture capital firm, saw the greater potential of mRNA therapy. After he led his own team of researchers who confirmed the validity of Rossi’s data, Afyan resigned from the flagship company within a few months and co-founded Moderna with Rossi and Lange in 2010. The name means Modified RNA.
Since the establishment of Moderna, they have been studying whether injecting mRNA encoding vascular endothelial growth factor (VEGF) into the heart of mice can repair the heart tissue damaged during a heart attack. If this method is feasible, by prolonging the time for mRNA to function in cells, enough protein can be produced to improve the survival rate and health of the body after a heart attack. The research was published in Natrue Biotechnology in 2013 (Nat Biotechnol 2013, DOI: 10.1038/nbt.2682). And received a US$240 million investment from AstraZeneca. After repeating the experiment in mice and pigs, AstraZeneca initiated a clinical trial of this therapy in patients with heart disease. The project is currently in clinical phase II. Experimenting.

On the other side of the earth, in Mainz, on the left bank of the Rhine River in Germany, a pair of Turkish scientists also paid attention to the research of Carrico and Weissman early on, and quickly established a biotechnology company based on the therapy. This company is BioNTech founded by a couple of physicians, Sahin (萨欣) and Di Lexi (Tureci). At that time, their husband and wife were conducting immunotherapy-related research in a hospital in Saarland, Germany. The main content of the research was to transform a personalized tumor vaccine to induce the immune system to kill tumors. After discovering the potential of mRNA, they successfully got the investment to establish BioNTech, which uses mRNA to develop tumor vaccines, and hired Calico as the senior vice president. Compared with Moderna’s high-profile appearances led by many investment circles at the beginning of its establishment, BioNTech’s development process is quite low-key. There has not been any press release for a long time, focusing on scientific research.

Sahin and Tureci
The yield of traditional vaccines is a serious problem. The manufacturing process takes several months. In contrast, mRNA vaccines can be mass-produced within a few weeks because of their simple components. Shortly after the establishment of Moderna, the Bill and Melinda Gates Foundation invested in Moderna’s mRNA vaccine program to treat diseases caused by Zika virus and HIV; Pfizer and BioNTech also cooperated in the development of mRNA influenza vaccines.

However, the time for Moderna and BioNTech to shine is the outbreak of the COVID-19 epidemic.
On January 10, 2020, Chinese scientists announced the gene sequence of the new coronavirus. Both BioNTech and Moderna started the development of mRNA vaccines in the first place. The vaccine design of the two companies is to encapsulate the mRNA encoding the dendritic protein of the new coronavirus in liposomes. When the vaccine is injected into the body, the cells in the body can synthesize a large amount of viral protein through the mRNA and induce the immune system Recognize the protein to generate immune memory of the new coronavirus to resist viral infection.
BioNTech chose to cooperate with Pfizer. They did not apply for any funding from the government in the early stages of research and development, and promised to receive government funding after at least 1 million doses of the vaccine were sold. If the R&D process fails, Pfizer is willing to bear the economic losses.
- November 20, BioNTech’s vaccine product BNT162 applied for FDA emergency approval.
Its clinical data showed that 36523 participants were randomly assigned to the vaccine group and the placebo group. After two shots of the vaccine were given to the subjects in the vaccine group, the number of cases of COVID-19 in the vaccine group and the placebo group were counted, and calculated After receiving two injections, the effectiveness of the vaccine protection is 95%. According to the application documents submitted by Moderna to the FDA on November 30, there are a total of 15,179 vaccine recipients and 15,163 placebo participants, and its effectiveness is also more than 95%. - December 2nd, BNT162 was launched in the UK as the world’s first COVID-19 vaccine.
- December 11, it obtained the emergency use right approved by the US FDA.
- December 18, Moderna also obtained the emergency use right of the COVID-19 vaccine.
Bill Gates said: “Why are so many companies willing to take risks this time? One of the reasons is that they see an opportunity to use their expertise to help end the epidemic.” Pfizer said that the willingness to take risks is to apply innovative technology to scientists. The exploration of vaccine possibilities prevents them from being too restricted.
Looking back on the birth of mRNA, every node in just ten years has important significance. Carrico’s persistence in the absence of funds, breakthrough discoveries after encountering Weissman, and the later founding of Moderna and BioNTech all pushed the field forward. More importantly, the outbreak of the COVID-19 epidemic has given the possibility of bringing mRNA vaccines to the market in a short period of time, and this will promote the prospects and plans of the entire drug research and development field towards mRNA treatment.
(source:internet, reference only)
Disclaimer of medicaltrend.org



