Is the reduced effectiveness of COVID-19 vaccines really due to Delta variants?
- Statins Lower Blood Lipids: How Long is a Course?
- Warning: Smartwatch Blood Sugar Measurement Deemed Dangerous
- Mifepristone: A Safe and Effective Abortion Option Amidst Controversy
- Asbestos Detected in Buildings Damaged in Ukraine: Analyzed by Japanese Company
- New Ocrevus Subcutaneous Injection Therapy Shows Promising Results in Multiple Sclerosis Treatmen
- Dutch Man Infected with COVID-19 for 613 Days Dies: Accumulating Over 50 Virus Mutations
Is the reduced effectiveness of COVID-19 vaccines really due to Delta variants?
- Red Yeast Rice Scare Grips Japan: Over 114 Hospitalized and 5 Deaths
- Long COVID Brain Fog: Blood-Brain Barrier Damage and Persistent Inflammation
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Is the reduced effectiveness of COVID-19 vaccines really due to Delta variants?
Although the decrease in VE of the COVID-19 vaccine after the epidemic of the Delta variant is observed in the real world, it cannot be easily concluded that “the decrease in VE of the COVID-19 vaccine is caused by Delta”.
As the Delta variant continues to wreak havoc, the world has entered a new round of epidemic peaks since June this year. Even the United States and Israel, which have high vaccination rates, have seen a rise in the number of infections, causing global panic. In this context, “Vaccine effectiveness (VE) decline” has become a hot topic. How does the worrying new coronavirus vaccine VE perform in the real world? Let us take a look at the latest research progress:
Real-world research confirms: With the prevalence of Delta variants, the COVID-19 vaccine VE decreases
On August 30, 2021, the American Centers for Disease Control and Prevention (CDC) Advisory Committee on Immunization Practice (ACIP) published a framework for discussing the need for enhanced vaccination. Through analysis of a number of recent real-world studies published, it was found that 3 Since the May Delta variants have appeared and spread rapidly in various countries, a decline in the VE of the COVID-19 vaccine has been observed (Figure 1)1.
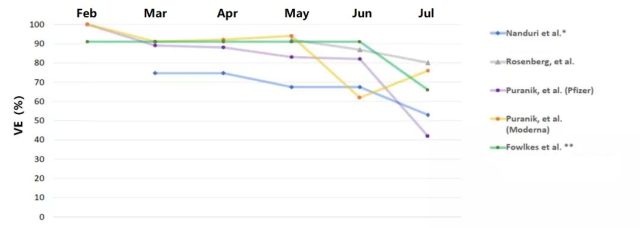
Figure 1 Vaccine VE changes over time in different studies
The CDC’s discussion framework also pointed out that before the Delta mutant strain became the main virus strain in the US epidemic, the VE could reach 87% or higher. After the Delta mutant strain appeared, the VE for infection or symptomatic disease dropped to 39. %~84%, the VE for hospitalization or severe illness also dropped to 75%~95%1 (Figure 2).
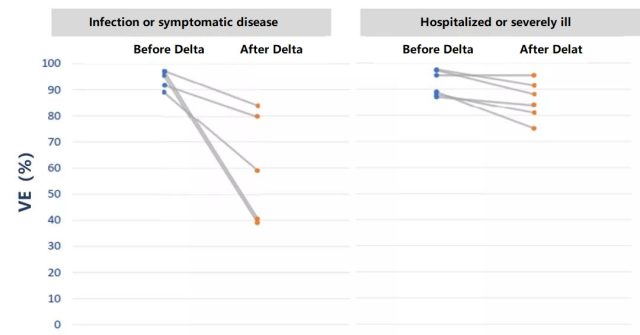
Figure 2 VE before and after the appearance of the Delta mutant
Real-world studies for different strains also found that compared with Alpha mutants, the VE for Delta mutants has a certain degree of decline (Figure 3).
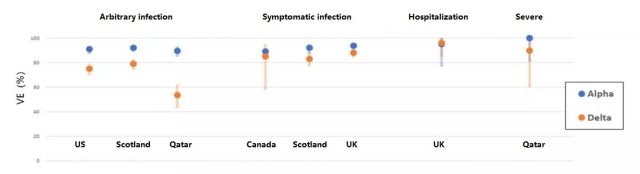
Figure 3 VE of Alpha mutant and Delta mutant
Is the drop in VE caused by the Delta mutant?
Although the reduction in VE of the COVID-19 vaccine after the delta variant has been observed in the real world, it cannot be easily concluded that the reduction in VE of the COVID-19 vaccine is caused by Delta. Many other factors may affect VE. Evaluation of the population, such as population characteristics, time of immunization, changes in variant strains, the interval between two doses1, etc.
In order to further clarify the influence of Delta mutant strains, a number of recent studies have explored the reasons for the decline in VE before and after the Delta mutant strains are prevalent:
On October 11, 2021, Nature published a study 2 that analyzed the effectiveness of mRNA vaccines against the current 16 epidemic variants. It compared the immune response within 70 days after mRNA vaccination and evaluated the neutralizing titer PRNT50. The results of the study showed that the neutralization titer of the vaccinated serum gradually decreased over time after the second dose, but it was still higher than the serum neutralization titer after a single vaccination. So is the neutralization titer of the mainstream Delta mutant strains among the various mutant strains the lowest?
Research on the ranking of vaccine immune escape shows that among the worrying variants (VOC, variant of concern), the degree of immune escape from low to high is Alpha<Delta<Gamma<Beta, and the PRNT50 of Delta variants after vaccination is higher than Gamma, Beta variants. This shows that for vaccines, the immune escape of the Delta variant is limited. According to the research data, for the Delta mutant strain, the researchers predict that the vaccine can provide protection for most vaccinators, and the increase in breakthrough infections associated with the mutant strain is more likely to be related to its high infectivity 3-6.
On October 4, 2021, a real-world study of over 3.43 million people in the United States published in The Lancet7 showed the effectiveness of preventing COVID-19-related hospitalizations within 6 months of full vaccination of BNT162b2 90% (95% CI 89%-92%), the total effectiveness of preventing SARS-CoV-2 infection is 73% (95% CI 72%-74%), of which the effectiveness in the first month is 88% , The effectiveness after 5 months is 47%.
From the perspective of different variants, within 1 month after full vaccination, the estimated VE values for preventing the infection of Delta variants and other variants are very high, respectively, 93% and 97%. Four months after full vaccination, the VE against Delta infection dropped to 53%, and the VE against other variant strains dropped to 67% (Figure 5). There was no significant difference in the decrease of VE of different variants (P=0.30). The author believes that this change in the effectiveness of the vaccine in preventing infection is mainly due to the weakening of its effectiveness, not due to the immune escape of the Delta mutant strain.
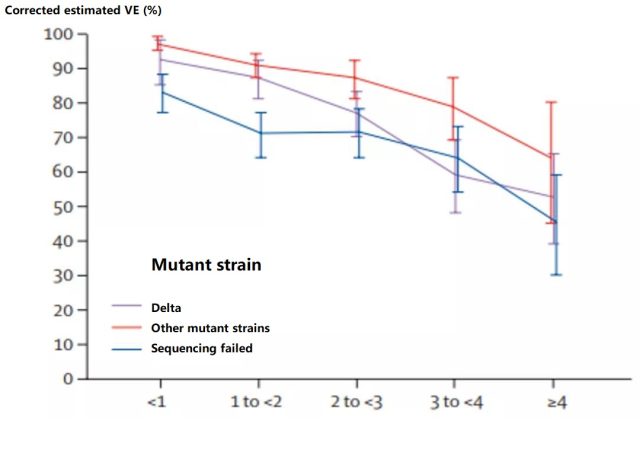
Figure 5 Estimated VE for different variants of SARS-CoV-2 infection
A preprint paper 8 was published on September 30, 2021, using open data during the period when the prevalence of Delta variants in 13 regions of the United States went from basically zero to nearly 100% (2021.5.15-9.15), and found that despite the Delta mutation The strain gradually became popular, but the VE of almost all regions maintained a fairly high level, with an overall average VE of 0.841. According to different time periods, the value of VE starts from around 0.9 in mid-May, drops to around 0.76 in mid-July, and then rises to around 0.9 in mid-September.
During this time, younger and healthier people are vaccinated, which in principle will increase the VE of the vaccine. This effect may be related to the increase in VE after July 15. This result suggests that the change in VE seems to be driven by demographic factors that affect vaccination, especially demographic factors related to age distribution. Based on the analysis of these data, the author believes that the Delta variant has minimal impact on VE.
So what are the main factors leading to the decline in VE? Many studies have found that the level of antibodies induced by vaccines decreases over time. A preprinted paper on September 17, 2021 provides direct evidence of the link between the decline in VE and the decline in antibody levels. Studies have shown that the antibody titer produced by the COVID-19 vaccine gradually decreases over time, and the decrease in titer is associated with an increase in the risk of infection. The study used data from a large Israeli non-profit health maintenance organization (HMO)9 to analyze 8,395 people who were fully vaccinated with the BNT162b2 vaccine and tested for IgG antibody levels between January and July 2021, aiming to understand vaccination. Effectiveness after 6 months.
The study found that the level of IgG antibodies in the fully vaccinated population gradually decreased over time (1 month vaccination vs 6 months vaccination: 14008 vs 1411, P<0.001). The IgG level is negatively correlated with the risk of infection. Those with an IgG serum level <300 AU/ml are more likely to develop infection. Specifically, when the IgG serum level is <150 AU/ml, polymerase chain reaction (PCR) detection of the new coronavirus The positive rate was 1.2%. When the IgG serum level was 150-299 AU/ml, the PCR positive rate was 1.3%, and when the IgG serum level was 300-799 AU/ml, the PCR positive rate was only 0.2%. In addition, excluding the influence of factors such as age (the first batch of vaccinated people are more likely to be older), the first batch of vaccinated people are 1.6 times more likely to be infected with CoVID-19 than those who are vaccinated later.
The way to deal with it: strengthen immunity and revitalize VE
Although the Delta mutant strain is extremely infectious, it quickly becomes the mainstream wherever it goes. However, it can be seen from recent studies that the Delta variant strain has limited immune escape to the vaccine and is not the main reason for the decline in VE.
The decrease in VE is mainly due to the attenuation of neutralizing antibodies induced by the vaccine over time after vaccination. Therefore, increasing the level of antibodies induced by intensified needles as a possible countermeasure has become a hot spot in the current research on immunization strategies.
Both mRNA vaccines and inactivated vaccines have undergone clinical trials of booster injections at all ages 10-12. Studies have shown that booster injections can significantly increase antibody levels and are safe to tolerate.
On October 21, 2021, Pfizer and BioNTech released the protection data for the first clinical trial of the third dose of COVID-19 vaccine. The protective power of BNT162b2 after the third dose inoculation was as high as 95.6%, and this protective power was mainly against the 13 of the Delta mutant strain.
Israel released the real-world research data of booster injection on August 31, 2021.14 It also shows that after the third dose of BNT162b2 mRNA vaccine booster injection for 12 days or more, the body neutralizing antibody level is compared with only two injections. Increased by 10 times, the relative risk of confirmed infection was reduced by 11.4 times, and the relative risk of severe illness was reduced by 15.5 times.
Summary
Existing data indicate that the Delta variant strain has limited immune escape to the vaccine, which is not the main reason for the decline in the effectiveness of the vaccine.
The decrease in VE is more due to the gradual attenuation of neutralizing antibodies produced by the vaccine over time, and the intensified needle strategy has also been proven to be an effective way to deal with the Delta variant. With the advent of winter, it is necessary to further promote the full coverage of vaccination and to promote intensified vaccination in an orderly manner. At the same time, strict public health measures are also indispensable.
The current trend of the new coronavirus pandemic is still continuing. As long as the new coronavirus is spreading, it may replicate in large numbers and produce new mutations.
Therefore, it is still necessary to strengthen the monitoring of new coronavirus mutations; in addition, strengthen the long-term effectiveness of needle protection, and Whether the emergent new mutant strains can maintain their effectiveness also requires continuous attention.
The struggle between humans and the COVID-19 virus still has a long way to go.
references: Is the reduced effectiveness of COVID-19 vaccines really due to Delta variants?
1.https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-08-30/09-COVID-Oliver-508.pdf.
2. Carolina Lucas, Chantal B F Vogels, Inci Yildirim, et al. Impact of circulating SARS-CoV-2 variants on mRNA vaccine-induced immunity Nature. 2021 Oct 11. DOI: 10.1038/s41586-
https://www.cdc.gov/vaccines/acip/index.html
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



