What is the most successful pathogen known to the scientific community?
- Statins Lower Blood Lipids: How Long is a Course?
- Warning: Smartwatch Blood Sugar Measurement Deemed Dangerous
- Mifepristone: A Safe and Effective Abortion Option Amidst Controversy
- Asbestos Detected in Buildings Damaged in Ukraine: Analyzed by Japanese Company
- New Ocrevus Subcutaneous Injection Therapy Shows Promising Results in Multiple Sclerosis Treatmen
- Dutch Man Infected with COVID-19 for 613 Days Dies: Accumulating Over 50 Virus Mutations
What is the most successful pathogen known to the scientific community?
- Red Yeast Rice Scare Grips Japan: Over 114 Hospitalized and 5 Deaths
- Long COVID Brain Fog: Blood-Brain Barrier Damage and Persistent Inflammation
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
What is the most successful pathogen known to the scientific community? Nature: It has evolved an amazing invasion mechanism.
Compared with the new coronavirus that is still raging around the world, as well as familiar viruses such as HIV and hepatitis B, the herpes virus seems to be a little low-key.
However, their behavior is not at all low-key and can be said to be the most successful pathogen known to the scientific community.
Herpes virus is a kind of DNA virus. There are 8 species in its family that can cause human diseases. Herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2) are typical representatives.
Humans are the natural host of herpes simplex virus. Infections are extremely common in the population.
80% to 90% of the initial infections are recessive infections. Most of them have no obvious symptoms, and only a few are overt infections.
The common clinical manifestations are mucosal or skin localization. Herpes.
After the initial infection, it often turns into a latent infection, which can cause recurrence after being exposed to external stimuli.
According to data from the World Health Organization (WHO) , HSV-1 has been lurking in nearly 70% of the world’s human body, and the number of infected people under the age of 50 reached 3.7 billion in 2016.
What is frustrating is that the herpes virus will remain latent in the peripheral nervous system of the host for life and will never be eradicated. So it is ” one kiss for life “: once you carry it, you have it for life .
Therefore, it is urgent to understand how the herpes virus invades the nervous system in order to make it possible to develop prevention strategies.
On November 18, 2021, researchers from Northwestern University published a research paper titled: Herpesviruses assimilate kinesin to produce motorized viral particles in Nature .
The study discovered the cunning strategy of herpes virus infecting the nervous system, further revealed the molecular mechanism of the virus evolution, and opened up for the development of vaccines against herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2) . the way. At the same time, this discovery may have a broad impact on many viruses, including the new coronavirus and HIV.

Throughout the life cycle, some herpes virus carriers may never have a dominant infection; but for others, their peripheral nervous system will occasionally experience recurrent infections.
In severe cases, the virus may also invade the central nervous system. System, this situation may cause blindness or life-threatening encephalitis. More and more evidence shows that herpes virus may also drive the occurrence of dementia.
The primary infection of herpes simplex virus type 2 (HSV-2) is mainly sexually transmitted, causing genital herpes, which is manifested as blisters on the genital area, which rupture and form ulcers. Complications include extragenital injury and aseptic meningitis.
A few primary infections can also be caused by HSV-1. HSV-2 can also be passed from mother to newborn as neonatal herpes during childbirth, manifesting as baby’s systemic lesions.
Most babies can recover, but in the worst case, it can cause brain damage or spread through all organs and eventually lead to death.
Therefore, there is an urgent need for a vaccine to prevent the herpes virus from invading the nervous system.
In this new study, the research team discovered how the herpes virus hijacked a protein from epithelial cells and “instigated it” to help it enter the peripheral nervous system. They call this process “assimilation”.
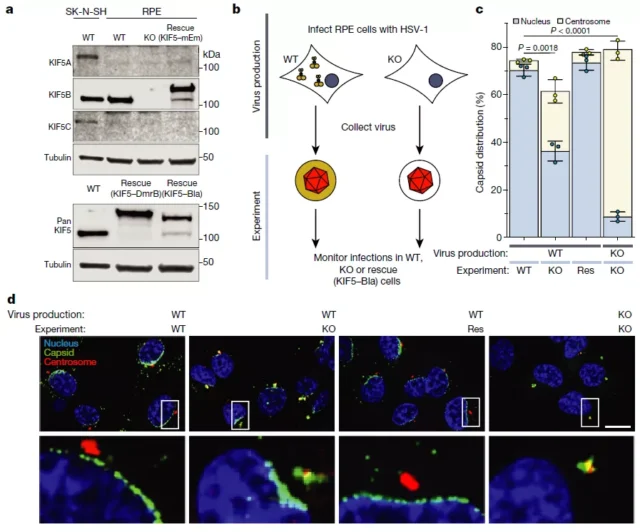
The virus needs to inject its genetic code into the nucleus so that it can begin to produce more herpes viruses. They reprogram the cell to make it a virus factory. But the biggest question is how do they reach the nucleus of the neuron?
Like many viruses, the herpes virus also uses microtubules. Microtubules are fibrous structures that exist in cells that connect different areas and are responsible for maintaining cell shape and transporting substances.
The herpes virus jumps on the orbits of microtubules and uses dynein and kinesin as its engines to move along the microtubules.
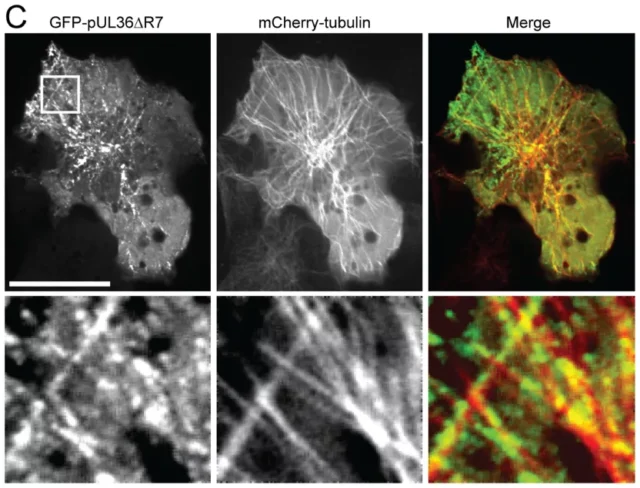
We can think of the cell as a train station. All tracks lead to a hub called the centrosome. Dynein and kinesin are the engines of two types of trains.
One of them leads to the hub (central body), and the other drives away from the center to the suburbs.
When a typical virus such as influenza infects mucosal epithelial cells, the virus grabs these two engines and moves back and forth on the microtubule bundle until it finally reaches the nucleus.
The distance from the suburbs to the nucleus through the centrosome is very short.
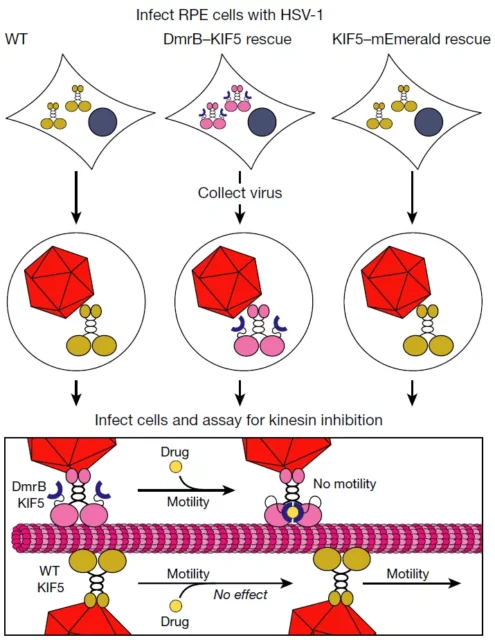
However, traveling along the nerves is equivalent to a transnational trip. The herpes virus jumped onto the “power train” (dynein engine) during this trip , and it also ensured that the protein engine would not bring it back to the “country of departure.” The researchers said that it may take 8 hours from the end of the neuron to the center.
But the dynein engine cannot take it farther than the centrosome, and the herpes virus “is determined to get it” to reach the nucleus.
At this time, it reached into its “pocket”, took out the kinesin engine it hijacked from mucosal epithelial cells, and “assimilated” it to become part of its team.
In this betrayal, this assimilated kinesin transported the herpes virus directly to the nucleus.
It is worth noting that the kinesin used by the herpes virus (HSV-1) is not endogenous to neurons, but is derived from previously infected epithelial cells from which viral particles are produced .
In general, the trapping and carrying of kinesins by virus particles between cells increases the possibility of HSV-1 reusing the captured kinesins to infect cells (including neurons) .
Corresponding author Gregory Smith said that by understanding how viruses achieve this incredible operation, it is now possible to consider how to take away their ability to invade the nervous system.
If we can prevent it from assimilating kinesin, we will have a virus that cannot infect the nervous system. It will be possible to develop preventive vaccines.
He added that this is the first time that a virus has been discovered to reuse a cell protein and then use them to drive subsequent infections, and he was very happy to further discover the molecular mechanisms that these viruses have evolved, making them the most successful pathogens known to the scientific community.
Paper link:
https://www.nature.com/articles/s41586-021-04106-w
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



