Are the side effects of statins really serious?
- Aspirin: Study Finds Greater Benefits for These Colorectal Cancer Patients
- Cancer Can Occur Without Genetic Mutations?
- Statins Lower Blood Lipids: How Long is a Course?
- Warning: Smartwatch Blood Sugar Measurement Deemed Dangerous
- Mifepristone: A Safe and Effective Abortion Option Amidst Controversy
- Asbestos Detected in Buildings Damaged in Ukraine: Analyzed by Japanese Company
Are the side effects of statins really serious?
- Red Yeast Rice Scare Grips Japan: Over 114 Hospitalized and 5 Deaths
- Long COVID Brain Fog: Blood-Brain Barrier Damage and Persistent Inflammation
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
EHJ: Are the side effects of statins really serious? The data of 4 million people confirms that the problem of statin intolerance is overestimated.
Cardiovascular disease (CVD) not only has a high prevalence, but also has a high mortality rate, with 2 out of every 5 deaths due to CVD [1].
Luckily we have statins to contend with. A large number of studies have confirmed that statins can significantly reduce the risk of CVD in high, intermediate and even low-risk groups, and reduce atherosclerosis-related disability and death [2,3], which can be said to be the leader of the CVD prevention and treatment community. .
The fly in the ointment is that, according to different studies, 2% to 50% of people are intolerant to statins, and they will experience adverse reactions such as muscle discomfort, neurocognitive impairment, and elevated alanine aminotransferase after taking statins [4-7]. If the drug is reduced or stopped as a result, the risk of CVD may spike again.
Before solving this thorny problem, the researchers first questioned the accuracy of the statin intolerance rate from the source, because the intolerance rate between different studies is too different, and it cannot be simply explained by the difference in the study population.
It is very likely that there are cases where rates of statin intolerance are underestimated or overestimated .
To this end, Maciej Banach and a group of experts conducted a meta-analysis of the statin intolerance rate of more than 4 million study subjects in 176 studies around the world.
The results showed that the statin intolerance rate was 9.1%.
In addition, they found some factors that were significantly associated with statin intolerance, such as advanced age, female sex, Asian and African descent, obesity, diabetes, hypothyroidism, chronic liver disease, renal failure, antiarrhythmic drugs, calcium channel blockade drugs, alcohol, etc.
The results were published in the European Heart Journal, an authoritative journal in the field of CVD [8].

Screenshot of the paper’s homepage
This meta-analysis was conducted by the Lipid and Blood Pressure Meta-Analysis Collaborative Working Group (LBPMC) and the International Lipid Experts Group (ILEP).
ILEP is composed of nearly 90 experts representing societies and research groups in more than 50 countries.
The researchers found a total of 3596 relevant studies.
After excluding studies that did not meet the criteria, such as the sample size of less than 100 people, the follow-up time of less than 6 weeks, and the absence of the definition of statin intolerance, there were finally 112 randomized controlled trials and 64 cohort studies.
More than 4 million study subjects were included in the analysis. The mean age of the study subjects was 60.5 years, 40.9% were female, and the mean follow-up was 19±7.3 months.
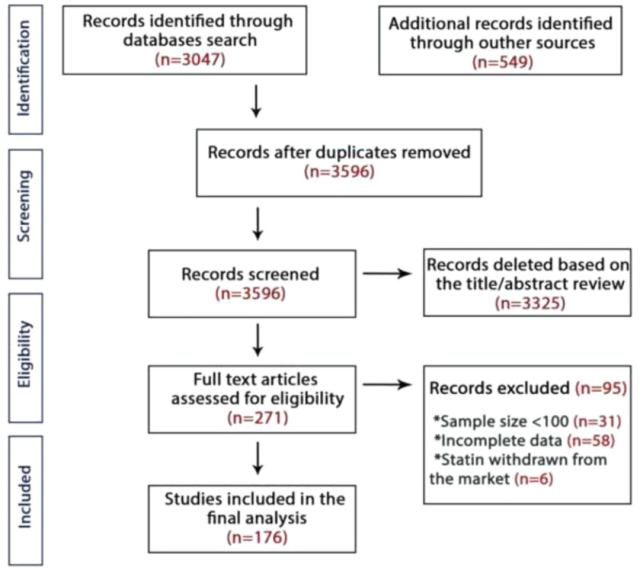
Study Screening Process
The primary endpoint of the study was the overall rate of statin intolerance and the rate of statin intolerance based on different diagnostic criteria, and the secondary endpoints were the rate of statin intolerance in patients with different diseases and the influencing factors of statin intolerance.
What did the meta-analysis find? Let’s take a look at it in detail.
One is that the rate of statin intolerance is overestimated .
Different professional organizations define statin intolerance differently, which undoubtedly affects estimates of statin intolerance rates. But the researchers found that statin intolerance rates were less than 10 percent regardless of the organization’s definition .
Second, the statin intolerance rate in different application scenarios may be different.
The rate of statin intolerance in the cohort study was higher than that in the randomized controlled study (17% vs 4.9%). This is related to the difficulty in correctly diagnosing statin intolerance in clinical practice, and also suggests that the occurrence of statin intolerance in the real world may be overestimated .
The rates of statin intolerance in primary and secondary prevention were comparable at 8.2% (95% CI: 6%-10%) and 9.1% (95% CI: 6%-11%), respectively.
However, in cohort studies that included both primary and secondary prophylaxis, the statin intolerance rate was 18% (95% CI: 14%-21%), suggesting that such observational studies may overestimate statin intolerance Case.
Intolerance rates were 9%, 12%, 13%, and 6% in patients with a family history of hypercholesterolemia, hypercholesterolemia, dyslipidemia, and type 2 diabetes mellitus for primary CVD prevention with statins, respectively ;
stable Intolerance rates in patients with coronary heart disease, acute coronary syndrome, myocardial infarction, and stroke/transient ischemic attack were 8%, 13%, 13%, and 5.4%, respectively, when using statins for CVD secondary prevention.
Intolerance rates were roughly similar between hydrophilic and lipophilic statins (5% vs 4%) .
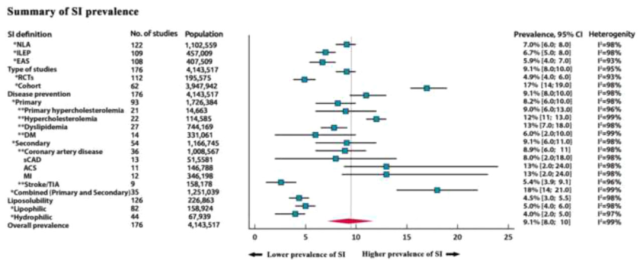
Rates of statin intolerance in different situations
Who is more likely to develop statin intolerance?
- Using regression models, the researchers found some factors that were significantly associated with statin intolerance, including:
- Demographics: Age ≥ 65 years, female, Asian and African
- Concomitant diseases: obesity, diabetes, hypothyroidism, chronic liver disease, chronic renal failure
- Drug interactions: calcium channel blockers, antiarrhythmic drugs, high-dose statins
- Habits: Drinking alcohol, exercising
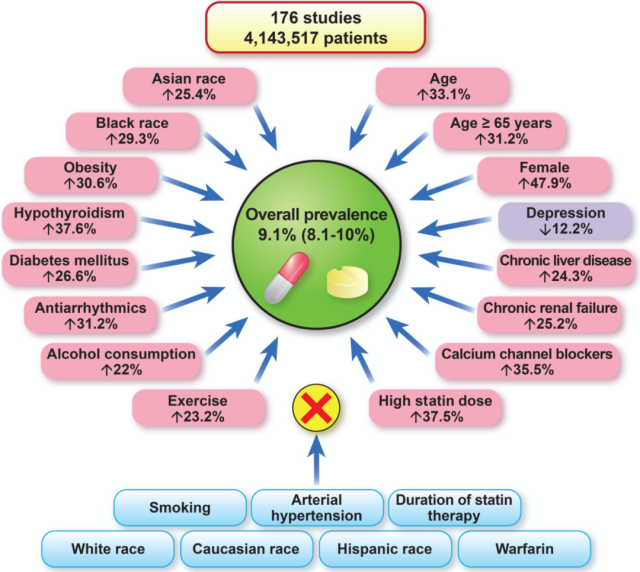
Factors influencing statin intolerance
Why are statin intolerance rates overestimated?
Possibly the nocebo effect . The so-called nocebo effect means that some patients have a negative attitude towards treatment measures, such as not believing that the treatment is effective or thinking that the side effects of the drug are serious, and related psychological factors may increase the risk of physical discomfort and perception, and even worsen the condition [9] .
As early as May 2017, the results of the ASCOT-LLA trial published in The Lancet already suggested the nocebo effect of statins.
The study found that the rate of muscle-related adverse events in the statin group was higher than that in the placebo group only in the unblinded state, when the patient and the physician knew that the patient was taking a statin, but not in the blinded state. It is suggested that the high rate of statin intolerance may be due to the nocebo effect [10].
This large global meta-analysis also points to this effect, and the findings will help physicians and patients more objectively view statin intolerance rates and the risks and benefits of statin therapy for CVD.
Readers and friends who take statins, don’t have too strong psychological presuppositions about the side effects of drugs~
References:
[2] Cardiovascular Branch of Chinese Medical Association, Cardiac Prevention and Rehabilitation Professional Committee of Chinese Rehabilitation Medicine Association, Cardiac Professional Committee of Chinese Gerontology and Geriatrics Association, etc. Guidelines for Primary Prevention of Cardiovascular Diseases in China [J]. Zhonghua Heart Chinese Journal of Cardiovascular Diseases, 2020, 48(12):1000-1038. [3] Guidelines for the Prevention of Cardiovascular Diseases in China (2017)[J]. Chinese Journal of Cardiovascular Diseases, 2018, 46(1): 10-25.
[4] Banach M, Stulc T, Dent R, et al. Statin non-adherence and residual cardiovascular risk: There is need for substantial improvement[J]. International Journal of Cardiology, 2016:184-196.
[5] Banach M, Mikhailidis D P. Statin Intolerance: Some Practical Hints[J]. Cardiology Clinics, 2018:225-231.
[6] Eagle K A, Kline-Rogers E, Goodman S G, et al. Adherence to evidence-based therapies after discharge for acute coronary syndromes: an ongoing prospective, observational study[J]. American Journal of Medicine, 2004, 117(2):73-81.
[7] Kamal-Bahl S J, Burke T, Watson D, et al. Discontinuation of Lipid Modifying Drugs Among Commercially Insured United States Patients in Recent Clinical Practice[J]. American Journal of Cardiology, 2007, 99(4):530-534.
[8] Ibadete B, Penson PE, Mikhailidis DP, et al. Prevalence of statin intolerance: a meta-analysis[J]. European Heart Journal , 2022 .
[9] Beauregard, Mario. Brain Wars The Scientific Battle over the Existence of the Mind and the Proof That Will Change the Way We Live Our Lives. Canada: HarperCollins. 2012.
[10] Gupta A, Thompson D, Whitehouse A, et al. Adverse events associated with unblinded, but not with blinded, statin therapy in the Anglo-Scandinavian Cardiac Outcomes Trial-Lipid-Lowering Arm (ASCOT-LLA): a randomised double-blind placebo-controlled trial and its non-randomised non-blind extension phase[J]. Lancet, 2017:2473.
Are the side effects of statins really serious?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



