Researchers found double advantage of ‘killer’ T cells in preventing cancer cell metastasis
- EPA Announces First-Ever Regulation for “Forever Chemicals” in Drinking Water
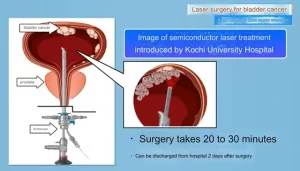
- Kochi University pioneers outpatient bladder cancer treatment using semiconductor lasers
- ASPEN 2024: Nutritional Therapy Strategies for Cancer and Critically Ill Patients
- Which lung cancer patients can benefit from neoadjuvant immunotherapy?
- Heme Iron Absorption: Why Meat Matters for Women’s Iron Needs
- “Miracle Weight-loss Drug” Semaglutide Is Not Always Effective
Researchers found double advantage of ‘killer’ T cells in preventing cancer cell metastasis
- Red Yeast Rice Scare Grips Japan: Over 114 Hospitalized and 5 Deaths
- Long COVID Brain Fog: Blood-Brain Barrier Damage and Persistent Inflammation
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Researchers found double advantage of ‘killer’ T cells in preventing cancer cell metastasis.
A team of scientists from the University of Geneva has demonstrated how “killer” T cells used in immunotherapy to eliminate cancer cells can also destroy the lymphatic vessels of tumors, greatly reducing the risk of metastasis.
Harnessing this synergistic effect could improve the treatment of cancers important for lymphangiogenesis, such as colorectal cancer, melanoma or breast cancer.
These results by researchers at the University of Geneva have been published in Science Advances .
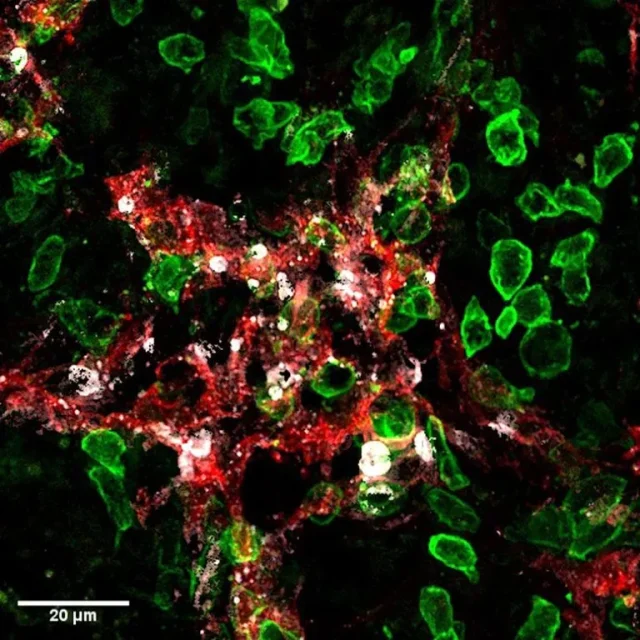
“Killer” T cells (also known as cytotoxic T cells or cytotoxic T lymphocytes) are immune cells that kill certain cells, such as foreign cells, cancer cells, and cells infected with viruses.
“Killer” T cells can be isolated from other blood cells, grown in the lab, and injected into patients to kill cancer cells. “Killer” T cells are a type of white blood cell and a type of lymphocyte.
The lymphatic system is the main way cancer cells spread in the body. They first colonize sentinel lymph nodes and then move elsewhere in the body to produce secondary metastases.
So far, however, therapies that block tumor lymphangiogenesis have been disappointing.
“In fact, they also represent a pathway by which some immune cells (dendritic cells) leave the tumor and activate anti-tumor-killer T cells,” said the Department of Pathology and Immunology of the UNIGE Faculty of Medicine and the Geneva Inflammation Research Center, which led the work. Associate Professor Stéphanie Hugues explained. “Therefore, we had to find a balance in which to inhibit this mechanism without completely blocking it, in order to decipher its mode of action in detail.”
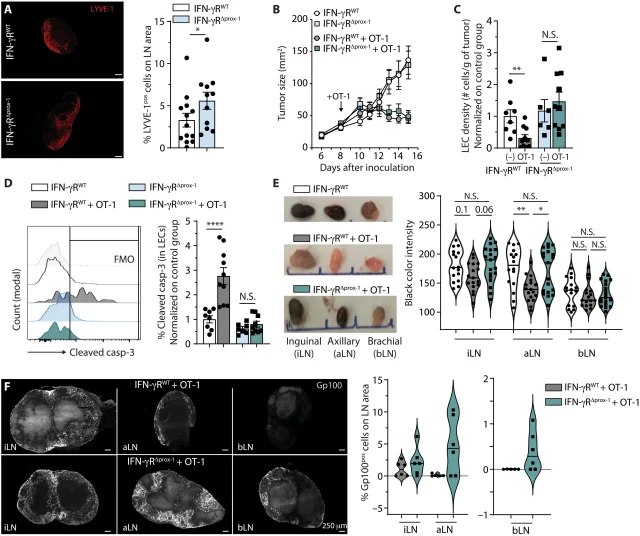
Identify a unique target
To do this, the scientists used so-called “killer” T lymphocytes used in immunotherapy regimens. Laure Garnier, a junior lecturer in the lab of Stéphanie Hugues and first author of the work, explains: “These T cells are immune cells that are specifically activated in the laboratory to eliminate tumor cells before they are injected into the patient. Here , we injected them into mice with melanoma. If the killer lymphocytes destroyed the tumor cells, as expected, they also attacked the lymphatic endothelial cells in the lymphatic vessels.”
Indeed, the destruction of cancer cells results in the release of tumor antigens.
These small cancerous segments are then captured by lymphatic endothelial cells, which, after becoming carriers of tumor-recognition markers, are also recognized as enemies by the T cells that attack them.
Thus, this mechanism disrupts the tumor-associated lymphatic system, greatly reducing the risk of metastasis, without completely blocking it.
The team confirmed these results with other methods, such as vaccinations aimed at boosting the immune system. “We also observed destruction of lymphatic endothelial cells and thus reduced lymph node metastases, limiting the risk of secondary metastases. Furthermore, since this effect occurs only in the tumor microenvironment, there is no concern about systemic effects. ,” emphasized Laure Garnier.
Increase synergy by choosing the right weapon
How can this effect be enhanced without impairing the action of immune cells, which need to travel through lymphatic vessels to enter tumors?
There are several options, such as intervening after immunity is established, or in combination with a treatment regimen, because the immune system is so strong that limiting lymphangiogenesis does not impair its function.
Stéphanie Hugues said: “Nevertheless, our results suggest that the most effective approach is to use killer T cells that have been generated in the laboratory and therefore ready to attack to bypass the first-stage activation, which may prove to be useful. questionable.”
Immunotherapy remains complex and is only used when conventional treatments have proven ineffective.
“Even if they are very promising, these therapies are not miraculous solutions and often cause severe side effects. This is why we want to understand the smallest biological processes at work,” the authors conclude.
Researchers found double advantage of ‘killer’ T cells in preventing cancer cell metastasis
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.