Types of COVID-19 Vaccines
Types of COVID-19 Vaccines
Types of COVID-19 Vaccines. At present, there are 5 routes to develop COVID-19 vaccines. In addition to adenovirus vector vaccines and inactivated vaccines that have entered clinical trials, vaccines of the other three technical routes are also entering clinical trials. What are the characteristics of these 5 vaccines?
1. Inactivated vaccine
Inactivated vaccines are the most traditional and classic technical route: culture the new coronavirus in vitro, and then inactivate it to make it non-toxic, but the “corpses” of these viruses can still stimulate the body to produce antibodies and make immune cells remember the virus appearance. At present, three inactivated COVID-19 vaccines in China have entered clinical research. Among them, the inactivated COVID-19 vaccine developed by Wuhan Institute of Biological Products has entered Phase II clinical research.
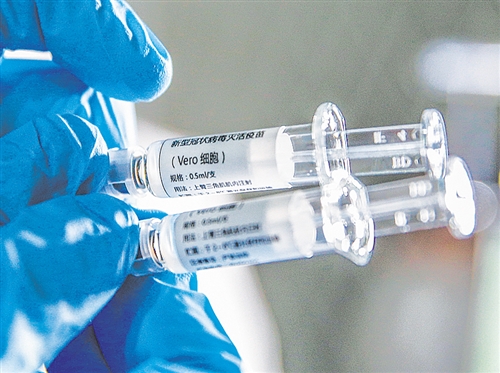
The advantages of inactivated vaccines are that the preparation method is simple and fast, and the safety is relatively high. It is the usual means to deal with the transmission of acute diseases. Inactivated vaccines are very common. The commonly used hepatitis B vaccines, inactivated polio vaccines, inactivated Japanese encephalitis vaccines, and DPT vaccines in China are all inactivated vaccines.
However, inactivated vaccines also have shortcomings, such as large doses, short immune periods, and single immune pathways. The most terrible shortcomings are that they sometimes cause antibody-dependent enhancement effects (ADE) and aggravate viral infections. Serious adverse reactions leading to the failure of vaccine development.
2. Adenovirus vector vaccine
The adenovirus vector vaccine uses modified and harmless adenovirus as a carrier, loaded with the S protein gene of the new coronavirus to make an adenovirus vector vaccine to stimulate the body to produce antibodies. The S protein is the key “key” for the new coronavirus to invade human cells. The harmless adenovirus wears the “hat” of the S protein and pretends to be “fierce” to make the body produce immune memory. The COVID-19 vaccine that Academician Chen Wei’s team is conducting phase II clinical trials is an adenovirus vector vaccine, which is a relatively mature vaccine technology route.
The advantages of adenovirus vector vaccines are: safety, high efficiency, and fewer adverse reactions. This vaccine has a successful precedent: Previously, the recombinant Ebola virus disease vaccine independently developed by the team of Academician Chen Wei and Tianjin Cansino Biotechnology Co., Ltd. also used adenovirus as a vector.
This vaccine also has shortcomings. The development of recombinant viral vector vaccines needs to consider how to overcome “pre-existing immunity”. Take the recombinant new coronavirus vaccine that entered clinical trials as an example. This vaccine uses type 5 adenovirus as a carrier, but most people have been infected with type 5 adenovirus during their growth. There may be antibodies in the body that can neutralize the adenovirus vector, so It may attack the vector and reduce the effect of the vaccine. In other words, the safety of the vaccine is high, but the effectiveness may be insufficient.
3. Nucleic acid vaccine
Nucleic acid vaccines include mRNA vaccines and DNA vaccines, which directly inject genes encoding S protein, mRNA or DNA into the human body, and use human cells to synthesize S protein in the human body to stimulate the body to produce antibodies. In layman’s terms, it is equivalent to handing over a detailed virus file to the body’s immune system. The mRNA COVID-19 vaccine approved by Moderna of the United States for Phase II clinical trials is a nucleic acid vaccine.
The advantages of nucleic acid vaccines are: no need to synthesize proteins or viruses during development, simple process and relatively high safety. Nucleic acid vaccines are new technologies for vaccine research and development that are actively being explored all over the world, and there is currently no nucleic acid vaccine on the market. Some high-level corrections in China are conducting research on this route.
The technology of this vaccine is too new and there is no successful precedent, so I don’t know where there may be a pit in the development process! From an industrial point of view, although the production process itself is not complicated, most countries in the world have a relatively weak foundation in this field, and a stable and controllable mass production supply chain has not yet been formed. So its shortcomings are: there is no successful precedent, most countries cannot produce on a large scale, and it may be difficult to spread to low-income countries because of the high price.
4. Recombinant protein vaccine
Recombinant protein vaccine, also known as genetic engineering recombinant subunit vaccine. It uses genetic engineering methods to mass-produce the S protein, which is most likely to be an antigen of the new coronavirus, and inject it into the human body to stimulate the body to produce antibodies. It is equivalent to not producing a complete virus, but separately producing the key components of many new coronaviruses and handing them to the body’s immune system. China has mastered the large-scale production of high-quality and high-purity vaccine protein technology, which is a technical route that can quickly produce vaccines on a large scale.
The advantages of recombinant subunit vaccines are: safety, high efficiency, and large-scale production. This route has a successful precedent, and the more successful genetic engineering subunit vaccine is the hepatitis B surface antigen vaccine.
The disadvantage of recombinant subunit vaccines is that it is difficult to find a good expression system. Its antigenicity is affected by the selected expression system, so the expression system needs to be carefully selected when preparing the vaccine.
5. Attenuated influenza virus vector vaccine
The attenuated influenza virus vector vaccine uses an attenuated influenza virus vaccine that has been approved for marketing as a carrier, carrying the S protein of the new coronavirus, and co-stimulating the human body to produce antibodies against the two viruses. Simply put, this vaccine is a fusion virus formed by the low-toxicity influenza virus wearing the COVID-19 virus S protein “cap”, which can kill two birds with one stone, and can prevent influenza and COVID-19. When the epidemic of COVID-19 pneumonia overlaps with influenza, its clinical significance is very great. Since the attenuated influenza virus is easy to infect the nasal cavity, this vaccine can be vaccinated only by nasal drip.
The advantages of the attenuated influenza virus vector vaccine are: one vaccine prevents two diseases, less frequent vaccination, and simple vaccination method.
Live attenuated virus vaccines are a very important type of vaccine. The common live attenuated vaccines we usually have are: Japanese encephalitis live attenuated vaccine, hepatitis A live attenuated vaccine, and measles live attenuated vaccine. But the disadvantage of live attenuated vaccines is that the development process is long.
It should be noted that this technical route does not directly attenuate the new coronavirus into a vaccine, because it requires long-term virus culture and passage attenuation and screening; it uses an attenuated influenza virus vaccine as a carrier. , The disease-causing S protein of the new coronavirus is transferred to the attenuated influenza virus vaccine through bioengineering methods, so that a large amount of virus culture, passage, attenuation and screening time can be saved.
What is the difficulty in vaccine development?
The research and development of the COVID-19 pneumonia vaccine faces many difficulties and obstacles.
Difficulty one: recognize new virus
To defeat a new virus, scientist must first recognize and understand it. The new coronavirus is the third coronavirus that has caused large-scale human infections through cross-species transmission in the past 18 years. The previous two are SARS and MERS.
Research experience on similar viruses can help us better understand new virus. Regrettably, no vaccines and drugs have been developed for a certain type of coronavirus so far, and neither SARS nor MERS have specific drugs or successfully marketed vaccines. Compared with other viruses, we still know little about the biological characteristics, infection process, pathogenicity of the new coronavirus, and the immune response of the human body to it. It will take us a lot of time to understand the new coronavirus in depth.
However, SARS and MERS have improved our understanding of the coronavirus. After the outbreak, Chinese scientists quickly completed the new coronavirus gene sequencing and strain isolation, laying a solid foundation for vaccine research and development.
Difficulty 2: The virus will transform
The new coronavirus is a highly glycosylated RNA virus, which means it is easy to transform and cause the vaccine to fail.
Glycosylation is a widespread, complex and changeable protein post-translational modification that plays an important role in cells and the body. Some scholars have compared the glycosylation sites of common enveloped viruses: hepatitis C virus has 4 to 11 glycosylation sites, influenza virus has 5 to 11 glycosylation sites, and Ebo Pull virus has 8 to 15 glycosylation sites, and HIV has as many as 20 to 30 glycosylation sites.
These glycosylation sites make the virus prone to a variety of mutations. After the virus is glycosylated, it is equivalent to using “disguise” disguise. The antibodies produced after the human body is injected with the vaccine may not be able to accurately identify the virus in the body, and it will not be able to prevent it. The glycosylation site of HIV is 3 to 6 times that of influenza virus, which is one of the main reasons why the development of AIDS vaccine has been delayed.
The latest research shows that the new coronavirus is a highly glycosylated spherical particle with a huge structure with at least 66 glycosylation sites! The glycosylation site of the new coronavirus is at least twice that of HIV, which also means that vaccine development is extremely difficult.
Difficulty three: Vaccine might be harmful to humans
The COVID-19 vaccine is a weapon for humans to deal with the virus, but the ADE effect may make this weapon in turn deepen the harm to humans. ADE means that when the body is infected by a pathogen, the original neutralizing antibody not only cannot prevent the virus from invading human cells, some viruses can reproduce or infect significantly with the assistance of specific antibodies, causing more serious pathological damage. The ADE effect has become one of the main obstacles in the decades of hard research and development of dengue vaccines.
Scientists have discovered the effect of ADE in primate experiments for the development of SARS vaccines: if monkeys are vaccinated with the “recombinant vaccinia-SARS vaccine” expressing the SARS virus spike protein and then infected with SARS virus, the acute lung injury will increase instead. . In view of the similar spike protein structure and infection mechanism of the new coronavirus and SARS virus, the new coronavirus vaccine also has the risk of ADE, and should be carefully concerned and studied in vaccine design.
However, there is good news in this regard recently. On May 6, Chinese scientists took the lead in publishing the animal experiment results of the new coronavirus vaccine in the top international academic journal “Science”: “Rapid Development of SARS-CoV-2 Virus Inactivated Vaccine”. Researchers have developed a purified inactivated new coronavirus vaccine candidate for use in animal experiments. Among them, 4 rhesus monkeys in the high-dose group had no virus detected in the throat, anus, and lungs, and no ADE was observed on the 7th day after infection.
In addition to the above three difficulties, there may be many unexpected difficulties in the development of COVID-19 vaccines that need to be overcome one by one, because no one can guarantee that vaccine development will be successful. HIV is an RNA virus. Vaccines have been developed since the 1980s and have been unsuccessful so far.
However, the development of Chinese COVID-19 vaccine is currently progressing smoothly, which makes people still very confident in the results of the research and development. Wang Junzhi, an academician of the Chinese Academy of Engineering, once clearly stated: Up to now, Chinese five major technical directions for vaccines are generally progressing smoothly. Chinese COVID-19 vaccine research and development progress is currently in the international advanced ranks and will not be slower than abroad.



