Structural heart disease: Definition Scope Surrent situation and Future
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Structural heart disease: Definition Scope Surrent situation and Future
Structural heart disease: Definition Scope Surrent situation and Future. At present, a variety of new devices and technologies for interventional treatment of structural heart disease are under development, and structural heart disease is showing a trend of flourishing and flourishing development.
Structural heart disease (SHD) is the fastest growing direction in the field of cardiovascular intervention in recent years. As new technologies for structural heart disease treatment continue to be produced and promoted throughout the world, the concept of structural heart disease has gradually become familiar to cardiology, other specialties and the public. However, the current academic community’s understanding of the definition and connotation of structural heart disease is still unclear. This article expounds the origin, definition and scope of the concept of structural heart disease, summarizes the development process and current situation of interventional therapy for structural heart disease, and prospects the development of structural heart disease.
1. The origin and scope of the concept of structural heart disease
In the published literature, no literature on the strict definition of structural heart disease has been consulted. In the non-public publication literature, the earliest lecture by Professor Martin Leon in the United States at the opening ceremony of the TCT (Transcatheter Cardiovascular Therapeutics) conference in 2001, when he classified the transcatheter technique, he first mentioned the structural heart The term disease.
At the 2005 CSI (Catheter Interventions in Congenital, Structural and Valvular Heart Disease) conference, Professor Horst Sievert of Germany formally proposed the concept of structural heart disease.
He pointed out: Structural heart disease refers to any abnormality of the heart structure, any disease related to the structure of the heart and large blood vessels; broadly structural heart disease refers to the structure of the heart in addition to the primary electrocardiographic disease and coronary artery disease. Abnormal diseases, that is, heart structural abnormalities that can be found by existing objective examinations such as echocardiography, magnetic resonance imaging, exercise stress test, endocardial biopsy, and autopsy; structural heart disease in a narrow sense refers to anatomical abnormalities that cause the heart Structural changes caused by physical and physiological changes in heart disease [1].
In the international literature, structural heart disease has another meaning, meaning organic heart disease, which is mainly used in the field of arrhythmia. It refers to the qualitative change of the heart generator relative to the change of cardiac function. Including coronary heart disease, cardiomyopathy, valvular disease, heart failure, etc.
Based on the current academic understanding and current technology development status, the author believes that structural heart disease refers to any disease related to the heart and the large blood vessel structure of the adjacent heart other than electrocardiographic disease and coronary artery disease. The treatment concept covers the correction or change of the heart Structure to treat the disease. The specific disease categories include (Figure 1):
(1) Congenital heart disease (ventricular septal defect, atrial septal defect, patent ductus arteriosus, tetralogy of Fallot, etc.);
(2) Heart valve disease (mitral valve, tricuspid valve, aortic valve, pulmonary valve, etc.);
(3) Cardiomyopathy (hypertrophic cardiomyopathy, dilated cardiomyopathy, etc.);
(4) Complicated with other diseases or exogenous cardiac structural abnormalities (ventricular septal perforation, ventricular aneurysm, iatrogenic atrial septal defect, etc.);
(5) Diseases or conditions that are complicated by other diseases that cause abnormal heart function and can be corrected by changing the cardiovascular structure (for example, atrial fibrillation leads to abnormal left atrial appendage function, and heart failure leads to abnormal heart function);
(6) Others: blood clots in the heart, heart tumors, pericardial diseases, etc.
In order to have separate divisions from the Vascular Surgery Specialty and the Pulmonary Vascular Specialty, the author suggests that in the current definition, diseases involving large blood vessels only include patent ductus arteriosus, Valsal’s sinus aneurysm rupture, main pulmonary artery window, etc. Diseases related to vascular structure, excluding diseases such as pulmonary vascular disease and aortic dissection. Structural heart disease treatment includes medication, surgery, and interventional therapy. At present, interventional therapy has become the most important development direction of structural heart disease. As far as the interventional treatment of structural heart disease is concerned, its technologies mainly include:
(1) Transcatheter closure of congenital heart disease;
(2) Traditional transcatheter valve therapy: mainly percutaneous balloon mitral valvuloplasty (PBMV), percutaneous balloon pulmonary valvuloplasty (PBPV), and percutaneous main Percutaneous balloon aortic valvuloplasty (PBAV), transcatheter paravalvular leak closure, etc.;
(3) Emerging transcatheter valve therapy: Transcatheter Aortic Valve Replacement (TAVR), Percutaneous pulmonary valve implantation (PPVI), transcatheter edge-to-edge mitral Transcatheter edge-to-edge mitral valve repair (TEER), transcatheter mitral valve implantation (TMVI), transcatheter tricuspid valve intervention, etc.
(4) Transcatheter left atrial appendage occlusion;
(5) Interventional treatment of cardiomyopathy: including alcohol ablation (Percutaneous transluminal septal myocardial ablation, PTSMA) or radiofrequency ablation of hypertrophic cardiomyopathy;
(6) Interventional treatment of heart failure: left ventricular volume reduction surgery, atrial shunt surgery, transcatheter ventricular assist devices, etc.
2. A brief history of the development of interventional therapy for structural heart disease
In 1953, Rubio-Alvarez et al. used an elbow catheter with a guide wire to perform pulmonary valvuloplasty on a 10-month-old infant with pulmonary valve stenosis. It is recognized as the earliest clinical report on interventional treatment of structural heart disease.
In 1966, Rashkind and Miller used a double-lumen balloon catheter to perform atrial septostomy on 3 infants with complete transposition of the great arteries. Almost at the same time, Portsmann used an embolus made of foam to perform catheter occlusion to treat patent ductus arteriosus.
Since 1974, King, Mills, Rashkind, etc. have designed congenital heart disease occluders, which have not been widely promoted because of poor effects and easy failures, but they have provided basic ideas for subsequent technical updates [4].
It wasn’t until 1997 that Amplatzer designed the occluder with a nickel-titanium alloy woven into a net and shaped into a double disc and one waist structure that is widely used in clinical practice, and the intervention of congenital heart disease has truly matured [4].
In 1982, Kan implemented PBPV for patients with pulmonary valve stenosis. In 1984, Lababidi successfully completed PBAV. In 1984, Japanese scholar Inoue developed a balloon to implement PBMV for patients with mitral stenosis.
In 2000, Bonhoeffer’s team reported that a 12-year-old patient with pulmonary valve stenosis and regurgitation after repairing tetralogy of Fallot successfully implemented PPVI [5], opening a new era of transcatheter valve replacement.
In 2002, Cribier completed the first human TAVR [6], setting off a new trend in interventional treatment of structural heart disease.
In 2003, the world’s first transcatheter mitral valve repair using the MitraClip system was successful [7], creating a precedent for transcatheter valve repair technology.
In 2012, the Affiliated Hospital of Rigshospitalet University in Copenhagen, Denmark completed the world’s first human TMVI, pushing transcatheter valve therapy technology to a new climax [8].
In 1995, Sigwart and others successfully implemented PTSMA on 3 patients with hypertrophic obstructive cardiomyopathy at the Royal Bruton Hospital in the United Kingdom [9]. In 2002, Horst Sievert used the PLAATO system to first report the transcatheter left atrial appendage occlusion, marking the birth of another important structural heart disease interventional therapy [10].
The new technology of structural heart disease opens and represents the fourth cardiac revolution in interventional cardiology.
Experts believe that the first revolution in interventional cardiology originated from the invasive cardiac catheterization techniques in 1929, such as cardiac catheterization, coronary angiography, and electrophysiological examinations [11].
The second revolution is based on the catheter treatment technology of simple balloon dilatation, such as coronary balloon dilation, pulmonary balloon dilatation and mitral valve balloon dilatation.
The third revolution is a technology characterized by simple implants (coronary stents, congenital occluders) or simple pacing and ablation techniques.
The fourth revolution is characterized by complex implants, delivery systems or precise interventions. It is the product of advanced catheter intervention technology and biomedical engineering technology. Representative technologies include TAVI, MitraClip, transcatheter ventricular assist devices, and capsules. Pacemaker, His bundle or left bundle branch pacing, pulsed electric field ablation, precision PCI, etc.
3. Current status of interventional therapy for structural heart disease
Since this century, the interventional treatment of structural heart disease has made great progress.
From 2007 to 2019, a total of 17 TAVR valves have obtained European CE certification. The new valve makes TAVR surgery more and more safe and effective. The current valve guideline management has listed patients with low-risk surgical procedures and elderly aortic stenosis as indications for TAVR [12-13].
In 2013, the number of TAVR operations in Germany exceeded that of surgical aortic valve operations.
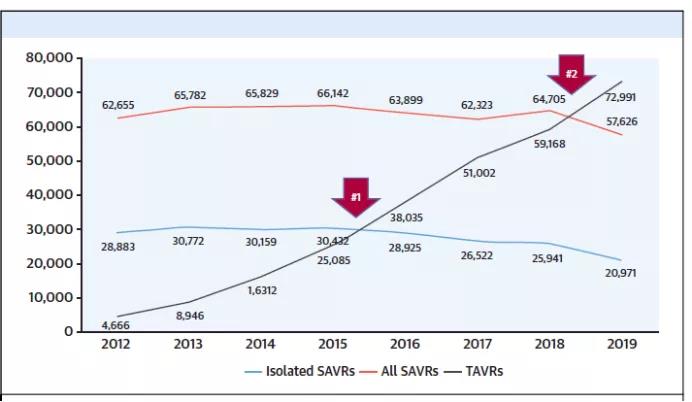
In 2019, the number of TAVR operations in the United States also surpassed surgical valve replacement operations (Figure 2) [14].
In 2020, the number of completed TAVR cases worldwide will be around 150,000.
During the 2016 TCT conference, Professor Martin Leon of the United States predicted that the global TAVR will reach 289,000 units per year in 2025, and its market sales will exceed the coronary stent market; at the same time, he also predicted that the structural heart disease market will surpass coronary intervention in 2020 The market reaches 20 billion US dollars.
MitraClip has completed more than 100,000 cases worldwide, and currently has about 20,000 cases completed each year. Currently, 200,000 cases of left atrial appendage occlusion have been completed globally, and approximately 50,000 cases have been completed each year.
At present, a variety of new devices and technologies for interventional treatment of structural heart disease are under development. Structural heart disease is showing a flourishing and vigorous development trend, including: mitral valve interventional therapy repair technology, TMVI, left ventricular volume reduction device (Parachute And Revivent), transcatheter tricuspid valve intervention device, atrial septal shunt, new congenital heart occluder, Liwen’s procedure, new left atrial appendage occluder, etc. The wave of interventional treatment of structural heart disease is sweeping the world.
4. Future prospects
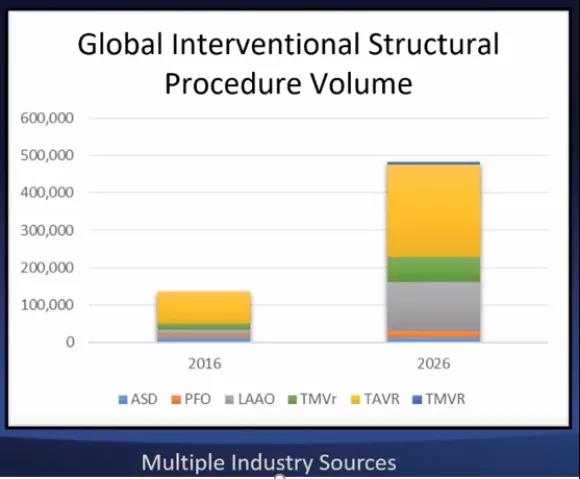
The author predicts that the development boom of interventional therapy for structural heart disease will continue for more than 10 years, and the number will increase rapidly (Figure 3). In the next 10-20 years, development and breakthroughs may be made in these areas:
(1) Progress has been made in valve durability, such as breakthroughs in dry valve, anti-calcification treatment technology, and multi-polymer technologies, allowing TAVR technology to be promoted to young patients;
(2) The number of TEER surgeries has increased dramatically, and breakthroughs have been made in new mitral valve repair technology, which promotes the clinical popularization of transcatheter mitral valve repair; breakthroughs have been made in transfemoral mitral valve replacement, which has become a mature treatment technology;
(3) The technology of transcatheter tricuspid valve interventional therapy is mature, and it has become a conventional treatment for tricuspid regurgitation;
(4) The development and application of new type of LAA occlusion device makes LAA occlusion safer, more effective and convenient. Minimal LAA occlusion surgery is generally carried out;
(5) Progress has been made in the treatment of hypertrophic cardiomyopathy, which can achieve safer, more convenient and effective ablation of hypertrophic cardiomyopathy;
(6) A breakthrough has been made in interventional therapy for heart failure, and it has launched an assault on the last fortress to overcome heart disease.
(source:internet, reference only)
Disclaimer of medicaltrend.org



