Nature: Cancer cells can “instigate” some immune cells to protect cancer cells
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Nature: Cancer cells can “instigate” some immune cells to protect cancer cells
Nature: Cancer cells can “instigate” some immune cells to protect cancer cells. Nature: Cancer cells can actually “instigate” some immune cells and produce lactic acid to feed them, which in turn can protect cancer cells.
Regarding the relationship between the immune system and cancer cells, we often think of cats and mice, but will all cats catch mice? Will there be some cats who like to make friends with mice and do not hesitate to become a “disgrace to the cat world”? The answer is yes, at least Tom is such a cat.
Then, in the immune system of the human body, is there such a type of immune cells that cannot withstand the sugar-coated shells from cancer cells, rebel into the enemy’s camp, and in turn do things for them?
On February 15, 2021, researchers from the Hillman Cancer Center and the University of Pittsburgh School of Medicine published a research paper titled Metabolic support of tumour-infiltrating regulatory T cells by lactic acid in the top international academic journal Nature.
This study shows that the tumor microenvironment will “instigate” a subgroup of immune T cells called regulatory T cells (Treg), reducing the sensitivity of cancer patients to immunotherapy.
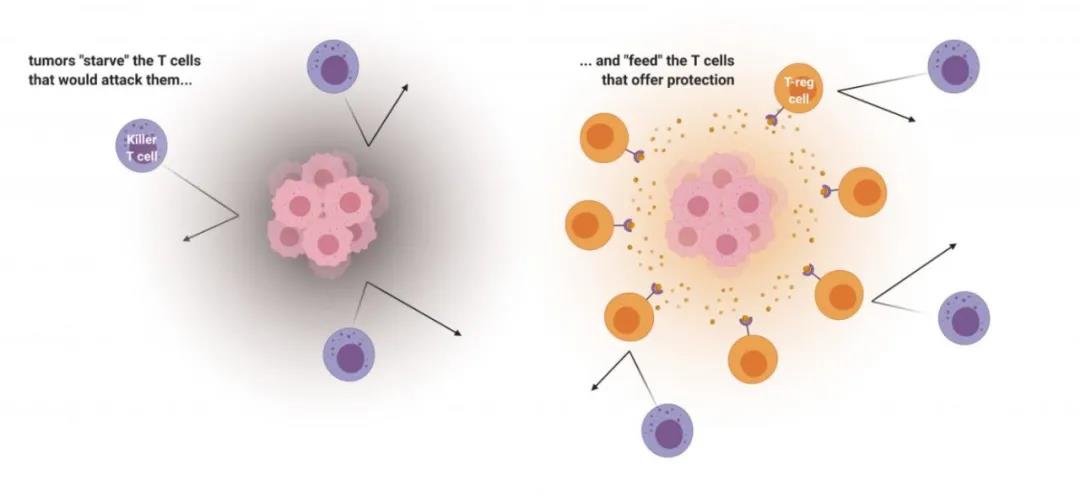
The tumor microenvironment produces lactic acid through metabolism and maintains a high lactic acid environment to inhibit T cells that attack cancer cells. At the same time, lactic acid “feeds” regulatory T cells (Treg) to protect themselves from being pursued by the immune system.
More importantly, the study also found and confirmed that inhibiting the MCT1 gene can prevent the uptake of lactic acid, thereby enhancing the efficacy of cancer immunotherapy.
In recent years, the rise of immunotherapy has opened up a new era of cancer treatment and has brought new hopes to cancer patients. However, it is regrettable that immunotherapy is not effective for everyone. For some cancer patients, especially young and female cancer patients, immunotherapy has little or no effect at all.
More importantly, although individual differences in immunotherapy have always existed, in fact there are many specific reasons for this phenomenon, and until now the scientific community has not been able to make a sufficient explanation.
In response, Dr. Greg Delgoffe, the corresponding author of this study and associate professor of the Department of Immunology at the University of Pittsburgh School of Medicine, said: “Most people do not respond to immunotherapy because we do not really understand the interaction between the immune system and the tumor microenvironment.”
In this study, the research team based on previous findings that Treg cells have different metabolic characteristics from effector T cells, and boldly hypothesized that the metabolic changes of the tumor microenvironment (TME) are related to the increase in the inhibitory activity of Treg cells in the tumor.
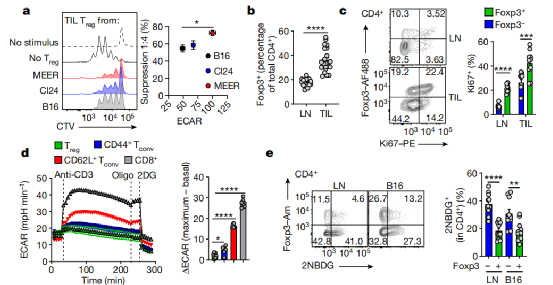
Treg cells have different metabolic characteristics from traditional T cells in normal and transplanted tumor tissues
Treg cells are an important immune T cell, which can inhibit the activation and division of effector T cells that kill cancer cells, maintain tolerance to autoantigens, and prevent autoimmune diseases, such as type I diabetes, Crowe Grace disease and multiple sclerosis.
It is worth noting that tumor cells produce a metabolically depleted, hypoxic and acidic tumor microenvironment, which can attract Treg cells and promote their functional specialization. Therefore, the effector T cells that enter the tumor tissue will face the situation of “being enemies”-not only to compete with tumor cells for metabolites, but also to be strongly inhibited by Treg cells in the tumor microenvironment.
In an in vitro cell culture experiment, the researchers found that when Treg cells use the glycolytic pathway (the glycolytic pathway does not require oxygen and produces a byproduct of lactic acid) to metabolize glucose in a high-glucose medium, the Treg cells become unstable. Moreover, the inhibitory ability of effector T cells is poor.
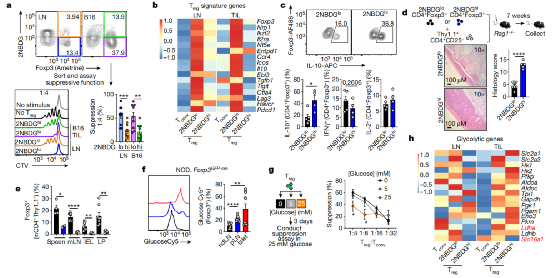
Saccharophilicity is associated with decreased Treg cell function
However, unlike most other cells, Treg cells can tolerate high levels of lactic acid. The research team found that when treated with lactic acid, the state of Treg cells in the high-sugar medium steadily improved and resumed growth and division. Coincidentally, tumor cells usually use glycolysis to produce energy and produce large amounts of lactic acid.
From this point of view, tumor cells and Treg cells are a natural match. The tumor cells produce lactic acid to feed the Treg cells, and the Treg cells inhibit the effector T cells to ensure the survival of the tumor cells.
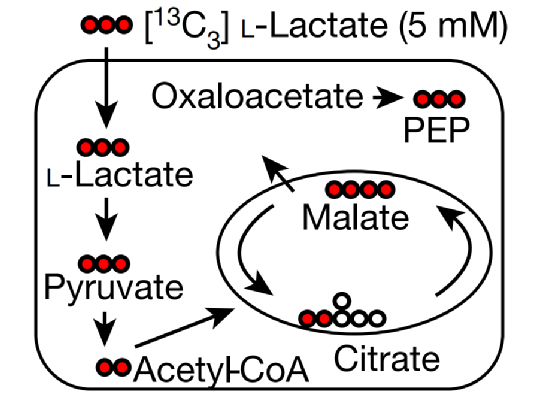
Treg cells metabolize lactic acid to support their proliferation and inhibitory functions
To further verify the relationship between the two, the researchers targeted a gene called MCT1, which encodes the lactate transporter in Treg cells, and then combined MCT1 knockout or drug suppression with immunotherapy. Research results indicate that preventing the uptake of lactic acid by Treg cells in the tumor microenvironment slows tumor growth and increases the response to immunotherapy.
Greg Delgoffe said: “Cancer cells are very smart. The tumor microenvironment will not only starve to death the effector T cells that harm them, but also feed the Treg cells that protect them. This study shows that inhibiting the uptake of lactic acid allows Treg cells starve. When Treg cells cannot be maintained by tumors, effector T cells will come in and kill cancer cells.”
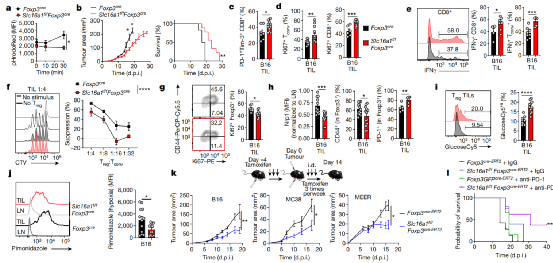
Preventing the uptake of lactic acid by Treg cells in the tumor microenvironment slows tumor growth and increases the response to immunotherapy
All in all, this study has shown us the “sly and cunning” of cancer cells: the tumor microenvironment will not only hinder the killing function of effector T cells, but also “trick” Treg cells to further inhibit effector T cells, thereby promoting the survival of cancer cells. .
Not only that, this study also explains to some extent the phenomenon that some cancer patients are not sensitive to immunotherapy. In the future, we may be able to inhibit lactic acid metabolism-related genes, such as MCT1, to enhance the effectiveness of immunotherapy and make immunotherapy truly Benefit the majority of cancer patients!
(source:internet, reference only)
Disclaimer of medicaltrend.org



