MIT: Boosts T-cell cancer therapy by vaccine
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
MIT: Boosts T-cell cancer therapy by vaccine
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
MIT: Boosts T-cell cancer therapy by vaccine.
MIT researchers have developed a strategy to increase the effectiveness of CAR-T cell therapy in eradicating solid tumors.
By using a vaccine to boost the response of these engineered T cells and stimulate the immune system to target various tumor antigens, they succeeded in addressing the problem of antigenic variation — a major hurdle in treating solid tumors.
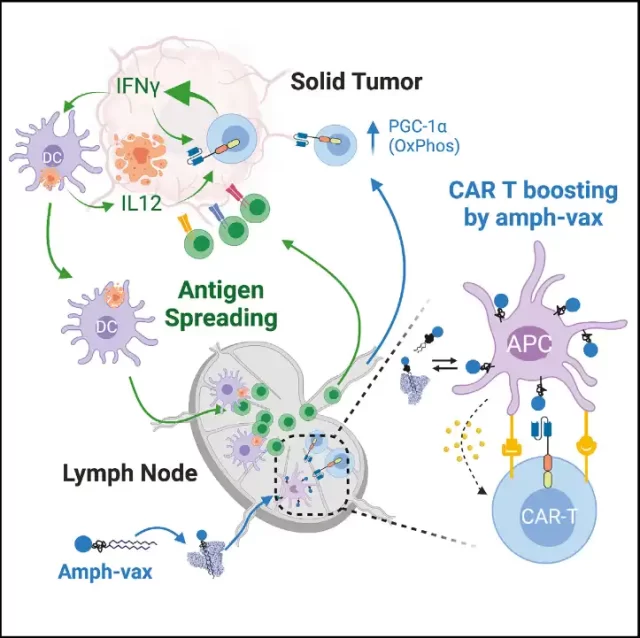
Engineering T cells to destroy cancer cells has been successful in treating certain types of cancer, such as leukemia and lymphoma. However, its therapeutic effect on solid tumors is not ideal.
One of the reasons for the lack of success is that the T cells target only one antigen (a target protein found on the tumor); if some tumor cells do not express this antigen, they can escape the T cell attack.
Researchers at MIT have now found a way to overcome this hurdle by using a vaccine that boosts the response of engineered T cells, known as chimeric antigen receptor (CAR) T cells, while also helping the immune system generate New T cells targeting other tumor antigens. In a study of mice, the researchers found that this approach was more likely to eradicate tumors.
Professor Underwood-Prescott is a professor in the MIT Department of Bioengineering and the Department of Materials Science and Engineering, and a member of the MIT Koch Institute for Integrative Cancer Research and the Ragon Institutes at MGH, MIT, and Harvard.
Irvine is the senior author of the study, which was published July 5 in the journal Cell. The first author of the paper is Leyuan Ma, a former Koch Institute postdoctoral fellow who is now an assistant professor of pathology and experimental medicine at the Penn School of Medicine.
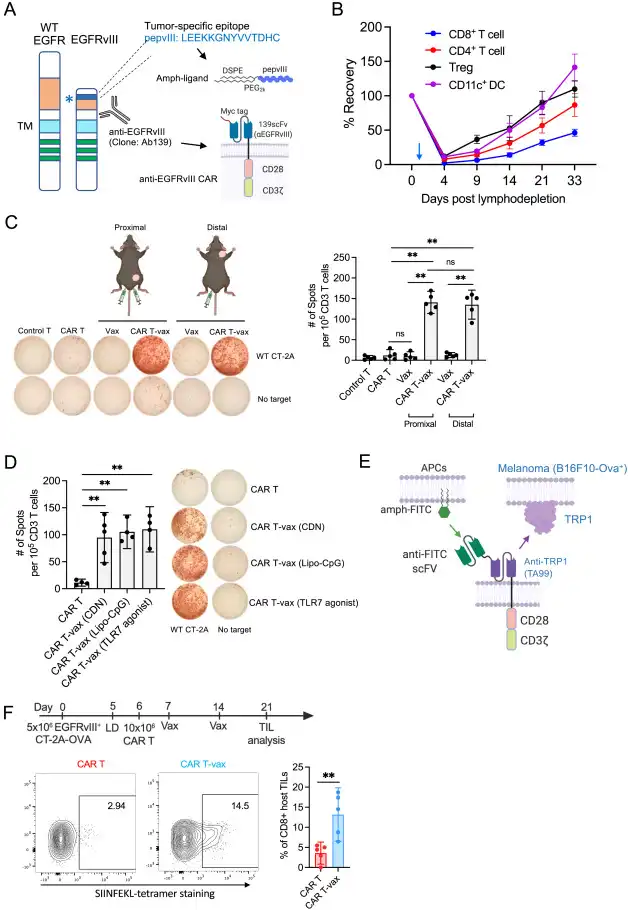
Engineered T cells
The U.S. Food and Drug Administration has approved several T-cell therapies for blood cancers. These therapies are based on CAR-T cells, which are engineered to display receptors that recognize specific antigens on cancer cells.
To try this treatment for glioblastoma, a type of brain cancer, the researchers engineered CAR-T cells that target a mutant version of the epidermal growth factor receptor.
However, not all glioblastoma cells express this antigen, and when attacked by CAR-T cells, some glioblastoma cells respond by stopping production of the target antigen.
In a 2019 study, Irvine and his colleagues boosted the effectiveness of CAR-T cells against glioblastoma by injecting mice with a vaccine shortly after injecting the engineered T cells.
The vaccine, which carries the same antigens that the CAR-T cells target, is taken up by immune cells in the lymph nodes, where the CAR-T cells are exposed to the vaccine.
In this study, the researchers found that the vaccine boost not only helped engineer CAR-T cells to attack tumors, but also had another unexpected effect: It helped generate host T cells that target other tumor antigens .
This phenomenon, known as “antigen spreading,” is desirable because it generates populations of T cells that work in concert to completely destroy tumors and prevent them from regrowth.
“This could precisely help with the antigenic heterogeneity of solid tumors, because if host T cells are directed to attack other antigens, they might be able to come in and kill tumor cells that CAR-T cells can’t kill,” Irvine said.
Immune enhancement
In their new study, the researchers wanted to explore how the additional T cell response is activated. They used the same type of CAR-T cells designed to target the mutated epidermal growth factor receptor and the same vaccine as in the 2019 study. Mice in the study received two doses of the vaccine, one week apart.
The researchers found that in these boosted mice, the CAR-T cells underwent metabolic changes that increased production of interferon gamma, a cytokine that helps stimulate a strong immune response. This helps T cells overcome the tumor’s immunosuppressive environment, which normally shuts down nearby T cells.
When CAR-T cells kill tumor cells expressing target antigens, host T cells (but not engineered CAR-T cells) encounter other antigens of these tumor cells, stimulating host T cells to target these antigens and help eliminate tumor cells.
The researchers found that without a response from the host T cells, the tumors would grow back even though the CAR-T cells had wiped out most of the original tumor cells. The reason for this is that tumor cells treated with CAR-T cells usually stop producing the antigens that the engineered cells target, thereby evading the cells’ attack.
Eradicate tumor
The researchers then tested their approach in mice with tumors that had varying levels of the target antigen.
They found that even in tumors where only 50% of the tumor cells expressed the target antigen, about 25% of the tumors could still be eliminated through the combined action of CAR-T cells and host T cells.
Tumors with higher levels of the target antigen had a higher rate of success. When 80 percent of the tumor cells expressed the antigen targeted by the CAR-T cells, tumors were eliminated in about 80 percent of the mice.
The technology used in the study has been licensed to a company called Elicio Therapeutics, which is working to develop the technology for potential testing in patients. In this study, the researchers focused on glioblastoma and melanoma, but they believe the technique could potentially be used to treat other types of cancer as well.
“In principle, this should apply to any solid tumor where you’ve generated CAR T cells that target them,” Irvine said.
Researchers are also studying how to adapt CAR-T cell therapy so that it can be used to attack tumors for which no target antigen has been identified.
MIT: Boosts T-cell cancer therapy by vaccine
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



