After-effects remain worrisome two years after contracting COVID-19
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
After-effects remain worrisome two years after contracting COVID-19
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
After-effects remain worrisome two years after contracting COVID-19.
Earlier this spring, the World Health Organization (WHO) declared an end to the global health emergency of COVID-19. However, the impacts of the virus are far from over.
A portion of individuals who have previously recovered from a COVID-19 infection continue to experience physiological, psychological, or cognitive symptoms, a condition known as “Long Covid.”
As per WHO’s definition, “Long Covid” is a condition that COVID-19 survivors may face, characterized by symptoms such as fatigue, shortness of breath, dizziness, brain fog, loss of smell or taste, among others. “Long Covid” can persist for 3 months, 6 months, 9 months, or even longer, and it has been described as an emerging public health crisis.
On August 21, 2023, the Nature Medicine published a study titled “Postacute sequelae of COVID-19 at 2 years.” This research indicates that even two years after infection with the novel coronavirus, the impact of COVID-19 may still persist.
The research team found that individuals previously infected with the coronavirus, including those who were hospitalized within 30 days of infection and those who were not hospitalized, still had a significantly elevated risk of developing many COVID-19-related chronic conditions over the course of two years. These conditions include diabetes, pulmonary issues, fatigue, blood clots, and diseases affecting the gastrointestinal and musculoskeletal systems.
Dr. Ziyad Al-Aly, the lead author of the paper and a clinical epidemiologist at Washington University in St. Louis, emphasized that the enduring and persistent risks associated with Long Covid for many individuals serve as a stark reminder that the COVID-19 pandemic is not truly behind us. The presence of Long Covid patients vividly underscores the harmful and long-lasting effects of COVID-19.

However, there is some encouraging news from this study. It notes that over the course of the two-year study, some health risks related to COVID-19 decreased to become inconsequential for non-hospitalized patients (the majority of COVID-19 cases are mild and do not require hospitalization).
These health risks included death, hospitalization, and diseases associated with the brain, heart, kidneys, and mental health. For instance, at 6 months and 19 months, the risks of death and hospitalization became statistically insignificant.
On the other hand, the situation remained dire for those who were hospitalized within 30 days of contracting the virus; two years post-infection, their risks of death and hospitalization remained elevated, as did the risks of adverse health conditions across all organ systems.
Dr. Ziyad Al-Aly stressed that the results of this study highlight the substantial cumulative burden of health loss caused by Long Covid. It underscores the ongoing healthcare needs of Long Covid patients, as the impact of Long Covid appears not only to affect their quality of life but could also lead to reduced life expectancy and potentially impact labor force participation, economic productivity, and societal well-being.
In the past, scientists around the world have extensively documented how the novel coronavirus attacks nearly every organ system in the human body, leading to a spectrum of diseases and symptoms affecting the lungs, heart, brain, blood, musculoskeletal system, and gastrointestinal tract. This latest research focuses on the risks of death, hospitalization, and 80 different adverse health conditions that COVID-19 patients might face within two years of infection.
Previous understanding of Long Covid was mostly limited to the analysis of patient data up to one year post-initial infection. Investigating the long-term health trajectories of COVID-19 patients beyond the first year is crucial and may inform care strategies for this population.
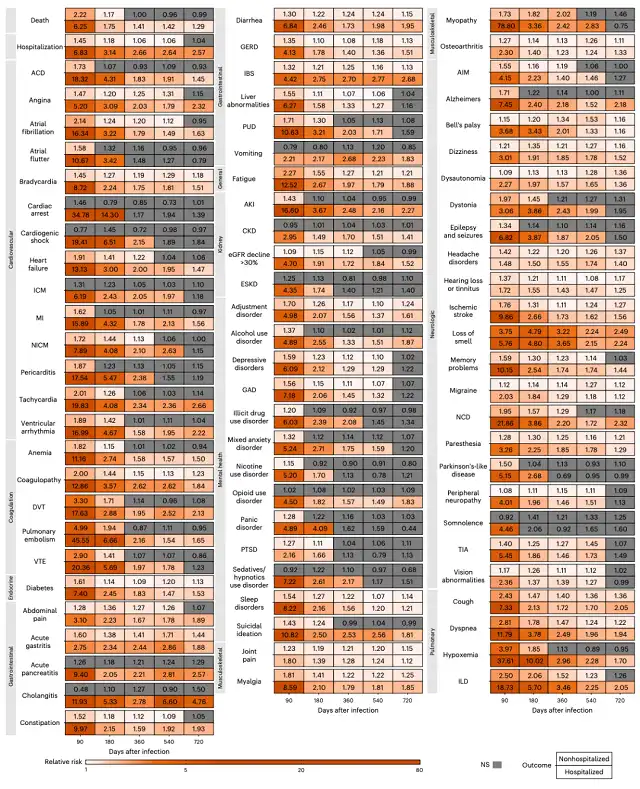
The research team analyzed de-identified medical records from the U.S. Department of Veterans Affairs, the largest integrated healthcare system in the United States, covering patients of various ages, ethnicities, and genders.
They created a control dataset consisting of over 5.9 million individuals who were not diagnosed with COVID-19 between March 1, 2020, and December 31, 2020. During the same period, they compiled a group of 138,818 individuals who tested positive for COVID-19, with 118,238 being non-hospitalized patients and 20,580 being hospitalized patients.
Using statistical models, the research team examined the health risks related to COVID-19 two years post-infection. Over this period, data were collected at five different time points to determine when and if the risks of 80 Long Covid-related conditions diminished compared to the non-infected control group.
For non-hospitalized individuals who contracted the virus, the risks of death and hospitalization decreased over time, becoming statistically similar to the non-infected control group at 6 months and 19 months. Within two years, 55 of the 80 Long Covid-related conditions analyzed (69%) exhibited decreased or statistically insignificant risk.
For individuals hospitalized due to COVID-19, the risks of death and hospitalization remained high two years post-infection, with 52 of the 80 Long Covid-related conditions (65%) showing elevated risk. This suggests that the road to recovery for those severely affected by COVID-19 and requiring hospitalization is arduous and prolonged.
Additionally, the research team measured and compared the health-adjusted life years lost due to COVID-19. The results indicated that, for non-hospitalized COVID-19 patients, COVID-19 led to a loss of 80 healthy life years per 1000 people over two years, with approximately 25% of the loss occurring in the second year.
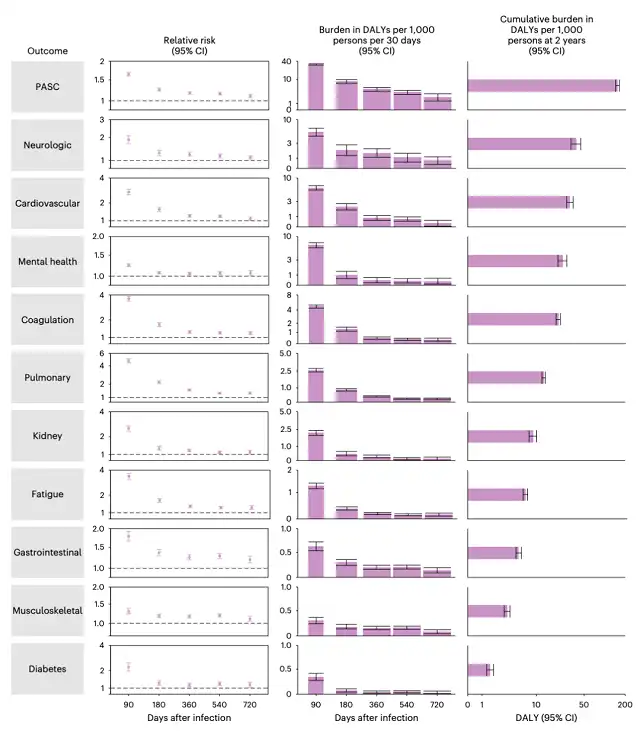
Dr. Ziyad Al-Aly emphasized that this 25% represents a significant portion of the burden of disability and disease.
It underscores that addressing the long-term effects of COVID-19 on health is a lengthy and formidable journey. Even in the second year post-infection, COVID-19 continues to pose a substantial risk of additional health losses.
The research team found that in the United States, the health-adjusted life years lost due to COVID-19 were significantly higher than other major diseases, surpassing even cancer and heart disease.
For instance, over a lifetime, cancer and heart disease led to the loss of 50 and 52 healthy life years per 1000 people, respectively, while in the first two years post-infection, COVID-19 resulted in the loss of 80 healthy life years per 1000 people.
Dr. Ziyad Al-Aly concluded that as we continue to study the long-term impacts of the novel coronavirus on health, the burden of disability and disease caused by Long Covid may increase. These two years of data have already revealed a staggering burden. Importantly, unlike cancer and heart disease, there is currently no effective treatment for Long Covid.
He further emphasized that measures to reduce the risk of Long Covid should be a focus of public health policies. Using updated vaccines, including those that prevent the spread of the virus, may be a key strategy in reducing the risk of long-term health problems. Additionally, finding treatments for Long Covid should be a top priority.
After-effects remain worrisome two years after contracting COVID-19
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



