The Immune Escape Mechanisms and Treatment Approaches in Tumor Immune Cycle
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
The Immune Escape Mechanisms and Treatment Approaches in Tumor Immune Cycle
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
The Immune Escape Mechanisms and Treatment Approaches in Tumor Immune Cycle
The application of immune checkpoint inhibitors (ICIs) has revolutionized the treatment paradigm for various cancers.
However, despite success in some cancer patients, a considerable portion shows no response to immune checkpoint inhibitors.
A functional cancer immune cycle is a prerequisite for a clinical response to immune checkpoint inhibitors, requiring activation and proper functioning at each step for meaningful immune responses.
Yet, the activation of the cancer immune cycle may not be equally present in every patient and cancer type.
Ideally, treatments should consider each step of the cancer immune cycle, providing personalized approaches to address functional impairments in the specific cancer immune cycle of individual patients.
Cancer Immune Cycle:
The cancer immune cycle involves several steps critical for initiating a clinically effective T-cell-mediated immune response:
- Release of tumor cell antigens.
- Antigen uptake by antigen-presenting cells (APCs).
- Transport of APCs to local lymph nodes through the lymphatic system.
- Presentation of antigens to naïve T cells in local lymph nodes.
- Activation of T cells in local lymph nodes.
- Migration of T cells to the local tumor site through the bloodstream.
- T-cell-mediated immune response in the tumor microenvironment.
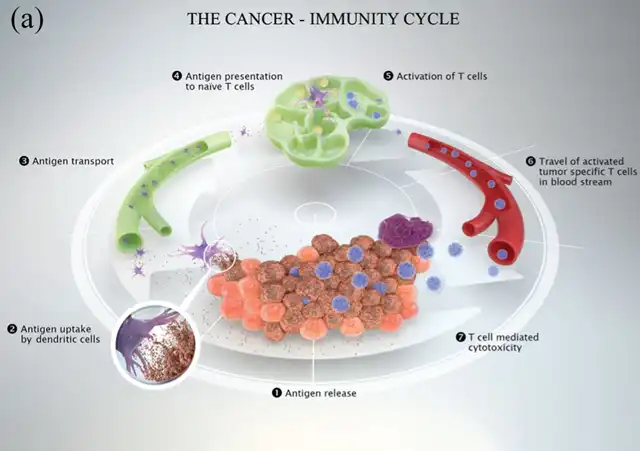
Challenges and Strategies:
Deficient Tumor Antigen Release: The first step in the cancer immune cycle requires the release of tumor-specific antigens from dying tumor cells. Insufficient antigen release may hinder effective antigen presentation and further progression of the cancer immune cycle, resulting in ineffective recognition of tumor cells by T cells. Cancer vaccines are being studied as a potential strategy to overcome antigen release and presentation deficiencies, showing some clinical benefits in situ or minimal residual disease.
Impaired Activation of T Cells in Local Lymph Nodes: Delivering tumor-specific antigens to naïve T cells triggers the activation and proliferation of effector T cells. However, the distribution of effector and regulatory T cells plays a crucial role in the effectiveness of the immune response. Immune checkpoint blockade has been shown to impact the diversity of the T-cell receptor (TCR) gene library, enhancing anti-tumor immunity at this specific stage of the cancer immune cycle.
Systemic Factors Inhibiting Tumor-Specific T Cells in Circulation: Activated effector T cells must circulate through the bloodstream to reach the local tumor site. Factors in the blood, such as increased neutrophils, can suppress T-cell-mediated anti-tumor responses, affecting overall treatment response and survival rates. Inhibiting pro-inflammatory cytokines may be a potential avenue to enhance anti-tumor immune responses.
Local Tumor Microenvironment Immune Suppression: The composition of blood vessel structures and cytokine gradients in the local tumor microenvironment affects T-cell homing and, consequently, the anti-tumor immune response. Combining therapies, such as chemotherapy or anti-angiogenic agents, with immune checkpoint inhibitors may enhance the immune response in the tumor microenvironment.
Conclusion:
Understanding the unique interactions between a patient’s immune system and cancer cells, as well as identifying specific immune escape mechanisms, is crucial for guiding personalized immunotherapy choices in cancer patients.
Current research is exploring promising novel immunomodulatory therapies and their combinations to achieve meaningful immune responses in cancer patients.
The Immune Escape Mechanisms and Treatment Approaches in Tumor Immune Cycle
Reference:
“Immune escape mechanisms and therapeutic approaches in cancer: the cancer-immunity cycle.” Ther Adv Med Oncol. 2022;14: 17588359221096219.
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



