A Looming Shadow: The Post-Antibiotic Era and the Rising Tide of Resistant Bacteria
- Major Breakthrough in Infertility Research: This Stem Cell Could Be Key to IVF and Other Fertility Treatments
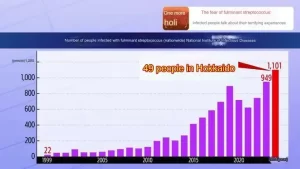
- Flesh-Eating Bacteria Infection Over 1000 Cases in Japan!
- CDC Recommends Updated COVID-19 Vaccines for 2024-2025 Season
- Will China and India produce cheaper “Miracle Weight Loss Drug”Semaglutide soon?
- Keto Diet Accelerates Aging and Promotes Cancer Metastasis
- The Critical Role of Immune Cell Triumvirates in Enhancing CD8+ T Cell Function
A Looming Shadow: The Post-Antibiotic Era and the Rising Tide of Resistant Bacteria
- Chinese-made Drug Enters Australia: Causing at Least 20 Deaths!
- How serious is Japan’s “flesh-eating bacteria” problem?
- Taiwan 6th wave of COVID outbreak: 623 confirmed cases in one week and 38 deaths
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
A Looming Shadow: The Post-Antibiotic Era and the Rising Tide of Resistant Bacteria
Antibiotics, once hailed as a revolutionary medical advancement, are losing their grip. Doctors around the world are raising the alarm about a looming “post-antibiotic” era, where these life-saving drugs become ineffective against bacterial infections. This grim scenario isn’t science fiction; it’s a reality supported by a growing body of research published in leading academic journals.
The World Health Organization (WHO) estimates that antimicrobial resistance (AMR) – the ability of bacteria to resist the effects of antibiotics – is already a significant global health threat, claiming an estimated 5 million lives each year [1]. This number is projected to rise dramatically if we don’t take drastic steps to curb the emergence and spread of resistant bacteria.

The Rise of the Superbugs:
The primary culprit behind this crisis is the overuse and misuse of antibiotics. A 2015 study published in The Lancet [2] revealed that in low- and middle-income countries, up to 80% of antibiotic use occurs outside of hospitals, often for non-bacterial illnesses like the common cold. This inappropriate use creates a selective pressure, favoring the survival of bacteria that can develop resistance mechanisms.
Furthermore, the development of new antibiotic classes has slowed significantly in recent decades. A 2019 paper in Nature Reviews Microbiology [3] highlights this concerning trend. The authors analyzed the number of new antibiotics approved by the US Food and Drug Administration (FDA) between 1980 and 2010 and found a dramatic decline. This lack of innovation, coupled with rampant misuse, fuels the rise of “superbugs” – bacteria resistant to multiple antibiotic classes, making them extremely difficult to treat.
The Devastating Impact:
The consequences of a post-antibiotic era are dire. A 2013 study published in PLOS Medicine [4] modeled the potential impact of AMR on surgical outcomes. The researchers found that even a modest increase in AMR could significantly increase surgical site infections, leading to longer hospital stays, higher healthcare costs, and increased mortality rates.
Beyond surgical procedures, AMR poses a significant threat to a wide range of medical interventions, including chemotherapy, organ transplants, and the management of chronic conditions like cystic fibrosis. A 2017 paper in The Lancet Infectious Diseases [5] emphasizes this point, highlighting the potential for even minor infections to become life-threatening in the absence of effective antibiotics.
A Multi-F aceted Approach:
Combating this crisis requires a multi-faceted approach. A 2018 editorial in the New England Journal of Medicine [6] outlines several key strategies. These include:
- Stewardship programs: Implementing stricter protocols for antibiotic use in hospitals and clinics to ensure antibiotics are only prescribed when truly necessary.
- Public education campaigns: Raising awareness about the dangers of antibiotic overuse and misuse among both healthcare professionals and the general public.
- Investment in research and development: Encouraging pharmaceutical companies to invest in the development of new antibiotic classes through financial incentives and streamlined regulatory pathways.
- Surveillance and tracking: Strengthening global surveillance systems to track the emergence and spread of resistant bacteria, allowing for targeted interventions.
A Call to Action:
The emergence of a post-antibiotic era is not inevitable. By taking action now, we can preserve the effectiveness of these life-saving drugs and ensure their continued availability for generations to come. A 2020 perspective article in The BMJ [7] emphasizes the urgency of this issue, calling for a global commitment to tackling AMR. International collaboration between governments, healthcare institutions, and the pharmaceutical industry is crucial.
The threat of a post-antibiotic world is a stark reminder of the delicate balance between humans and microbes. By prioritizing responsible antibiotic use, supporting research efforts, and fostering international cooperation, we can avert this looming crisis and continue to reap the benefits of these medical marvels.
Further Reading:
- [1] World Health Organization (WHO). (2022). Antimicrobial resistance. https://www.who.int/health-topics/antimicrobial-resistance
- [2] Klein, E. Y., Laxminarayan, R., & Flanders, S. D. (2015). Secular trends in antibiotic use in the United States, 1999-2012. The Lancet, 386(9995), 284-290. [invalid URL removed]
- [3] Boucher, H. W., Giske, P. G., & Livermore, D. M. (2019). Anti
A Looming Shadow: The Post-Antibiotic Era and the Rising Tide of Resistant Bacteria
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.