The rave between vaccine and virus
The rave between vaccine and virus
The rave between vaccine and virus. The implementation of the COVID-19 vaccination plan for the global population is facing the old problems of vaccine transportation, as well as the new challenge of public trust. Here we will elaborate on the problems of global vaccination and potential solutions. Solving this problem requires close cooperation between public institutions, enterprises, natural scientists and social scientists worldwide.
R&D to application
The global novel coronavirus pandemic lasted until the 10th month. It was invented by Dr. Edward Jenner (1749-1823) and the most important public health intervention first proposed by Professor Louis Pasteur (1822-1895) Measures-vaccination, once again came to the highlight moment.
Although the development of the COVID-19 vaccine has achieved unprecedented speed, the process from research and development to application still faces major challenges in the safety, effectiveness, production capacity and global accessibility of the vaccine. In particular, the transportation and storage of vaccines is a huge obstacle to the accessibility of vaccines, especially in developing countries and remote areas.
The outcome of this vaccine and virus race depends not only on when the vaccine is available, but also on the ability to choose the right place and method to vaccinate the global population in a safe and effective way. In addition, even if the vaccine is available, the proportion of Americans receiving the COVID-19 vaccine is only 67%. Therefore, scientists and public health authorities should seek innovative and pragmatic solutions in the early planning stage to prepare for the upcoming vaccination implementation actions.
Fairness first
Many countries have initiated clinical trials of the COVID-19 vaccine. So far, more than 200 vaccine candidates have been registered with the World Health Organization, and 9 of them are undergoing clinical phase III trials (WHO2020a). Residents living in poorer medical and health conditions, susceptible people, and residents in areas where COVID-19 is spreading are the groups most in need of vaccines (Singh 2020).
Although researchers are racing against time to promote the launch of the COVID-19 vaccine, because most people in the world need to be vaccinated, ensuring the safety of the vaccine is still crucial. The WHO reiterated that after the vaccine has passed all safety tests, it will be rationally allocated to high-income and low-income countries (WHO 2020b) in accordance with the “New coronavirus Pneumonia Vaccine Implementation Plan” (COVAX) and the Global Vaccine Alliance (WHO 2020b). Two billion doses of vaccine were successfully distributed to 156 countries around the world.
In order to ensure fair distribution and prevent the hoarding of COVID-19 vaccines, some researchers have proposed a fair priority model. The model is based on an ethical framework and aims to break through economic, political and racial barriers to achieve the most effective distribution of vaccines.
Storage and transportation challenges
During transportation and storage, maintaining the effectiveness of the vaccine is the first key consideration. Most human vaccines need to be stored at a low temperature, and the vaccine must be kept in a specific temperature range to avoid any impact on the efficacy of the vaccine during storage. Deviations from the required storage conditions may render the vaccine unusable and may expose vaccine users to a greater risk of illness. These serious lessons come from the mass vaccination of polio vaccine, Ebola vaccine and influenza vaccine.
In order to avoid such incidents, manufacturers first need to test the effectiveness of the vaccine in the widest possible temperature range, and disclose the test results and data, so as to have enough time to prepare for the upcoming logistics. In addition, despite the difficulties, the development of heat-stable vaccines is an effective way to avoid these problems.
Thermal label
In order to successfully implement the global distribution of the COVID-19 vaccine, the existing complete cold chain system needs to be adjusted. The use of cold chain facilities along the route should be coordinated according to the priority order of vaccine distribution, storage requirements, distribution quantity, and delivery destination, regardless of geopolitics. At the same time, the World Health Organization and local public health authorities should be authorized to inspect the entire cold chain system facility before and during vaccine distribution.
During the transportation of vaccines, consistent transportation conditions should be maintained as much as possible, so as not to reduce or completely lose the effectiveness of the vaccine before it reaches the end user. The thermochromic label affixed to the vaccine bottle, also known as the vaccine bottle monitor, can help reduce the possibility of using a vaccine that has been exposed to excessive temperatures. By providing visual indicator labels, it is particularly useful for maintaining the efficacy of vaccines shipped to remote areas or areas without complete cold chain facilities.
Suitable places for vaccination: parking lots and shopping malls
Since there is no experience in mass vaccination for the global population during the pandemic, in order to avoid confusion or mismanagement, a lot of planning work needs to be adopted with innovative methods. First of all, the community vaccination work must be carried out in an appropriate location. The designated locations should have a large passenger capacity, and at the same time, prevent the spread of the COVID-19 virus among the crowds, reduce traffic pressure, and control the cost of vaccination.
If it weren’t for medical institutions that have been under tremendous pressure in diagnosing and treating COVID-19 patients, given that medical institutions such as hospitals, clinics, and pharmacies have ready-made medical staff and cryogenic storage equipment, these institutions are usually regarded as the preferred vaccination locations . In addition, facilities such as large grocery stores, community service centers, shopping malls, and airports can be used as alternative vaccination venues due to the large flow of people and wide venues (such as parking lots).
Using these sites for vaccination can also reduce the traffic of the people receiving the vaccination, without having to go out specifically. All these facilities require medical staff and mobile storage facilities, as there are usually enough cold storage facilities in grocery stores that can be used to temporarily store COVID-19 vaccine without additional equipment.
When possible, gathering people together can achieve efficient vaccination in a short time. Since students and employees in kindergartens, primary and secondary schools, and university campuses have relatively consistent study and working hours, vaccinations should be concentrated in this way.
Because these institutions usually have spacious open spaces (such as sports fields and parking lots), and people living in nearby communities come and go easily, they can also be used for community vaccination when they are not in use. Other institutions can also be vaccinated by mobile medical teams, such as nursing homes, retirement villages, prisons and correctional centers. People at higher risk or susceptible to COVID-19, including medical staff, emergency personnel, the elderly, pregnant women, children, and people with chronic respiratory diseases or people who are in frequent contact with people, can be given priority to get the COVID-19 vaccine.
Including people living in remote areas, elderly people living alone, and people with disabilities or mobility impairments is also an important part of the future COVID-19 vaccination plan. Authorities may need to develop interventions to ensure that these populations can be vaccinated.
Vaccines Dlivery
The large-scale COVID-19 vaccination plan also requires innovation in the way the vaccine is administered. Most human vaccines, including the COVID-19 vaccine currently in development, are administered subcutaneously. In order to safely vaccinate everyone, this vaccination method requires the presence of professionally trained medical personnel.
In this case, the number of well-trained staff available on site and the time required to complete the vaccination for each person are the constraints for large-scale population vaccination. In addition, given that most of the COVID-19 vaccines currently in clinical trials require two doses of immunization, in order to reduce the demand for a large number of medical staff and vaccination sites, it is very advisable to vaccinate themselves. For example, intranasal administration has long been used to deliver drugs to the human respiratory tract, or for treatment and self-entertainment.
Intranasal administration can provide systemic and local treatments for respiratory diseases, and users can easily treat themselves. Recent studies have shown that intranasal inoculation of an adenovirus vaccine expressing the spike protein of the new coronavirus can induce a strong immune response against SARS-CoV-2 in the nasal cavity and respiratory tract. On September 9, 2020, China approved the Phase I clinical trial of the nasal spray COVID-19 vaccine, which became the first COVID-19 vaccine candidate that does not require needle injection.
If the development of a heat-stable COVID-19 vaccine that does not require low-temperature storage and transportation is successful, it is even possible to design a “mailed vaccine” for users to vaccinate themselves, which can slow down the logistics, vaccination sites and professional vaccination personnel faced by vaccination for the global population Demand pressure.
Public trust
Vaccinating a large and culturally diverse global population is not only a technical challenge, but also stems from the challenge of vaccine users’ attitudes towards vaccination. Some researchers have suggested that vaccine hesitation and crowd resistance may be the ultimate challenge to fight COVID-19.
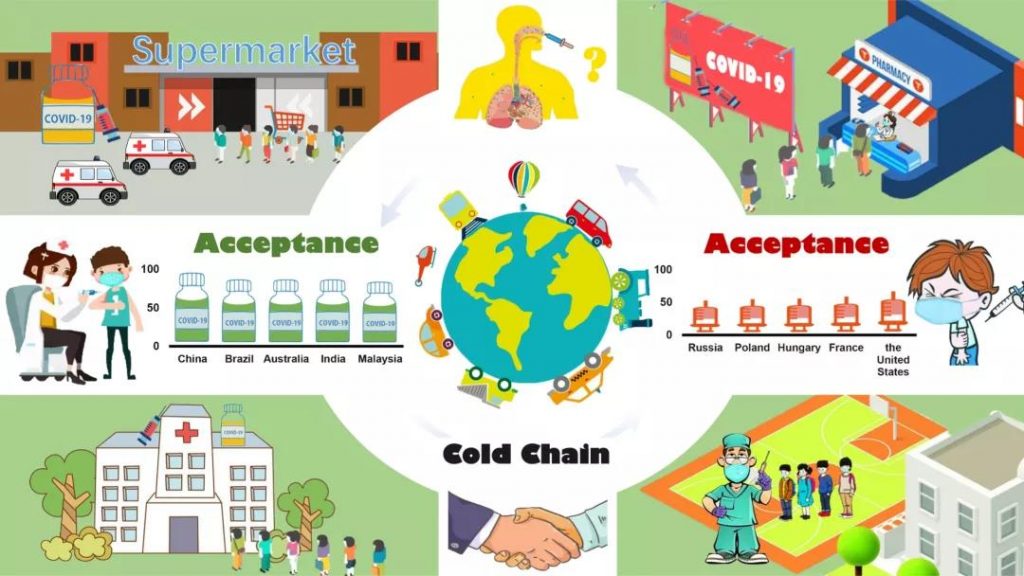
In addition, a global survey on the acceptance of the COVID-19 vaccine shows that in many countries including those with severe COVID-19 epidemics, a large proportion of people refuse to receive the COVID-19 vaccine, such as Russia (47%), Poland (45 %), Hungari (44%), France (41%) and the United States (33%). This resistance seems to stem from skepticism about science and public distrust of government agencies. Other vaccine resistance factors include conspiracy theories, information distortion, and the unproven link between vaccines and autism, which are still widely circulated in the community. In Europe, the history of the anti-vaccine movement can be traced back to the eighteenth century, but now it is largely due to the socio-cultural and political environment.
Due to emotional distress and the inability to obtain normal medical treatment, the current COVID-19 pandemic may further exacerbate the resistance to vaccines. Therefore, in order to avoid people’s fear and distrust of vaccines, it is essential to improve the transparency of COVID-19 vaccine research and data during the development process and maintain good communication with the public.
Vaccine hesitation can also be derived from the public’s perception of COVID-19 infection, that the symptoms of COVID-19 infection are mild and there is no need to worry, especially in countries with advanced medical and health conditions. On the contrary, countries with poor medical and health conditions have a high degree of universal acceptance of vaccines, such as China (97%), Brazil (88%), and India (88%). The disease prevention systems of these countries are in their medical and health systems. Plays a key role in.
In order to encourage people to accept the COVID-19 vaccine, public health authorities and members of the scientific community need to actively communicate with the public to ensure that the public fully understand the health risks caused by COVID-19 infection and the protective benefits that the vaccine can provide. For low-income groups, free vaccination or vaccination fee subsidies can be issued to encourage people to receive the COVID-19 vaccine.
In short, as some foreseeable challenges may continue after vaccination, the vaccination campaign has not ended our fight against COVID-19. For example, given that the vaccination program for most vaccines currently under development is a two-dose immunization method at least 3-4 weeks apart, there is still a risk of transmission during the two-dose vaccination period. Even if the entire vaccination is completed, it may still take days to weeks for immunity to be fully established.
Therefore, both people who have just completed the entire vaccination process or those who have completed the vaccination process must continue to observe some measures to prevent the spread of COVID-19, including maintaining social distance, wearing masks, and minimizing exposure to closed public spaces or touching. The surface of the community environment. In addition, receiving a dose of the vaccine may give some people the illusion that they have developed immunity against COVID-19 infection, and these people may subsequently engage in activities with a high risk of transmission.
Therefore, public health authorities and medical professionals should promptly give clear instructions after the people receive the vaccination or during the multi-dose vaccination period to raise people’s awareness of such non-immune risks.
mutation
We should also keep in mind that the new coronavirus is a constantly evolving organism, and mutations continue to occur during the evolution process. Since August 24, 2020, there have been at least 4 confirmed cases of COVID-19 that may be caused by reinfection with different SARS-CoV-2 mutants in Hong Kong, the Netherlands, Belgium and the United States.
The most recent case of reinfection occurred 48 days after the initial infection, and the patient showed more severe clinical symptoms after being infected with the new SARS-CoV-2 mutant strain. These new cases not only make people doubt whether they can obtain herd immunity against COVID-19 infection, but also indicate that as the pandemic continues to develop in the community, it may be necessary to redesign the developed vaccine and continue to Develop a new COVID-19 vaccine.
Until scientists find the ideal way to treat the new coronavirus infection, vaccinating the global population will be the basic strategy for the current response to the COVID-19 epidemic. The numerous challenges in the process from vaccine development to application not only present us with arduous tasks, but also provide unprecedented opportunities for interdisciplinary cooperation and finding innovative solutions on a global scale. These are all for us to deal with future infectious diseases. The pandemic has accumulated experience.
It is difficult to say whether there will be infectious diseases or pandemics in the future. Therefore, the above experience will become a valuable experience left to humans in the struggle against disease in the COVID-19 era.
(source:internet, reference only)
Disclaimer of medicaltrend.org



