Medical Knlowledge: What’s the treatment of Nanobodies?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Medical Knlowledge: What’s the treatment of Nanobodies?
Medical Knlowledge: What’s the treatment of Nanobodies? “Cell” magazine (Cell) published an important paper on the development of COVID-19 antibodies online.
Scientists have found a variety of “nanobodies” in llamas, which can effectively neutralize SARS, MERS, and pseudoviruses of the new coronavirus in vitro. This research has once again aroused the industry’s attention to Nanobody technology. In fact, Nanobodies have huge application potential and prospects. Fierce Biotech once ranked Ablynx’s nanobody technology platform as the top ten technology platform in the field of biotechnology and pharmaceuticals in the next ten years.
What is a nanobody? Simply put, it is a type of antibody that only contains naturally occurring heavy chains and is much smaller in size than ordinary antibodies. Due to its unique structure, nanobodies have become ideal materials for creating new types of biopharmaceuticals with multiple competitive advantages. In fact, the concept of developing Nanobodies into medicines has been clinically verified. In 2018, the world’s first Nanobodies, Cablivi (caplacizumab), was approved for marketing in the EU.
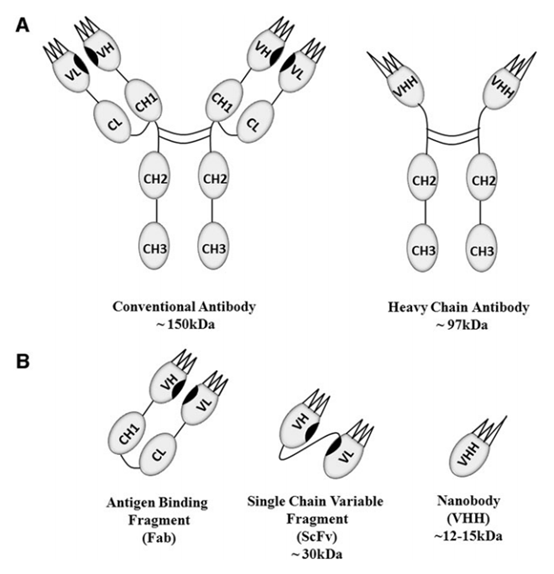
In 1989, Raymond Hamers et al. conducted a pioneering study on the immune system of dromedary camels, which marked the discovery of heavy chain therapeutic antibodies. Seven heavy chain antibodies are different from traditional antibodies in the light chain, and heavy chain antibodies have no changes.
And constant light chain and CH1 domain (Figure A below). Similar heavy chain antibodies have been found in carps such as sharks. However, these heavy chain antibodies are called IgNAR antibodies and have 5 constant (CH) domains. Due to the difficulties in immunizing sharks, engineering and development are challenging. .
Traditional antibodies contain 6 complementarity determining regions (CDRs) in the heavy and light chains, while heavy chain antibodies only have 3 CDRs (Figure B below). Although there are only 3 CDRs, these heavy chain-only antibodies exhibit comparable antigen binding affinity and other effector functions compared with traditional 6-CDR antibodies.
Nanobodies as cancer treatment
Advances in cancer immunology have paved the way for many new treatment strategies, including antibodies and nanobodies and their ability to detect tumor cells and activate the effector response of the immune system. These breakthrough cancer immunotherapy methods include the recognition and therapeutic inactivation of checkpoint suppression, the activation of antigen presenting cells (APCs), the blocking of immunosuppressive cells, the neutralization of immunosuppressive molecules, and chimeric antigen receptor T cells (CAR T cell) and CAR-Natural Killer (NK) cell development, cytokine regulation, etc.
Application of Nanobodies and T Cells in Cancer Immunotherapy
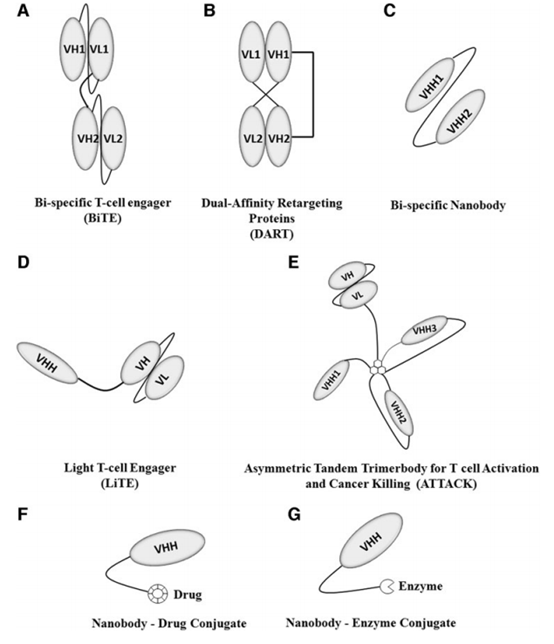
Currently, there are three types of bispecific antibodies that have specific benefits; bispecific T cell enzymes (BiTE), dual affinity and redirecting proteins (DARTs) and tandem two antibodies (TandAbs). BiTE antibodies are developed to T cells and tumor cells are connected and consist of two scFv fragments, one for T cell antigens/markers, such as CD3, and the other for TAA, plus a peptide linker. Blinatumomab is a BiTE approved by the Food and Drug Administration (FDA) for the treatment of B-cell acute lymphoblastic leukemia (B-ALL).
It is specific for CD3 of T cells and CD19 of B cells (overexpressed in ALL). Sex, connected with glycine-serine linker. This antibody shows good efficacy, but has a short half-life, which is a major problem of blinatumomab and other BiTEs. It requires high therapeutic doses to achieve the required T cell activation. DARTs have been developed as an alternative to Overcome the short half-life of BiTEs and solve the problem of rapid elimination. Different from BiTEs, DARTs have Het-erodimerized Fv fragments, Fv1 fragment has VL of target A and VH of target B, and Fv2 fragment has VL of target B and VH48 of target A (Figure 2B).

Compared with traditional BiTEs, bispecific nanobodies with significantly improved stability, solubility and performance are also expected to show higher efficacy. Recently, a bispecific antibody against T cell CD3 and breast cancer cell Her2 was developed. The uniqueness of this treatment method is the combination of a single domain (VHH) specific for Her2 and a scFv-fragment specific for CD3. This construct can be easily expressed in E. coli and carried out by affinity chromatography purification.
cd T lymphocytes
There are not many cd T lymphocytes, but they play a key role in anti-tumor activities. This small subset of T cells has many unique characteristics in the immune response. They do not require major histocompatibility complex (MHC) to be activated; they are stimulated by stress antigens. DNAM-1 (DNAX accessory molecule-1), CD27 and other stimulation.
There are some subsets of cd T lymphocytes–regulatory cdT and cdT17 cells promote tumor growth, while Vc9Vd2 T cells inhibit tumor growth, and have different activation molecules and pathways, which make them targeted for therapy. Many nanobodies Has been developed.
NK cells
NK cells are innate lymphocytes, which play a pivotal role in antiviral and antitumor immune responses. They do not require the presence of MHC to activate, and through many receptors, such as CD94/NKG2A, KIR, natural cytotoxic receptors NKp46, NKp30, NKp44, IgG receptor FccRIII and many other C-type lectin-like receptors, using activation and Suppressing (killing and non-killing) signals A large number of nanobody constructs have been developed to target FccRIII (CD16) of NK cells. Two camel nanobodies (C21 and C28) directed against the extracellular domain of FccRIII were generated in camels, which have significant affinity for FccRIIIb+polymorphine.
Nanobody-drug conjugate
Combining targeted therapies such as Nanobodies with non-targeted therapies such as chemotherapy/radiotherapy is an improvement over previous methods. Researchers use a VHH7 domain (for MHC class-II) as a therapeutic agent and also an imaging tool for B-cell lymphoma. When the VHH7 domain is conjugated with the thiomethansin derivative mertansine (DM1) and used as a treatment When used, it showed excellent specificity, internalization and cytotoxicity in a mouse model of A20 B-cell lymphoma, which resulted in a reduction in tumor growth and metastasis (Figure 2F).
The same VHH7 domain, when combined with near-infrared (NIR) fluorophores, exhibits excellent diagnostic performance in visualizing local and metastatic tumor cells. Also, as a new targeting construct, it can target radionuclide therapy and nanotechnology. The binding of antibodies is gaining great attention.
Nanobody enzyme conjugate is another nanobody-enzyme conjugate-based method, which has shown good activity in eliminating tumors. In 2004, scientists developed a nanobody enzyme conjugate, cAb-CEA5:bL to target tumor-related CEA114 (Figure 2G). The nanobody is conjugated with the Enterobacter cloacae b-lactamase enzyme, which can specifically activate the anti-tumor original drug 7-(4 carboxybutanamido cephalosporin mustard), making it an active drug phenylenediamine mustard. Conjugation is performed using llama c2c hinges to provide flexibility and stability, and show rapid clearance from the systemic circulation and concentration in the tumor, thereby avoiding off-target toxicity.
Nanobody-based CAR T cell therapy
In 2018, the first nanobody-based CAR T cell therapy was launched, using the VHH domain to target MUC-1, CD28 and OX40 as costimulatory molecules. The killing effect of CAR T cells on MUC-1+ tumor cells was observed in tumor xenotransplantation , And combined with the increased production of pro-inflammatory cytokines IL-17 and IFN-.
The NanoCAR system is further enhanced with a suicide gene system to avoid unnecessary damage to healthy cells and control unnecessary replication. In this system, one uses homodimer-regulated caspase 8, which is activated by the synthetic ligand AP20187 to induce apo-ptosis.
In addition to the tumor microenvironment, a major challenge in the treatment of solid tumors is tumor-specific target identification. In order to solve this problem, researchers from MIT and Harvard University have developed CAR T cells based on nanobodies, which target the general tumor microenvironment, especially PD-L1 and EIIIB, which are present in a variety of tumor types. These nano-CAR T cell therapies have shown good recognition and binding activity in many tumors, and can also secrete IL-2 and IL-12 when activated, which increases tumor inflammation.
Car T cell therapy based on bispecific nanobodies has also been developed, because relying on a single antigen for tumor recognition is usually not enough and leads to the failure of the treatment of antigen-negative tumors. In 2018, scientists developed two NanoCARs targeting CD20 and HER2; the antigen binding domain consists of two VHH tandem domains, targeting two different antigens on tumor cells. This NanoCar method overcomes the problem of antigen loss on tumors and eliminates The tumor has shown good potential.
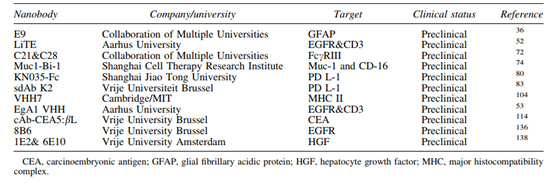
In addition, a nanobody-based anti-EGFR+ tumor-resistant UniCAR has also been developed. Unlike traditional CARs, the activity of this UniCAR can be regulated and targeted to tumor-specific antigens through recombination of targeting module epitopes, thereby eliminating unnecessary risks such as cytokine syndrome and CAR T cell overexpression. This Nanobody-based UniCAR shows controllable, substantial tumor cell lysis and good biodistribution, and has a long half-life. Some Nanobodies in pre-clinical development are listed in the table below.

Conclusion
Nanobodies have good dynamic properties, contract size, thermal stability, penetration ability (even through the BBB), high solubility and low immunogenicity, making them very promising therapeutic molecules.
Easy handling and low-cost production further increase their prospects as therapeutic drugs. They are used to treat many diseases, especially cancer, by activating effector cells and suppressing several dynamic strategies of immunosuppression.
Bispecific Nanobodies lacking the VL-VH domain exhibit impressive stability and extremely low degree of polymerization. Many naked antagonistic nanobody constructs have shown successful inactivation of tumorigenesis pathways by blocking ion channels and growth factor receptors.
Their tiny size shows the re-labeled tissue penetration and biodistribution of Nanobodies and Nanobody-drug conjugates, which opens the door to combat solid tumors and enhances the efficacy. Nanobodies have a good anti-tumor response in the application of photothermal therapy and photodynamic therapy.
Advances in synthetic biology have led to the development of probiotics, which can synthesize therapeutic anti-tumor nanoantibodies in the tumor microenvironment to avoid the toxicity challenge of conven- tional checkpoint inhibitors.
CAR T and CAR NK cells with nanobodies as variable domains have developed bispecific CAR T and CAR NK cells with excellent anti-tumor activity and tumor specificity. Their potential has attracted the interest of many pharmaceutical companies, and nanobodies have now become the main products in many drug pipelines.
Recently, the FDA approved CABLIVI nanobodies for the treatment of thrombotic thrombocytopenic purpura, further highlighting their appearance in the market, and they will undoubtedly continue to innovate treatment options.
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



