Is COVID-19 more harmful to men like making the genitals smaller?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Is COVID-19 more harmful to men like making the genitals smaller?
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Is COVID-19 more harmful to men like making the genitals smaller?
The COVID-19 pandemic has been going on worldwide for two years.
While posing a huge threat to human life and health, it has also continuously impacted human social order and economic development.
It is worth noting that many COVID-19 studies have shown that COVID-19 is more harmful to men, and the mortality rate of men among COVID-19 patients is also higher.
However, a new study from the GenderSci Lab at Harvard University shows that during the COVID-19 pandemic, gender disparities in COVID-19 vary widely across regions and over time, suggesting observed gender differences in COVID-19 It cannot be explained without reference to social background factors .
The study was published in Social Science & Medicine under the title: Sex disparities in COVID-19 outcomes in the United States: Quantifying and contextualizing variation [ 1] .

The study, led by Professor Sarah Richardson , director of the GenderSci Laboratory at Harvard University , is also the first to quantify changes in COVID-19 mortality rates across U.S. states and over time. The findings show that 30 percent of the U.S. gender disparity can be attributed to state-to-state differences and 10 percent to timing differences.
Prof Sarah Richardson said: “Gender differences should not be quickly assumed to be directly caused by sex-related biological factors. A focus on biology could limit the scope of public health engagement and create more vulnerabilities. If scientists By not focusing on gender-related social factors, they risk wasting time, energy and resources.”
Is COVID-19 more harmful to men? Even make the genitals smaller?
From the very beginning of the COVID-19 pandemic, scientists have noticed that the ratio of males and females and the death rate of patients with COVID-19 pneumonia are not the same.
In May 2020, a statistic showed that more than 70% of COVID-19 deaths were men, which means that the death rate for men is almost 2.5 times that of women.
In this regard, studies have shown that sex hormones are likely to be the real “culprit” of this difference.
In May 2020, the University of Groningen in the Netherlands published a research paper entitled: Circulating plasma concentrations of angiotensin-converting enzyme 2 in men and women with heart failure and effects of renin–angiotensin–aldosterone inhibitors in the internationally renowned medical journal European Heart Journal【2】.
The study, which analyzed clinical data from thousands of COVID-19 patients, showed that male patients have higher concentrations of the ACE2 receptor in the blood than females , and ACE2 is a key receptor for SARS-CoV-2 to invade human cells.
This will help explain why men are more susceptible to SARS-CoV-2.
In addition to this, more studies have found that the kidney and testis also have high levels of ACE2 receptor expression , therefore, these organs may also be potential infection targets of SARS-CoV-2.
Even more alarming is that in November 2021, a survey led by University College London (UCL) showed that more than 200 potential COVID-19 symptoms were identified in more than 3,700 patients with confirmed or suspected long-term infection of the COVID-19, These include ” reduced male genital size ” symptoms, although such symptoms are relatively rare.
In fact, as early as April 2021, an article in World J Mens Health found that 2 male patients with COVID-19s developed erectile dysfunction after recovery , and urologists found COVID-19s in the cells of their genitals virus particles [3] .

Judging from the above studies, SARS-CoV-2 is more harmful to men, which is reflected in the fatal consequences such as increased morbidity and mortality, compared with that of shortened genital length and erectile dysfunction.
Gender disparities in COVID-19 affected by region and time
So, are the gender differences in COVID-19 really as stark as the above studies suggest? Professor Sarah Richardson said gender disparities in COVID -19 varied widely across US states and were not volatile over the course of the pandemic.
For example, throughout the pandemic, the death rate among men in Texas has been higher, while in Connecticut, the death rate among women was higher than among men for 22 weeks.
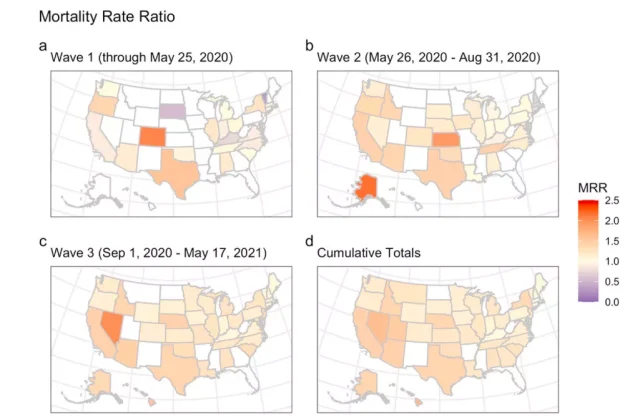
Gender differences in COVID-19 at different times and in different regions
Not only that, but gender differences are also very significant in the waves of major epidemics. For example, the gender disparity in cumulative death rates in New York was actually caused by the large gender disparity at the start of the pandemic.
In a related article currently in preprint, the research team demonstrated that 72.7% of additional male deaths in New York State occurred during the first wave of the pandemic between March 14 and May 4, 2020.
Since then, New York’s COVID-19 gender gap has narrowed considerably, approaching gender parity.
Ann Caroline Danielsen , the paper’s first author, noted: “Single-factor approaches, which focus on gender-related traits, cannot explain the changes we observe over time and geography.
Our data do not support the COVID-19 pandemic. gender-differentiated, stable, and long-term consistent views.”
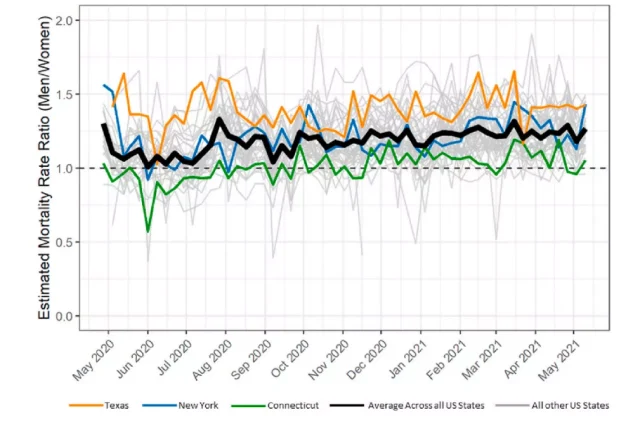 Predicting weekly death rates by state with regression models
Predicting weekly death rates by state with regression models
In fact, since the beginning of the COVID-19 pandemic, scientists have been attributing higher male COVID-19 mortality rates to factors related to biological sex, assuming that the pattern of sex differences is stable across context and time .
In contrast, this study concludes that there is little reason to believe that interventions centered on sex-related biological factors will play a major or substantial role in explaining and ameliorating sex differences.
Gender differences in COVID-19 need to be viewed rationally
Gendered health behaviors, occupational exposures, and pre-existing health conditions interact with differences in state-level responses, such as time and length of mask wearing, business closures, and school closures, which may lead to, at the state and timing, male and women differ in their vulnerability to severe consequences of COVID-19.
In addition, the study also shows that from April 27, 2020 to May 10, 2021, statistics show that the mortality rate of male COVID-19 patients is only 10-20% higher than that of women, which is 50% higher than the death rate claimed by the media The rate is much lower, similar to the persistent gap between male and female mortality rates that existed before the pandemic.
All in all, this study shows that the gender gap in COVID-19 is not as great as the media has advertised, depending on time and region. Therefore, we still need to be rational about gender differences in COVID-19 .
References :
1. Danielsen AC, Lee KM, Boulicault M, et al. Sex disparities in COVID-19 outcomes in the United States: Quantifying and contextualizing variation [published online ahead of print, 2022 Jan 10]. Soc Sci Med. 2022;294: 114716. doi:10.1016/j.socscimed.2022.114716
2. Sama IE, Ravera A, Santema BT, et al. Circulating plasma concentrations of angiotensin-converting enzyme 2 in men and women with heart failure and effects of renin-angiotensin-aldosterone inhibitors. Eur Heart J. 2020;41(19) :1810-1817. doi:10.1093/eurheartj/ehaa373
3. Kresch E, Achua J, Saltzman R, et al. COVID-19 Endothelial Dysfunction Can Cause Erectile Dysfunction: Histopathological, Immunohistochemical, and Ultrastructural Study of the Human Penis. World J Mens Health. 2021;39(3):466- 469. doi:10.5534/wjmh.210055
Is COVID-19 more harmful to men like making the genitals smaller?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Is COVID-19 more harmful to men like making the genitals smaller?
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Is COVID-19 more harmful to men like making the genitals smaller?
The COVID-19 pandemic has been going on worldwide for two years.
While posing a huge threat to human life and health, it has also continuously impacted human social order and economic development.
It is worth noting that many COVID-19 studies have shown that COVID-19 is more harmful to men, and the mortality rate of men among COVID-19 patients is also higher.
However, a new study from the GenderSci Lab at Harvard University shows that during the COVID-19 pandemic, gender disparities in COVID-19 vary widely across regions and over time, suggesting observed gender differences in COVID-19 It cannot be explained without reference to social background factors .
The study was published in Social Science & Medicine under the title: Sex disparities in COVID-19 outcomes in the United States: Quantifying and contextualizing variation [ 1] .

The study, led by Professor Sarah Richardson , director of the GenderSci Laboratory at Harvard University , is also the first to quantify changes in COVID-19 mortality rates across U.S. states and over time. The findings show that 30 percent of the U.S. gender disparity can be attributed to state-to-state differences and 10 percent to timing differences.
Prof Sarah Richardson said: “Gender differences should not be quickly assumed to be directly caused by sex-related biological factors. A focus on biology could limit the scope of public health engagement and create more vulnerabilities. If scientists By not focusing on gender-related social factors, they risk wasting time, energy and resources.”
Is COVID-19 more harmful to men? Even make the genitals smaller?
From the very beginning of the COVID-19 pandemic, scientists have noticed that the ratio of males and females and the death rate of patients with COVID-19 pneumonia are not the same.
In May 2020, a statistic showed that more than 70% of COVID-19 deaths were men, which means that the death rate for men is almost 2.5 times that of women.
In this regard, studies have shown that sex hormones are likely to be the real “culprit” of this difference.
In May 2020, the University of Groningen in the Netherlands published a research paper entitled: Circulating plasma concentrations of angiotensin-converting enzyme 2 in men and women with heart failure and effects of renin–angiotensin–aldosterone inhibitors in the internationally renowned medical journal European Heart Journal【2】.
The study, which analyzed clinical data from thousands of COVID-19 patients, showed that male patients have higher concentrations of the ACE2 receptor in the blood than females , and ACE2 is a key receptor for SARS-CoV-2 to invade human cells.
This will help explain why men are more susceptible to SARS-CoV-2.

In addition to this, more studies have found that the kidney and testis also have high levels of ACE2 receptor expression , therefore, these organs may also be potential infection targets of SARS-CoV-2.
Even more alarming is that in November 2021, a survey led by University College London (UCL) showed that more than 200 potential COVID-19 symptoms were identified in more than 3,700 patients with confirmed or suspected long-term infection of the COVID-19, These include ” reduced male genital size ” symptoms, although such symptoms are relatively rare.
In fact, as early as April 2021, an article in World J Mens Health found that 2 male patients with COVID-19s developed erectile dysfunction after recovery , and urologists found COVID-19s in the cells of their genitals virus particles [3] .

Judging from the above studies, SARS-CoV-2 is more harmful to men, which is reflected in the fatal consequences such as increased morbidity and mortality, compared with that of shortened genital length and erectile dysfunction.
Gender disparities in COVID-19 affected by region and time
So, are the gender differences in COVID-19 really as stark as the above studies suggest? Professor Sarah Richardson said gender disparities in COVID -19 varied widely across US states and were not volatile over the course of the pandemic.
For example, throughout the pandemic, the death rate among men in Texas has been higher, while in Connecticut, the death rate among women was higher than among men for 22 weeks.

Gender differences in COVID-19 at different times and in different regions
Not only that, but gender differences are also very significant in the waves of major epidemics. For example, the gender disparity in cumulative death rates in New York was actually caused by the large gender disparity at the start of the pandemic.
In a related article currently in preprint, the research team demonstrated that 72.7% of additional male deaths in New York State occurred during the first wave of the pandemic between March 14 and May 4, 2020.
Since then, New York’s COVID-19 gender gap has narrowed considerably, approaching gender parity.
Ann Caroline Danielsen , the paper’s first author, noted: “Single-factor approaches, which focus on gender-related traits, cannot explain the changes we observe over time and geography.
Our data do not support the COVID-19 pandemic. gender-differentiated, stable, and long-term consistent views.”
 Predicting weekly death rates by state with regression models
Predicting weekly death rates by state with regression models
In fact, since the beginning of the COVID-19 pandemic, scientists have been attributing higher male COVID-19 mortality rates to factors related to biological sex, assuming that the pattern of sex differences is stable across context and time .
In contrast, this study concludes that there is little reason to believe that interventions centered on sex-related biological factors will play a major or substantial role in explaining and ameliorating sex differences.
Gender differences in COVID-19 need to be viewed rationally
Gendered health behaviors, occupational exposures, and pre-existing health conditions interact with differences in state-level responses, such as time and length of mask wearing, business closures, and school closures, which may lead to, at the state and timing, male and women differ in their vulnerability to severe consequences of COVID-19.
In addition, the study also shows that from April 27, 2020 to May 10, 2021, statistics show that the mortality rate of male COVID-19 patients is only 10-20% higher than that of women, which is 50% higher than the death rate claimed by the media The rate is much lower, similar to the persistent gap between male and female mortality rates that existed before the pandemic.
All in all, this study shows that the gender gap in COVID-19 is not as great as the media has advertised, depending on time and region. Therefore, we still need to be rational about gender differences in COVID-19 .
References :
1. Danielsen AC, Lee KM, Boulicault M, et al. Sex disparities in COVID-19 outcomes in the United States: Quantifying and contextualizing variation [published online ahead of print, 2022 Jan 10]. Soc Sci Med. 2022;294: 114716. doi:10.1016/j.socscimed.2022.114716
2. Sama IE, Ravera A, Santema BT, et al. Circulating plasma concentrations of angiotensin-converting enzyme 2 in men and women with heart failure and effects of renin-angiotensin-aldosterone inhibitors. Eur Heart J. 2020;41(19) :1810-1817. doi:10.1093/eurheartj/ehaa373
3. Kresch E, Achua J, Saltzman R, et al. COVID-19 Endothelial Dysfunction Can Cause Erectile Dysfunction: Histopathological, Immunohistochemical, and Ultrastructural Study of the Human Penis. World J Mens Health. 2021;39(3):466- 469. doi:10.5534/wjmh.210055
Is COVID-19 more harmful to men like making the genitals smaller?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.
Is COVID-19 more harmful to men like making the genitals smaller? Is COVID-19 more…
co
Is COVID-19 more harmful to men like making the genitals smaller? Is COVID-19 more…
co



