Can COVID-19 vaccine also “anti-cancer”?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Can COVID-19 vaccine also “anti-cancer”?
Can COVID-19 vaccine also “anti-cancer”? Is it the truth or a rumor?
The COVID-19 pneumonia is still affecting our lives, even though the COVID-19 vaccine has already been vaccinated.
Breaking news: Cancer patients accidentally contracted COVID-19, and the tumors in their bodies disappeared by themselves?!
This news, at first glance, looks particularly like a rumor, but at a closer look, a “dongtian” that can change the status quo of cancer treatment is revealed before our eyes!
▌COVID-19 pneumonia makes cancer disappear? This is not a “rumor”
On January 2, 2021, the famous British hematology magazine “BJ Haem” published a paper reporting a 61-year-old male patient with malignant lymphoma in the Department of Hematology, Royal Cornwall Hospital.
In the case of the spread of the whole body and the failure of active treatment, this patient accidentally contracted the new coronavirus. After giving up all active treatments and only giving full symptomatic support to palliative treatment, the tumors of the patient’s body have subsided during the home recuperation process!
Later, after another PET/CT scan, it was confirmed that the tumor lesions of the patient’s whole body actually achieved “CR”, that is to say, this malignant blood cell tumor has completely disappeared!
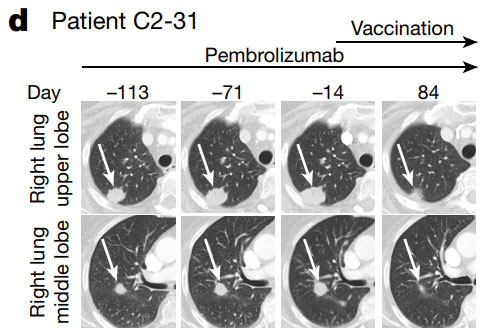
▲ The comparison of PET/CT before and after the patient was diagnosed with COVID-19, it can be clearly seen that the extensively spreading tumors have subsided later
How did the terrible new coronavirus pneumonia become the “savior” for patients with hematological malignancies? A closer look at the causes and consequences of this case revealed that the body’s immune system played an indispensable role.
The new coronavirus is very likely to trigger the body’s anti-tumor immune response. As the author of the paper speculated, the pathogen infected by this patient activated a specific T cell immune response, which “cross-reacted” with tumor antigens. In other words, activated T cells also have anti-tumor properties.
Another related cellular immune response is NK cells (natural killer cells). The author further speculates that the inflammatory factors produced after infection activate the body’s NK, which also has a tumor-killing effect.
What’s even more amazing is that this is not the only case in which the cancer “relapsed” caused by new coronavirus pneumonia! A patient with advanced lung cancer also experienced this “rebirth”.
Not long ago, Dr. Antonio Calles of the General Hospital of Gregorio Marañón University in Spain announced on social networks that a patient with advanced lung squamous cell carcinoma who had liver metastases contracted new coronavirus pneumonia after the cancer recurred, and also experienced complete tumor regression. Response (CR), whether it is a recurrence of lungs or metastases on the liver, all disappeared!
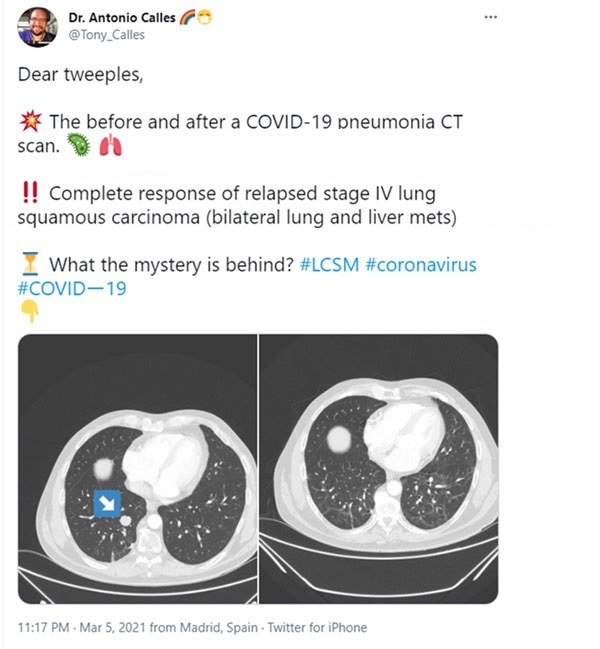
Since this situation is only a case, Antonio Calles did not make further reports, and it is estimated that further research is currently underway.
These case reports are undoubtedly “sensational” for patients. However, from the perspective of population data, the new coronavirus pneumonia does not allow most cancer patients to achieve “cure”.
It is this Dr. Antonio Calles who observed in detail 23 lung cancer patients with new coronavirus pneumonia. In the observation period of less than two months, the patient fatality rate was as high as 35% (8/23)! He pointed out in the conclusion of the paper: “During the COVID-19 epidemic, reducing the risk of viral infection is the key to protecting lung cancer patients”!
It seems that cancer is inextricably linked with viruses and other pathogens, and uncovering the principles behind these links is an opportunity to “defeat” it in the end!
In fact, attempts to uncover the relationship between cancer and pathogens are not uncommon in history. However, such attempts are basically at the stage of theoretical or pre-clinical research. The legendary Dr. William Colley tried to treat cancer with live streptococci and succeeded in sporadic cases. But in the end, this kind of microbial therapy failed to enter the mainstream treatment field of tumors.
All in all, the road to microbial anti-cancer is “long road and long”! On the whole, new coronavirus pneumonia is still the “public enemy” of people all over the world, and the idea of relying on this powerful infectious disease to fight cancer is very unreliable. Unless you have the luck of winning the “Super Lotto”, don’t put your hopes on it.
▌Can the COVID-19 vaccine technology be used to fight cancer? Really! And it is not far from practical application
Relying on the new coronavirus to fight cancer with “drugs” is currently undesirable. But don’t forget the analysis of the experts in those cases-“The ability to activate the body’s immune cells may be the key to fighting cancer cells.”
Yes, adhering to this idea, the design idea used by a COVID-19vaccine has gradually become the next cancer “killer”.
According to data from the World Health Organization, so far, more than 6 vaccines have been put into the global wave of anti-epidemic.
In addition to the traditional inactivated vaccines and live attenuated vaccines, there are two new types of vaccines that are put into use or research and development, namely adenovirus vector vaccines and mRNA vaccines. It is this new type of mRNA vaccine that has something to do with anti-cancer.
It turned out that on November 9 last year, the Phase III clinical data of the first COVID-19 vaccine confirmed that an mRNA COVID-19 vaccine had an effective rate of more than 90%. After a week, the effective rate was further updated to 95%. This number greatly exceeds the FDA’s requirement that the effective rate must be greater than 50%. A month later, the FDA approved this mRNA COVID-19 vaccine for marketing, and then approved another COVID-19 vaccine.
In less than a year, two mRNA vaccines were launched on the market, both for the COVID-19, which can be said to have created an unprecedented “miracle” in the history of vaccine development.
Soon, more explosive news came soon! The COVID-19 vaccine research and development agency-Moderna, reported another mRNA vaccine-mRNA-4157 (remember this number) for the clinical trials of 10 patients with advanced head and neck cancer The trial was successful! The total remission rate reached 50%, and the disease control rate (DCR) reached 90%! Moreover, this mRNA vaccine has been confirmed to be effective against a variety of solid tumors!
It is 90% effective for new coronavirus pneumonia and 90% control for cancer treatment. This is an extremely rare number, all of which fall on the mRNA vaccine!
BioNTech, another research and development institution for COVID-19 vaccines, is also “fruitful” in the field of anticancer vaccines. As early as last year, they announced in the journal Nature that the cancer vaccine BNT111 (remember this number) has achieved curative effects in the treatment of melanoma.
Moreover, BioNTech’s vaccine breaks down the harsh requirements of general mRNA vaccines for low temperature (below -70°C), as long as they are stored in a refrigerator. This greatly reduces the threshold for the use of mRNA vaccines. At present, BNT111 has started the second phase of clinical trials, which is one step closer to being widely used in cancer patients.
The two research and development institutions of the COVID-19vaccine actually “success in the first battle” in the cancer field. This news has made American cancer patients on social networks not calm. They quickly confused the “similarities and differences” of the two vaccines and spread that “the COVID-19 vaccine is helpful.” “Anti-cancer” news! And, in the absence of clinical data to support, look for vaccinations everywhere.
The reality is that the cancer vaccine developed by the two companies is only the same technical route as the COVID-19 vaccine. Under a simple explanation, the COVID-19 vaccine uses the mRNA of the virus S protein, and the anti-cancer vaccine uses the mRNA of a certain type of cancer cell-specific protein. Although they are all mRNA vaccines, the immune activation information they carry is quite different.
However, if we go deeper, mRNA vaccine can not only help humans prevent COVID-19, but also break the cancer “curse”. How does it do it?
▌Why can innovative vaccine technology fight cancer? Ultra-high R&D efficiency creates a miracle of tumor immunity
To put it simply, a vaccine is to introduce a part (antigen) of a virus that is not pathogenic to the human body, and by stimulating the human body to produce a specific immunity, when the next time you encounter a similar virus, you will not be afraid of regenerating disease.
Vaccine research and development, no matter how complicated, whatever route it takes, to put it bluntly is to make antigens. The so-called “antigen” is actually the “fragment” of the virus that stimulates the body’s immunity, and its main component is generally protein.
The COVID-19 vaccine uses the spike protein of the COVID-19 virus, also known as the S protein. This protein is one of the important components that stimulate the immune response. Simply importing S protein into the human body is not enough to make people infected with new coronavirus pneumonia, so it is safe.
The traditional inactivated vaccine is to find the antigen directly from the virus. The virus is cultivated in the laboratory, and then chemically put to death to obtain the S protein. At this time, the dead virus loses its virulence, but its “fragments” retain immunogenicity, and will trigger an immune effect as soon as it enters the body. At present, most of the vaccines released and used by the CDC are traditional inactivated vaccines.
The mRNA vaccine is different. Instead of looking for the virus for antigen, it uses the genetic information of the antigen, that is, mRNA as the “engineering blueprint” to “create” the S protein antigen component in human cells. Come.
▌Tips
mRNA mRNA, also called “messager RNA”, is an intermediate molecule that transmits cell genetic information from DNA to protein macromolecules. The genetic code carried by DNA needs to be transcribed into corresponding mRNA before it can be further “translated” into protein molecules. , The latter further forms a variety of colorful life phenomena.
As early as January last year, China announced the genetic sequence of the new coronavirus to the world. Therefore, as long as the mouse clicks on the website, all the genetic information of the S protein can be obtained, and there is no need to risk “biochemical leakage” to cultivate the new coronavirus.
In this way, the mRNA with the S protein gene information is created through artificial synthesis. After entering the human body, it can automatically guide the cells to produce viral antigens.
Similar to viruses, cancer cells are different from normal cells. As long as you understand the genetic information of these cancer antigens, you can artificially synthesize a piece of mRNA. The cancer antigens “made” by the input cells are also anti-cancer immunogenic!
It’s simple to say, but not easy to do.
Before practical application, Hungarian scientist Katalin Kariko successfully laid the foundation for the use of mRNA after more than 20 years of research.
She first stabilized the reaction strength of mRNA in the body, and then introduced a “lipid delivery system” to put the mRNA into special nano-lipid particles, and successfully transport the active and stable mRNA molecules into the organism.
This mRNA vaccine was first designed for difficult diseases such as cancer.
Entering 2020, as the COVID-19 epidemic spreads across the world, it poses unprecedented challenges to vaccine design and production. The technology of using mRNA to rapidly synthesize vaccines just came in handy.
How fast is the development efficiency of mRNA vaccines? You may not imagine!
From gene sequencing information to the first injection, Moderna’s new coronavirus vaccine took only 63 days from design to application. It was approved only 12 months from the first appearance of the new coronavirus! This is a traditional vaccine, no matter whether it is an inactivated vaccine or an adenovirus vaccine, it cannot be matched.
And this kind of super-high research and development efficiency vaccine is applied to cancer, it is not a day or two.
▌New mRNA cancer vaccines live up to expectations: initial research results are remarkable
In July 2020, “Nature” magazine published the results of the BioNTech cancer vaccine-BNT111. The researchers made the four cancer antigens of malignant melanoma (the four gene sequences in the figure below) into mRNA vaccines.
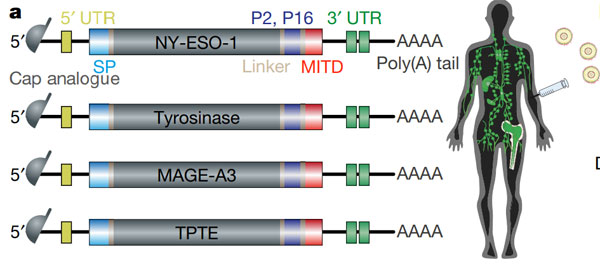
After the patient has developed resistance to immunotherapy, through the use of vaccine alone or in combination with PD-1 antibody, many cancer patients have turned around again!
The imaging results of the tumor changes in two of the patients (below) can particularly illustrate the problem: the introduction of vaccines actually made the tumors “relapsed” after the use of pembrolizumab.

In this process, cancer vaccine is like a “booster” that ignites tumor-specific immunity, and it has a “perfect match” with PD-1 antibody, successfully “repelling” tumors that are difficult to treat by conventional methods.
Moderna, another mRNA research and development organization, has a bigger layout in the field of cancer-related mRNA molecules!
According to the official website, they have introduced at least 5 mRNA molecules into cancer clinical research, including 2 cancer vaccines and 3 immune activators, and they have achieved remarkable results!
The success of mRNA vaccines may mean that in the field of cancer vaccines, humans have entered the final stage of sprint. Relying on vaccines to “defeat” cancer for more than half a century of “eagerness” is finally about to become a reality!
(source:internet, reference only)
Disclaimer of medicaltrend.org



