What is BTLA-HVEM in tumor immunity?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
What is BTLA-HVEM in tumor immunity?
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
What is BTLA-HVEM in tumor immunity?
Preface
Immunotherapy has changed the current mode of cancer treatment, especially immune checkpoint inhibitors, which have achieved remarkable results in cancers such as melanoma.
Immune checkpoint inhibitory antibodies including CTLA-4, PD-1/PD-L1 are approved by the FDA for the treatment of multiple cancer types.
However, only 20-30% of cases have observed a long-lasting response. Therefore, there is an urgent need for new immunotherapy targets.
BTLA ( CD272 ) is another important co-inhibitory receptor, and its ligand is the herpes virus invasion mediator (HVEM).
Although BTLA has similarities with PD-1 and CTLA-4, they differ in expression and function.
HVEM is widely expressed in various cell types and participates in immune homeostasis.
The expression of HVEM is up-regulated in a variety of tumors, and targeting BTLA and HVEM shows very promising application potential in tumor immunotherapy.
BTLA and WHO
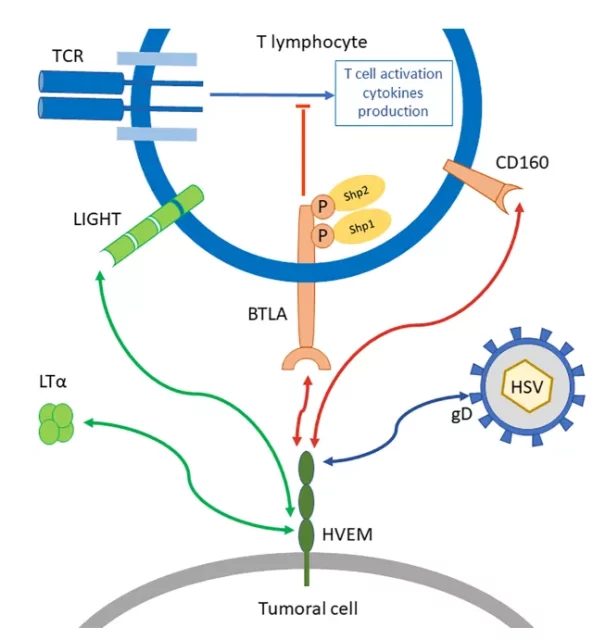
BTLA belongs to the CD28 family and has structural similarities with PD-1 and CTLA-4. It has an extracellular immunoglobulin domain, an immunoreceptor tyrosine inhibitory motif ( ITIM ), and an immunoreceptor tyrosine-based switch motif ( ITSM ).
BTLA signal transduction includes phosphorylation of ITIMs and the combination of phosphatase 1 ( SHP-1 )/SHP-2 containing SH2 domain , thereby inhibiting T cell proliferation and cytokine production.
In healthy people, naive CD4+ and TCD8+ T cells from peripheral blood have higher BTLA expression.
During the period of CD4+ differentiation, the expression of BTLA remained at a high level, while during the period of CD8+ T cell differentiation, the expression of BTLA was down-regulated.
Similar results were also observed on γδ-T cells. BTLA was highly expressed on quiescent Vγ9Vδ2 cells ( the main γδ-T cell subset in human peripheral blood ) and was down-regulated during Vγ9Vδ2 differentiation.
In vitro BTLA blockade enhances the proliferation of CD8+ T cells. In addition, BTLA-positive DC cells participate in peripheral Treg induction.
These data emphasize the importance of BTLA in immune homeostasis.
HVEM ( TNFRSF14 ) is a member of the TNF receptor family. HVEM is highly expressed in the lung, kidney and liver, moderately expressed in the heart, placenta, skeletal muscle and pancreas, and extremely low in the brain.
Among immune cells, HVEM is strongly expressed by quiescent T cells and B cells, NK cells, Tregs, monocytes, and DCs.
Mesenchymal cells and epithelial cells also express HVEM. In epithelial cells, HVEM expression plays a key role in innate mucosal defense against pathogens
The interaction between HVEM and BTLA is the earliest connection between the Ig structure and the TNFR family.
HVEM has other ligands besides BTLA, such as CD160, LIGHT, lymphotoxin-α ( LTα ) and herpes simplex virus glycoprotein D.
When HVEM is combined with LIGHT or LTα, it transmits a co-stimulatory signal, and when HVEM is combined with BTLA or CD160, it triggers a co-inhibitory signal.
Therefore, HVEM is generally described as a molecular switch that depends on the attached ligand.
However, HVEM-/- mice have increased response to T cell stimulation and increased susceptibility to autoimmune diseases, indicating that the co-inhibitory signal of HVEM is stronger than the co-stimulatory signal.
The role of HVEM in tumors
Upregulation of HVEM in tumors represents an immune escape mechanism, similar to tumor cells overexpressing PD-L1 or PD-L2.
HVEM is overexpressed in some tumors and shows that tumor-infiltrating T cells are BTLA positive. In addition, high expression of HVEM is associated with a significantly poorer prognosis.
In another study of 136 gastric cancer biopsies, increased expression of HVEM was associated with disease progression and decreased overall survival.
In another study on glioblastoma, through IHC evaluation of 34 glioma tissues, HVEM expression was located in the surrounding necrotic area and microvascular proliferation area.
According to transcriptomics analysis, HVEM expression is related to immune cell infiltration and stromal cells in the microenvironment.
The expression of HVEM is also related to the expression of PD-1, PD-L1, CTLA-4, LAG-3, and VISTA.
Therefore, HVEM plays a vital role in the regulation of immune and inflammatory responses, especially T cells. activation.
In summary, these data indicate that the upregulation of HVEM is closely related to the tumor progression and aggressiveness of many solid cancers.
The role of BTLA in tumors
BTLA expression in tumors
Studies have shown that the expression of BTLA in malignant tissues is higher than that in normal tissues, and higher BTLA expression is positively correlated with higher HVEM expression.
In addition, BTLA expression affects the prognosis. The 5-year overall survival rate ( OS ) of the low BTLA expression group was 48.3%, and it dropped to 17.9% when the BTLA expression was high.
Higher BTLA expression is also associated with lymph node metastasis.
BTLA is related to the expression of other co-inhibitory receptors.
In advanced melanoma, Fourcade et al. demonstrated that 42% of NY-ESO-1-specific CD8+ T lymphocytes co-express BTLA and PD-1, and these cells have a partially dysfunctional phenotype. When NY-ESO-1 specific CD8+ T lymphocytes are stimulated by a homologous antigen for a long time, TIM-3 and PD-1 are up-regulated.
BTLA expression follows a different pattern, which suggests that BTLA upregulation depends on different conditions, rather than functional exhaustion driven by high antigen load.
In addition, blocking BTLA with anti-BTLA antibodies can enhance the production of IFN-γ, TNFα and IL-2 by NY-ESO-1 specific CD8+ T cells.
Interestingly, when anti-BTLA is combined with anti-PD-1, a synergistic effect is observed in the functional analysis.
BTLA: an important part of T cell exhaustion
In lung cancer, the expression and function of BTLA are unclear, however, some key data have been reported.
In a mouse model of subcutaneous lung tumor implantation, Mittal et al. showed increased BTLA on CD4+ and CD8+ T cells, as well as other co-inhibitory markers, such as PD-1 and 2B4.
Thommen et al. confirmed and expanded the study in human lung tumor samples.
The study conducted a detailed immunophenotyping of TIL in NSCLC biopsy, and found that the expression of PD-1 and Tim-3 in advanced tumor-infiltrating CD8+ T cell subsets increased.
The percentage of BTLA positive cells is quite low, but follows the same pattern as PD-1 and TIM-3.
BTLA+CD8+T cells also highly express other co-inhibitory receptors, indicating that BTLA is up-regulated in the later stages of T cell exhaustion. Studies believe that the sequential expression of co-inhibitory receptors begins with PD-1, then TIM-3, CTLA-4 and LAG-3, and finally BTLA.
In fact, PD-1 blockade can partially rescue T cell functions that depend on PD-1 expression.
However, only CD8+ T cells with moderate PD-1 expression can benefit from anti-PD-1 therapy, and CD8+ T cells with high PD-1 expression are deeply depleted and cannot recover their function.
It is worth noting that, compared with the PD-1int subgroup, the PD-1high subgroup also expresses a higher number of TIM-3, CTLA-4, LAG-3 and BTLA.
Therefore, the joint strategy with PD-1 blocking is a direction worth exploring.
It is worth noting that Lou et al. studied the correlation between epithelial mesenchymal transition ( EMT ) and immune activation in lung cancer , confirming that EMT is closely related to the transcriptomic characteristics of inflammation.
In addition, in tumors showing EMT, the transcriptome expression of immune checkpoints, including BTLA, is increased and is associated with the recruitment of regulatory T cells.
This indicates that EMT can be regulated by the inflammatory microenvironment through a BTLA-dependent mechanism, which opens up a new research field for exploring the expression of BTLA on non-immune cells.
At present, Junshi Biologics anti-BTLA monoclonal antibody TAB004 (JS004) is in the clinical stage ( NCT04278859, NCT04137900 and NCT04477772 ).
Summary
In short, BTLA-HVEM does participate in immune escape in tumor immunity. In fact, the up-regulation of HVEM by tumor cells participates in suppressing anti-tumor immunity through BTLA, leading to disease progression and poor prognosis.
Blocking the inhibition triggered by BTLA can further improve the function of tumor infiltrating lymphocytes, and the combined blocking of BTLA and PD-1 shows a significant synergistic effect.
Therefore, targeting BTLA or HVEM is a promising new direction.
references:
1.BTLA-HVEM Couple in Health and Diseases:Insights for Immunotherapy in Lung Cancer. Front Oncol. 2021; 11: 682007.
What is BTLA-HVEM in tumor immunity?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.