Nature: Super bacteria had existed before antibiotics were used
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Nature: Super bacteria had existed before antibiotics were used
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Nature: Super bacteria had existed before antibiotics were used.
Antibiotic resistance of bacteria can cause human infections. It was previously thought that this was only a modern phenomenon and was caused by the clinical use of antibiotics.
The abuse of antibiotics is accelerating this process, and antibiotic resistance worldwide has risen to a high-risk level.
On January 5, 2022, researchers from Cambridge University, Wellcome Sanger Institute, Danish National Serum Institute, and Royal Botanic Gardens collaborated and published a paper on Antibiotics, entitled: Emergence of methicillin resistance predates the clinical use of antibiotics .
The study found that about 200 years ago, when antibiotics were not discovered and used, super bacteria appeared on hedgehogs.
It was the result of co-evolutionary adaptation of Staphylococcus aureus against colonizing dermatophytes in hedgehogs .
This study overturns the widely believed view that the abuse of antibiotics leads to the emergence of superbugs , because superbugs appeared on hedgehogs long before the use of antibiotics, which is more likely to be a natural evolutionary biological process.

Methicillin -resistant Staphylococcus aureus ( MRSA ) is one of the most common antibiotic-resistant bacterial pathogens, causing approximately 171,000 invasive infections each year in Europe alone.
In 1960, after the introduction of methicillin (celbenin) as a treatment option against penicillin Staphylococcus aureus clones, MRSA was first discovered.
Subsequently, methicillin resistance appeared in many Staphylococcus aureus clones around the world, which had serious adverse effects on the treatment of infections.
Currently, the World Health Organization considers MRSA to be an important threat to human health.
The methicillin resistance of Staphylococcus aureus is mediated by the mecA and mecC genes, which encode penicillin binding protein 2a (PBP2a) and PBP2c enzymes, respectively.
mecA and mecC are resistant to almost all β-lactam antibiotics , including penicillins that are not resistant to penicillinase (such as penicillin G) , penicillins that are resistant to penicillinase (such as methicillin), and cephalosporins (such as cefoxitin) ) .
Hedgehog surveys from Denmark and Sweden show that the prevalence of mecC- carrying MRSA (mecC-MRSA) is surprisingly high , indicating that the evolution of these bacteria may be driven by natural selection in wild animals, rather than the clinical use of antibiotics that is now generally believed. This study is to test this hypothesis.

Image source: PIA B. HANSEN
mecC-MRSA is widely distributed in hedgehogs
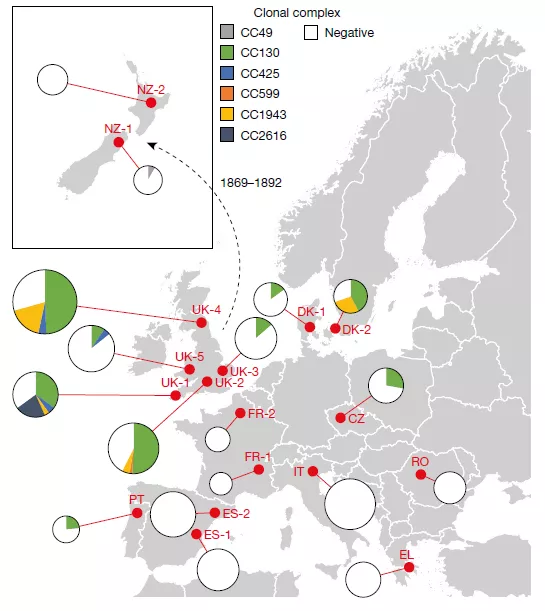
The researchers first examined the geographic distribution and population structure of mecC-MRSA in European hedgehogs.
The researchers analyzed a total of 828 samples of the nose, skin and feet of 276 hedgehogs from 16 wildlife rescue centers in 10 European countries and 2 wildlife rescue centers in New Zealand.
Surprisingly, mecC-MRSA exists in England and Wales (66%, 81 out of 123) , Czech Republic (50%, 6 out of 12) , Denmark (50%, 22 out of 22). 11) , Portugal (29%, 2 of 7) and New Zealand (6%, 1 of 17) hedgehogs.
Therefore, mecC-MRSA presents a wide geographic distribution on hedgehogs .
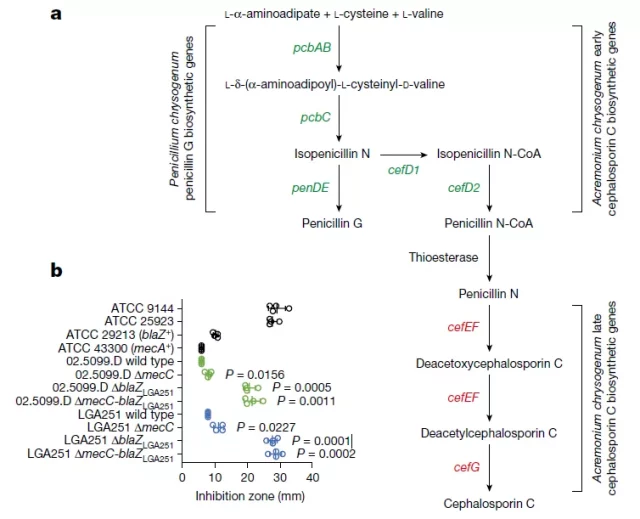
T. erinacei produces β-lactam
Researchers have discovered that Trichophyton erinacei ( T. erinacei ) produces two β-lactam antibiotics, which provide a natural selective environment.
In this environment, MRSA isolates have advantages over sensitive isolates.
To put it more succinctly, the hedgehog’s skin carries fungi and bacteria, and the two have fought a protracted battle for survival. Fungi secrete antibiotics to kill bacteria, but bacteria have evolved antibiotic resistance-namely MRSA .
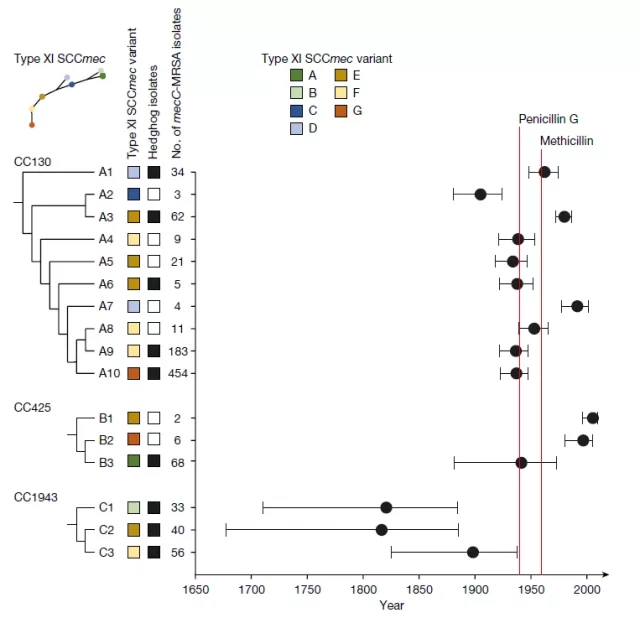
The evolutionary history of mecC-MRSA
Next, the researchers inferred the evolutionary history of Staphylococcus aureus (Methicillin-susceptible S. aureus, MSSA) CC130, CC425, and CC1943, which constitute the most successful mecC-MRSA clone in Europe.
To this end, the researchers collected and sequenced 786 mecC-MRSA and 127 MSSA CC130, CC425 and CC1943 isolates to represent the known geographic distribution (mainly Western and Central Europe) and host (mainly human, Cattle, sheep, goats and wild animals) .
The researchers used core genome SNP diversity and isolation dates to infer these isolates, as well as 205 mecC-MRSA and 9 MSSA CC130, CC425, and CC1943 isolates collected from hedgehogs.
For sequencing data processing and analysis, the researchers traced the genes that make mecC-MRSA antibiotic-resistant, and traced them back to their first appearance, and discovered that they appeared in the 19th century .
This suggests that the initial appearance of MRSA was not caused by the use of penicillin, but a natural biological process. “We believe that MRSA evolved in the battle for survival on the skin of hedgehogs and then spread to livestock and humans through direct contact , ” said Wellcome Sanger and researcher Ewan Harrison of the University of Cambridge .
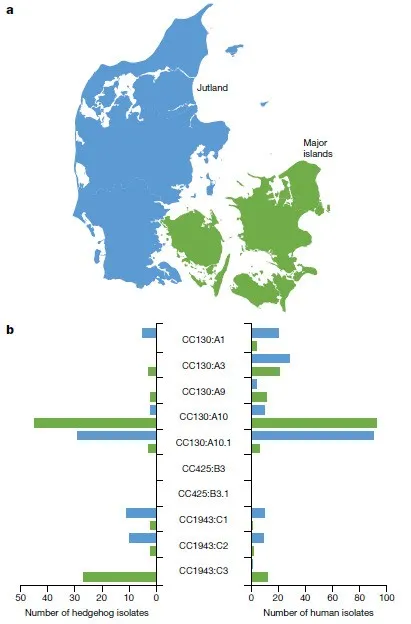
Population dynamics of mecC-MRSA
Hedgehogs constitute a large library of mecC-MRSA clones , and mecC-MRSA isolates appear much less frequently in humans, domestic animals, and other wild animals.
Hedgehog isolates exist in 9 of 16 mecC-MRSA pedigrees, including the 8 largest (≥ 25 isolates)and 3 earliest(200-130 years ago)pedigrees.
The two largest mecC-MRSA CC130 lineages (CC130:A9 and CC130:A10) account for 67% (232 of 344) and 65% (520 of all mecC-MRSA isolates from hedgehog, human, and other sources ) , respectively 339) and 43% (66 out of 153) , and have the widest geographic coverage in Western and Central Europe.
In summary, these studies indicate that methicillin resistance appeared before the use of antibiotics and was the result of co-evolutionary adaptation of Staphylococcus aureus against colonizing dermatophytes in hedgehogs .
This study overturns the widely believed view that the abuse of penicillin leads to the emergence of superbugs , because superbugs appeared on hedgehogs long before the use of antibiotics, which is more likely to be a natural evolutionary biological process.
Since almost all the antibiotics we use today come from nature, it is likely that resistance to them already exists in nature. In humans or livestock, excessive use of any antibiotic will benefit the resistant strains of bacteria, so it is only a matter of time before antibiotics begin to lose their effectiveness.
As Ewan Harrison said, “Wild animals, livestock, and humans are all interconnected.
We share an ecosystem. Only by looking at the entire system can we understand the evolution of antibiotic resistance. “
When we understand the world, we should not be stuck in a corner, let alone think in a fixed way, because nothing in the world is absolute truth.
It is worth mentioning that these findings cannot be a reason for us to be afraid of hedgehogs , because humans are rarely infected with mecC-MRSA, and it has existed in hedgehogs for more than 200 years.
And not only hedgehogs carry antibiotic-resistant bacteria, all wild animals carry many different types of bacteria, parasites, fungi or viruses and other microorganisms.
Paper link :
https://www.nature.com/articles/s41586-021-04265-w
Nature: Super bacteria had existed before antibiotics were used
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



