Cell: Why does the new coronavirus attack multiple organs and tissues?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Cell: Why does the new coronavirus attack multiple organs and tissues?
Cell: Why does the new coronavirus attack multiple organs and tissues? “Cell” magazine recently released the results of a pathological study by Chinese scientists on the new coronavirus. The results show that the virus can cause damage to all organs throughout the body, and the culprit is not necessarily the ACE2 receptor in the patient’s body, but the cathepsin L1 in the lungs.
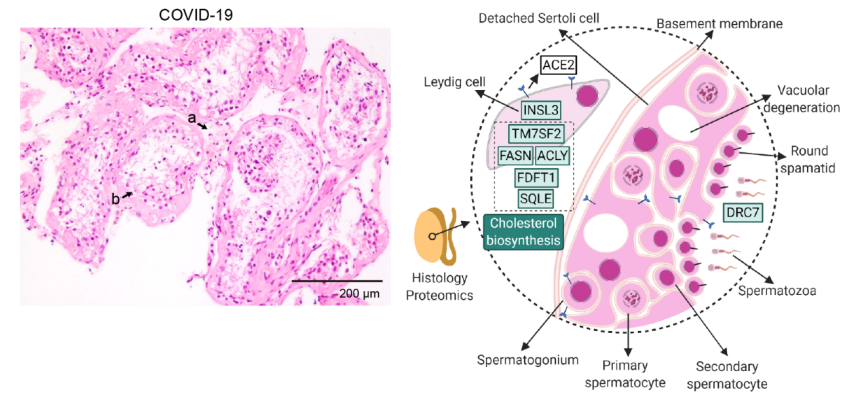
Since the discovery of the new coronavirus, clinical experts have discovered that this virus not only attacks the lungs, but also causes damage to organs throughout the body, including the heart, brain, kidneys, and fundus of the eyes. According to expert analysis, the concentration of ACE2 receptors in damaged organs is very high, which is the channel for viruses to invade cells. It is speculated that ACE2 receptors are the key factor leading to the aggravation of viral infections.
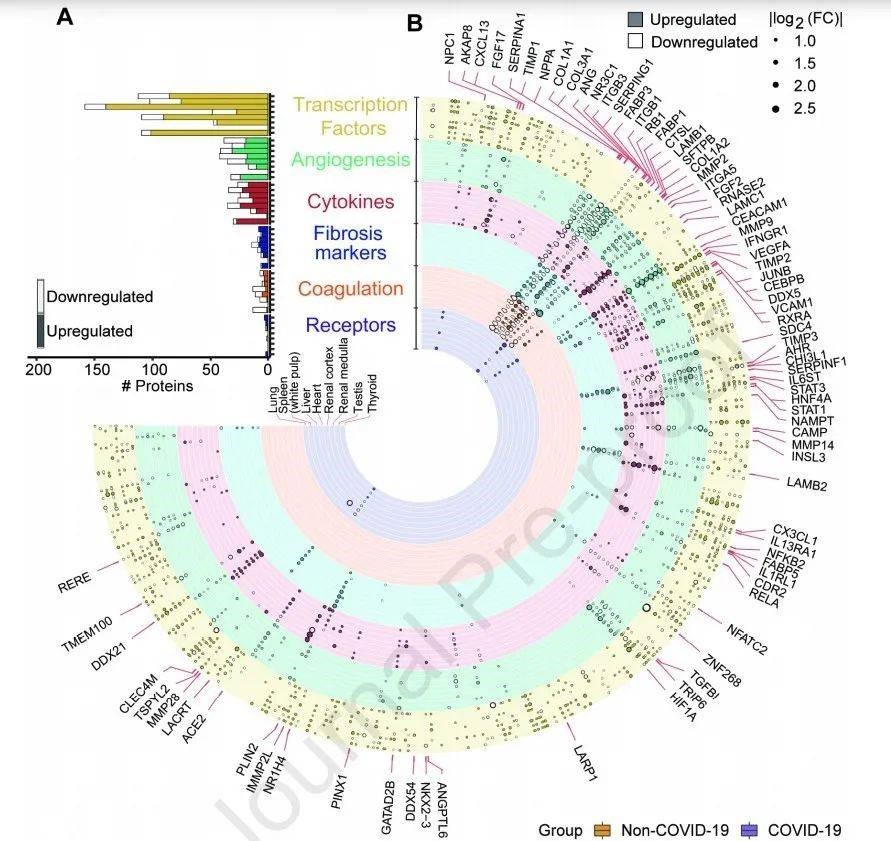
The Xia Jiahong/Hu Yu team of Huazhong University of Science and Technology in China and the Guo Tiannan team of West Lake University issued a paper pointing out that the molecular pathology of multiple organ injuries in patients with new coronavirus pneumonia is still unclear, hindering the progress of drug research. In this study, researchers performed proteomic analysis of 144 autopsy samples from 7 organs of 19 patients with new coronavirus pneumonia. The researchers quantified 11,394 proteins in these samples, of which 5,336 were significantly changed in at least one organ of patients with new coronavirus pneumonia.
The data shows that the expression of lung cathepsin L1 is significantly up-regulated in the lungs of patients with new coronavirus pneumonia. Proteomics data shows that the new coronavirus infection may cause excessive inflammation, which in turn causes the destruction of the gas exchange barrier in the lungs, which leads to hypoxia, angiogenesis, coagulation and fibrosis in the lungs, kidneys, spleen, liver, heart, and thyroid. Lung cathepsin L1 may act as an important host factor to induce cytokine overexpression in the COVID-19 infection and promote tissue fibrosis.
It is worth mentioning that the research team found that there is no significant difference in the number of ACE2 receptors in various organs of patients with non-new coronavirus pneumonia compared with patients with new coronavirus pneumonia. However, lung cathepsin L1, which helps viruses enter cells, has increased significantly in the lungs of patients with new coronavirus disease. This suggests that ACE2 is only a channel for the new coronavirus to enter the human body, but lung cathepsin L1 may be a potential therapeutic target to block virus invasion.
In summary, the study described the multi-organ proteomics profile of the deceased with new coronavirus pneumonia, and provided new clues for the prevention and treatment of new coronavirus pneumonia. Of course, these studies are based on tissue samples from patients who died from tCOVID-19. Whether the same changes will occur in mild and severe patients, and whether such changes are reversible, still needs further research.
(source:internet, reference only)
Disclaimer of medicaltrend.org



