Complications of mannitol and principles of clinical application
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Complications of mannitol and principles of clinical application
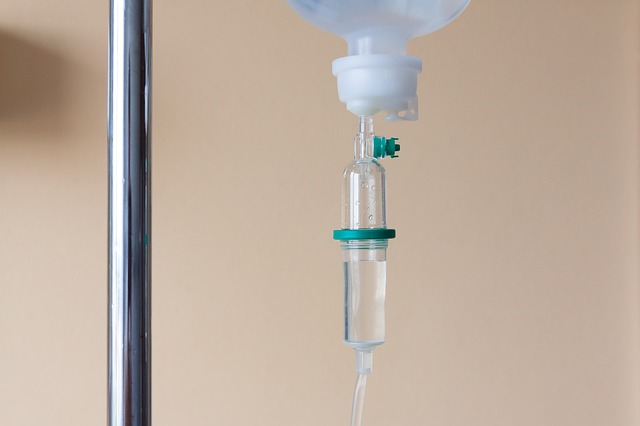
Complications of mannitol and principles of clinical application. Mannitol injection is a supersaturated solution and should be instilled separately. If electrolytes such as potassium chloride and dexamethasone are added, mannitol will be salted out to produce crystals.
Mannitol is a kind of drug that we have many clinical applications. Today we look at some of the problems of mannitol used in reducing intracranial pressure.
The effect of mannitol in lowering intracranial pressure is not only a simple diuresis, but also mainly to increase blood osmotic pressure, so that water in the brain tissue can be absorbed into the blood, thereby reducing cerebral edema and lowering intracranial pressure.
1. Complications of mannitol
Generally, it takes effect within 20 minutes after intravenous injection, and the antihypertensive effect reaches its peak in 2-3 hours and can be maintained for 4-6 hours. The usual dose is 0.25-0.5 g/kg. One dose per adult. However, many years of clinical practice has proved that mannitol can cause hypokalemia, induce or aggravate heart failure, hematuria, renal insufficiency, renal failure, and allergic reactions, in addition to the following complications:
⑴ Make brain edema worse
Mannitol dehydration to lower intracranial pressure depends on the integrity of the blood-brain barrier (BBB). Mannitol can only remove water from normal brain tissue, and not only has no dehydration effect on damaged brain tissue, but also due to the destruction of the blood-brain barrier. Mannitol can enter the brain tissue of the lesion area through the ruptured blood vessel, causing the formation of cerebral edema in the lesion to accelerate and increase in severity.
For patients with cerebral ischemia, due to the increased permeability of the blood vessels in the ischemic area, mannitol molecules easily enter the intercellular space of the ischemic area from the blood vessels. At the same time, because mannitol cannot be metabolized, excessive accumulation leads to reverse osmosis, which makes The edema in the ischemic area worsened. Clinical animal tests have also confirmed that it can reduce cerebral pressure and reduce cerebral edema 5 times before. The edema worsened after 5-7 times.
⑵ Obvious rebound of intracranial pressure
When the mannitol in the blood is rapidly excreted by the kidneys, the blood osmotic pressure is significantly reduced, so that the water moves from the blood to the brain tissue and the intracranial pressure rises again.
⑶ Intracranial hemorrhage worsens
The previous view believed that intracerebral hemorrhage was a short process of about 30-40 minutes, and it stopped with the appearance of blood clots; but with the continuous development of imaging and the clinical application of CT and MRI, it was found that there were about 38 % Of patients with cerebral hemorrhage have a hematoma within 24 hours after the onset, especially within 6 hours, and its expansion range is about 33%. In addition to the body’s own factors, it is mainly related to the improper use of mannitol.
The main cause of rebleeding caused by mannitol is
① After mannitol dehydrates the brain tissue outside the hematoma, it can rapidly increase the pressure gradient between the hematoma and the brain tissue, and reduce the support of the brain tissue, thereby expanding the early hematoma;
②On the other hand, because mannitol rapidly absorbs brain tissue fluid into the blood, short-term hypervolemia occurs, which further increases blood pressure and aggravates active cerebral hemorrhage.
2. Application principles of mannitol:
(1) According to the patient’s clinical symptoms and actual needs, determine the dosage and usage of the dehydrating agent. And closely observe the dynamic changes of intracranial pressure, adjust the treatment plan, achieve effective control, and rational use of drugs.
(2) Those with impaired consciousness, suggesting that the lesion is large and the midline structure has been affected, can be given 125ml of 20% mannitol, intravenous drip, q4-6h, and observe the dynamic changes of the condition and disturbance of consciousness, pay attention to the symptoms after medication Whether it is relieved, so as to adjust the dosage and interval time of medication.
(3) If the patient’s degree of coma deepens, tendon reflexes and muscle tension gradually decrease, and there is a contralateral pyramidal tract sign or a tonic response to the brain, it is a sign that the lesion is enlarged or the midline structure shifts aggravated. In addition to intravenous infusion of 250 ml of 20% mannitol for active dehydration treatment, 40 mg of furosemide should be added, and 10-20 mg of dexamethasone can be added intravenously in a short period of time, 1-2 per day Second, the above two drugs can be applied simultaneously or alternately.
(4) Patients with mild clinical symptoms, clear consciousness, no severe headache, vomiting, and no papilledema on fundus examination, especially those with lacunar cerebral infarction or small focal cerebral infarction may not need dehydrating agent temporarily.
(5) Dehydrating agent is generally used for 5-7 days. However, if it is combined with lung infection or frequent seizures, the cerebral edema is often aggravated due to infection, poisoning, hypoxia and other factors, and the application time of dehydrating agent can be appropriately extended.
In the process of applying dehydrating agents, it is necessary to pay attention to whether the purpose of dehydration has been achieved, but also to prevent adverse reactions caused by excessive dehydration, such as insufficient blood volume, hypotension, electrolyte imbalance and renal damage.
3. Summary
(1) Timing of medication It is not recommended to use mannitol for the prevention of cerebral edema.
There is no unified view on the timing of the use of mannitol, and a large-scale prospective study is still needed. The editor reviewed the Eighth Edition of Internal Medicine and the 14th Edition of Practical Internal Medicine and said, “Mannitol is the first choice for dehydration to reduce intracranial pressure, but attention should be paid to the prevention and treatment of adverse reactions, especially when it is used for a long time. Deal with such as hypovolemia, hyperosmotic state, electrolyte disturbance, renal function and cardiac function damage.
A retrospective analysis by Helbok et al. in 2011 showed that mannitol can effectively reduce the intracranial pressure in patients with severe cerebral hemorrhage and benefit brain metabolism. “There is no mention of the application of mannitol in active bleeding.
With the widespread use of CT and MRI, a higher proportion of patients find that hematomas have significantly enlarged. The enlargement of the hematoma is at least related to factors such as the degree of increased blood pressure, coagulation function, bleeding site, and hematoma morphology. According to the results of Wen Bingtao et al. “The Effect of Mannitol on Early Hematoma Expansion of Cerebral Hemorrhage”, the results show that: Early use of mannitol can increase the incidence of early expansion of cerebral hemorrhage in dogs; early onset of cerebral hemorrhage, especially within 24 hours, should not be blindly used mannitol , So as not to induce hematoma enlargement and aggravate the condition.
Once active bleeding is suspected, mannitol should be used with great caution. Because mannitol dehydrates tissues other than the hematoma, it can rapidly increase the pressure gradient between the hematoma and the brain tissue, thereby promoting the expansion of the hematoma or aggravating active bleeding, leading to worsening of clinical symptoms.
Some people suggest that patients with cerebral hemorrhage should take active measures after the first CT examination to maintain the patient’s vital signs, closely observe the changes in the condition, and review the CT 24 to 48 hours later. If the condition and the size of the hematoma are stable, osmotic drugs such as mannitol can be used to help reduce brain edema. At present, there is no unified view on the timing of the use of mannitol, and a large-scale prospective study is still needed. We believe that the timing of the application of mannitol in patients with cerebral hemorrhage should consider the patient’s condition and the size and location of the hematoma, and pay attention to individualization.
(2) The drip rate problem
The faster the drip rate, the higher the plasma osmotic pressure, the stronger the dehydration effect, and the better the curative effect. However, pay attention to the underlying disease of the patient. In patients with cardiac insufficiency, coronary heart disease, and renal insufficiency, the rapid drip rate may lead to fatal diseases. A transient increase in blood volume may cause acute cardiac insufficiency; too much diuresis can lead to insufficient effective blood volume, increase blood viscosity, and cause acute myocardial infarction and cerebral infarction. Too fast drip rate may have a damaging effect on kidney function. It is generally required to finish dripping within 20 minutes. It depends on the different conditions of each patient.
(3) Dosage issues
Mannitol has been used clinically as a drug for lowering intracranial pressure for a long time, but its dosage is still controversial. At present, there are several opinions:
①The use of mannitol advocates a large dose of 1.0 g/kg.
Wise et al. once believed that a large dose of 1.0 g/kg was an effective dose, and the effective time was 4 to 6 hours. Experiments with dogs, by monitoring intracranial pressure, found that the best dose of mannitol for lowering intracranial pressure is also 1.0 g/kg, but the effective time is 90 to 120 minutes. They believe that for patients with severe intracranial pressure increase, if the intracranial pressure needs to be quickly and effectively reduced, the mannitol dose should be 1.0 g/kg, and the medication should be repeated within 120 minutes. However, some people believe that the maximum dose of mannitol can only reach 1 g/kg every 6 hours. There is no need to increase the dose or shorten the interval between medications. Exceeding this dose cannot increase dehydration, but only increase side effects.
② Some people advocate the use of low-dose mannitol (0.2-0.5g/kg).
It is believed that the effect of low-dose mannitol in reducing intracranial pressure is similar to that of high-dose, and can avoid severe dehydration, osmotic imbalance, and extravasation of mannitol in high-dose.
Clinical observations have found that the use of 0.5 g/kg of low-dose mannitol in the treatment of acute cerebrovascular disease has a curative effect similar to that of high-dose, and no toxic side effects occur. The first dose of mannitol is 0.75 g/kg, and 0.25 g/kg every 2 hours thereafter or until the plasma osmotic pressure exceeds 310 mOsm/L. This regular and frequent use of mannitol results in a relatively stable change in intracranial pressure. At present, most scholars believe that patients with acute cerebrovascular disease often have damage to the heart and kidney function, and large doses of mannitol can constrict the renal blood vessels and increase the burden on the heart and kidney. Low-dose mannitol expands volume, diuresis, dilates renal blood vessels, and has a protective effect on the kidneys, and low-dose mannitol has a similar effect on lowering intracranial pressure as high-dose. Therefore, low-dose mannitol is safe and effective in the treatment of acute cerebrovascular diseases.
③The effect of dehydration on lowering intracranial pressure is small when the dosage is small, and the side effects of large dosage and rapid drip rate increase correspondingly.
It should be taken seriously according to the specific situation of the patient. For small focal bleeding, use 20% mannitol 125~150ml for rapid intravenous infusion, 2 times a day or q8h. Larger hemorrhage or severe ischemic brain edema can be used up to 125-250mlq4-8h.
And to consider its underlying diseases. People with heart failure, coronary heart disease, and renal failure should be used with caution. And add furosemide or/and albumin appropriately according to different situations. If the patient has a significant heart, furosemide should be preferred for kidney disease.
Some animal experiments have shown that 125ml and 250ml have no significant difference in dehydration effect, but there are also experiments that show that the dehydration effect of larger doses has a certain degree of increase, and there is a dose-effect relationship. The best can make the patient’s plasma osmotic pressure between 300-320mOsm/L.
(4) How long to use
Generally 7±3 days, some severe cases 14±3 days
(5) Rebound mechanism and preventive measures of mannitol
The half-life of mannitol is (1.23±0.22)h, and the volume of distribution (Vd) is 426.79 ml. The pharmacokinetic properties of mannitol show rapid elimination in the body and the distribution is not very extensive. Cai Minghong and other studies have shown that the excretion of mannitol in CSF is slower than the excretion of mannitol in serum. Mannitol can penetrate the blood-brain barrier and stay in CSF. When the concentration of blood mannitol decreases, the mannitol in CSF remains Maintain a higher concentration to form a new osmotic gradient, which causes a rebound in brain pressure.
The rebound time is more than 1 hour after administration. Further research found that the high-dose group (760 mg/kg) had different degrees of rebound after 1 to 1.5 hours of medication. The mannitol concentration in the cerebrospinal fluid was measured (0.91±0.64) mmol/L; while the low-dose group (400mg/kg) kg) had no rebound phenomenon, the concentration of mannitol in the cerebrospinal fluid was lower (0.65±0.53) mmol/L, and the percentage of cerebral pressure drop was better than that of the high-dose group.
In patients with intracranial hypertension, when intravenously injecting mannitol to lower cerebral blood pressure, the dosage should be 400 mg/kg, and the infusion rate should not exceed 50 mg/(kg•min). This can achieve the best effect of lowering blood pressure and prevent brain pressure from rebounding. .
4. What should be paid attention to in nursing?
Question 1: What are the requirements for mannitol intravenous infusion?
1. During intravenous infusion, nurses must patrol and closely observe the infusion speed and changes in the condition; critically ill patients or those who require pressure infusion must be closely monitored, and abnormal conditions should be reported to the doctor in time.
2. Due to the fast dripping rate of mannitol, it is easy to stimulate local pain. In severe cases, it may cause phlebitis, causing the vein to become hard and occluded. Change the injection vein site or replace the indwelling needle according to the situation.
3. Mannitol tends to crystallize when cold, so it should be checked carefully before application. Mannitol must be used without crystals. If there is crystals, it must be dissolved before use; if crystals appear during intravenous infusion, the infusion should be stopped in time and the drug should be replaced.
Question 2: How to protect blood vessels during intravenous infusion of mannitol?
1. The clinical use rate of mannitol is relatively high. The application of intravenous indwelling needle, central venous puncture, PICC puncture, greatly reduces the vascular puncture injury.
2. Choose a thicker blood vessel, the blood flow is faster, and reduce the incidence of phlebitis.
3. During medication, a thin foam dressing can be applied to the puncture site, and hot compress after removal of the needle; during infusion, 50% safflower alcohol gauze can also be placed on the skin of the upper end of the needle to prevent phlebitis.
4. Once the symptoms of phlebitis such as pain and redness in the injection vein occur, promptly adopt methods such as alcohol wet compress and mannitol warming input to control the symptoms of phlebitis; change the site for venipuncture if necessary.
Question 3: How to deal with mannitol extravasation?
Once leakage occurs, immediately take measures such as 0.01% phentolamine solution soaked gauze wet compress, scald ointment external application, etc., which can improve microcirculation, eliminate edema, and prevent tissue necrosis.
If the extravasation is accompanied by local congestion, local injection of procaine can be used to reduce the fragility of local blood vessels, thereby reducing or preventing fluid extravasation and pain response, alleviating vasospasm, improving ischemic hypoxia, and facilitating exudation The absorption of substances can reduce local damage; if it is not handled in time, it will not recover for more than 24 hours.
For ischemia that has occurred, hot compresses are strictly prohibited, because hot compresses can increase the temperature of local tissues, accelerate metabolism, increase oxygen consumption, and aggravate tissue necrosis.
Question 4: The doctor orders to lower intracranial pressure and requires rapid infusion of mannitol. What should I do if the heart and kidney function is poor during rapid intravenous infusion?
The faster the mannitol drip rate, the higher the plasma osmotic pressure, the stronger the dehydration effect, the better the curative effect. Mannitol is generally required to be dripped within 20 minutes, but in clinical application, the nurse still has to decide according to the different conditions of each patient.
Pay attention to the underlying diseases of the patient. For patients with cardiac insufficiency, coronary heart disease, and renal insufficiency, too fast drip rate may lead to fatal diseases, transient increase in blood volume may cause acute cardiac insufficiency, and excessive diuresis may cause Insufficient effective blood volume can cause blood viscosity to increase, which can cause acute myocardial infarction and cerebral infarction. Too fast drip rate can also damage kidney function.
When mannitol is used for the treatment of drugs and poisons, it is infused intravenously at a conventional rate.
When used for the treatment of cerebral edema, intracranial hypertension and glaucoma, it is required to be applied to the patient in a relatively short time. The clinical speed can be increased by “pressurized infusion”, which is generally 0.25-2 g/kg according to the body weight, and the preparation is 15 %~25% concentration intravenously in 30~60 min.
However, when the patient’s heart and kidney function is poor, the dose should be reduced, and the kidney function should be closely followed up. It should be used with caution or not for those who have had heart failure or heart failure.
Question 5: The specification of mannitol is 250ml/bottle, but doctors usually use 100-125ml. How can the clinic ensure the accuracy of the dosage?
1. You can let go of half in advance;
2. Use a mark on the corresponding horizontal position of the infusion bottle (draw with a marker). When the input reaches this horizontal line, pay attention to changing the liquid (remember: remind family members to help watch).
Supplement: Is it necessary to record the amount of intravenous mannitol in the 24-hour intake?
The clinical conclusion is still inconclusive. The nurse should record the medication, but the specific amount is not counted, and should communicate with the doctor in advance to reach a consensus on the information.
Question 6: In order to ensure safe medication, what are the adverse reactions of mannitol that nurses need to know about?
Excessive dosage, high concentration, and long time of mannitol can degenerate and block the renal tubules, resulting in oliguria or azotemia;
Experiments have proved that kidney damage can be seen within 96 hours of intravenous injection of mannitol, and a large amount of rapid intravenous drip can cause osmotic nephropathy (also known as mannitol nephropathy);
Mannitol can also enter the blood-brain barrier destruction area, aggravating local cerebral edema;
Large doses, long-term use or plasma osmolality exceeding 320 mmol/L can cause electrolyte disturbances, renal failure, acidosis, etc.
Question 7: Can dexamethasone be added to mannitol?
There is a taboo between the two.
The “Guidelines for the Preparation and Use of Clinical Intravenous Drugs” also pointed out: “Mannitol injection is a supersaturated solution and should be instilled separately. If electrolytes such as potassium chloride and dexamethasone are added, mannitol will be salted out and crystallized.
Dexamethasone is a sodium salt of phosphate injection, containing 0.2% sodium sulfite, mixed with supersaturated 20% mannitol injection to cause salting out reaction of mannitol.
-THE END-
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



