Harvard University research: Overeating is not the main cause of obesity
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Harvard University research: Overeating is not the main cause of obesity
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Harvard University research: Overeating is not the main cause of obesity.
Subverting a century-old classic theory, Harvard University research points out: overeating is not the main cause of obesity.
With economic development and improvement of living standards, obesity has become a major public health problem worldwide. According to the World Health Organization (WHO) , nearly 2 billion people are overweight or obese in the world.
From 1975 to 2016, the global obesity rate has nearly tripled, and the number of deaths caused by overweight or obesity is as high as 2.8 million each year .
In fact, obese people are not only inconvenient to live and have reduced exercise capacity, but also are more prone to metabolic diseases and cardiovascular and cerebrovascular diseases.
Numerous studies have shown that obesity is associated with increased risk and reduced prognosis and survival for more than a dozen cancers .
In response to the growing obesity epidemic, the USDA’s 2020-2025 Dietary Guidelines tell us that weight loss requires adults to reduce the calories they get from food and drink and increase the calories they burn through physical activity.
This approach to weight management is based on the century-old ” energy balance model ,” which states that weight gain is due to more energy being ingested than expended. In today’s world, surrounded by delicious, mass-market, inexpensive processed foods, it’s easy to consume far more calories than you actually need.
Today ‘s sedentary lifestyle further exacerbates this imbalance.
According to this model, overeating, combined with insufficient physical activity, is driving the obesity epidemic.
Despite decades of public health messages advising people to eat less and exercise more, the incidence of obesity and obesity-related diseases has been steadily rising.
However, the ” energy balance model ” that treats obesity as an energy balance disorder reiterates the principles of physics without considering the biological mechanisms of weight gain.
Recently, an expert team of 17 internationally recognized scientists, clinical researchers and public health experts from Harvard Medical School, Weill Cornell Medical College, University of Copenhagen, National Institutes of Health and other institutions published in The American Journal of The journal Clinical Nutrition published an article titled: The carbohydrate-insulin model: a physiological perspective on the obesity pandemic .
The study supports the ” carbohydrate-insulin model ,” which argues that obesity is a metabolic disorder that has more to do with ” what you eat ” than ” how much you eat .” This also explains why many people eat less and exercise more but fail to lose weight.
The ” carbohydrate-insulin model ” makes a bold claim: Overeating doesn’t lead to obesity ; the process of getting fat leads to overeating . The current obesity epidemic is due to hormonal responses to changes in food quality: especially foods with a high glycemic load, they fundamentally alter our metabolism.
Overall, the authors point out fundamental flaws in the ” energy balance model , ” arguing that the ” carbohydrate-insulin model ” can better explain obesity and weight gain , and point the way to more effective, longer-lasting weight management strategies : More attention should be paid to what to eat rather than how much .

The study’s leader, Dr. David Ludwig , an endocrinologist at Boston Children’s Hospital and a professor at Harvard Medical School , explains why the ” energy balance model ” doesn’t help us understand the biology of weight gain: For example, during a growth spurt in adolescence, It might be possible to eat 1000 calories a day, but is it the overeating that causes the growth spurt, or is the growth spurt causing starvation and overeating?

Professor David Ludwig
Contrary to the ” energy balance model ” , the ” carbohydrate-insulin model ” , which boldly claims that overeating is not a major cause of obesity , blames the current obesity epidemic on modern dietary patterns characterized by excessive consumption of high glycemic loads foods : especially processed, rapidly digested carbohydrates.
These foods trigger a hormonal response that fundamentally alters our metabolism, leading to fat storage, weight gain, and obesity.
When we eat highly processed carbohydrates, the body increases insulin secretion and suppresses glucagon secretion.
This, in turn, signals fat cells to store more calories, reducing the energy expenditure available to fuel muscles and other metabolically active tissues. The brain thinks that the body is not getting enough energy, which in turn causes hunger.
In addition, metabolism may slow down as the body tries to conserve energy expenditure. Therefore, we tend to stay hungry even as we continue to gain excess fat.
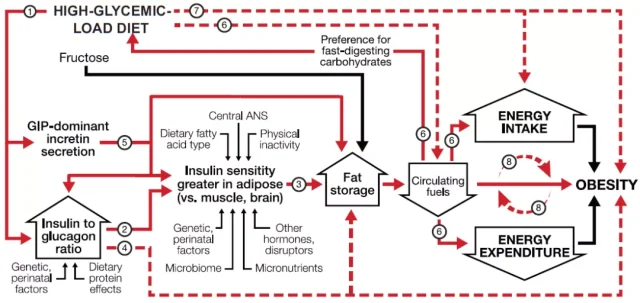
Carbohydrate-Insulin Model
Therefore, to understand the obesity epidemic, it is necessary to consider not only how much food we eat, but also how the type of food we eat affects our hormones and metabolism.
The ” energy balance model ” asserts that all calories from food are similar to the body, which misses a key piece of the puzzle.
In fact, the ” carbohydrate-insulin model ” is not a newly proposed model, it dates back to the 1900s, but this paper by Harvard Medical School, Weill Cornell Medical College, University of Copenhagen, National Institutes of Health The opinion piece published by a team of 17 internationally recognized scientists, clinical researchers and public health experts from the Institute and other institutions is the most comprehensive expression of the “carbohydrate-insulin model” to date .
Overall, this article summarizes the growing body of evidence supporting the ” carbohydrate-insulin model . ” In addition, the authors identify a set of testable hypotheses to differentiate the two models to guide future research.
Adopting a ” carbohydrate-insulin model ” rather than an ” energy balance model ” has fundamental implications for weight management and obesity treatment. Rather than urging people to eat less, the “carbohydrate-insulin model” suggests another pathway that’s more focused on what we actually eat. Reducing the consumption of rapidly digestible carbohydrates that are now flooding the food supply reduces the body’s underlying drive to store fat. This way we can lose weight with less hunger and struggle .
Finally, the authors also point out that further research is needed to finally test both models, which would also lead to new models that are more accurate.
To this end, they call for constructive discussions and collaboration with scientists with different viewpoints to test the predictions of the carbohydrate-insulin model in rigorous and impartial research .
Reference:
https://doi.org/10.1093/ajcn/nqab270
Harvard University research: overeating is not the main cause of obesity
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



