Vaccination of pregnant women significantly reduces the risk of neonatal COVID-19 hospitalization
- Why Botulinum Toxin Reigns as One of the Deadliest Poisons?
- FDA Approves Pfizer’s One-Time Gene Therapy for Hemophilia B: $3.5 Million per Dose
- Aspirin: Study Finds Greater Benefits for These Colorectal Cancer Patients
- Cancer Can Occur Without Genetic Mutations?
- Statins Lower Blood Lipids: How Long is a Course?
- Warning: Smartwatch Blood Sugar Measurement Deemed Dangerous
Vaccination of pregnant women significantly reduces the risk of neonatal COVID-19 hospitalization
- Red Yeast Rice Scare Grips Japan: Over 114 Hospitalized and 5 Deaths
- Long COVID Brain Fog: Blood-Brain Barrier Damage and Persistent Inflammation
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Evidence: Vaccination of pregnant women significantly reduces the risk of neonatal COVID-19 hospitalization
When discussing high-risk groups for COVID-19, the general focus is on the elderly , immunosuppressed , or people with multiple underlying medical conditions .
They are of course a high-risk group. For example, most of the people who are still hospitalized with the COVID-19 after vaccination are the elderly, and the proportion of immunosuppressed people is also much higher than the proportion of this group in the population.
But another group of people is also very important – pregnant women. From a physiological point of view, pregnant women can be regarded as people with underlying diseases, and they belong to a high-risk group after contracting the COVID-19.
Real-world data also confirms this. In a Scottish study [1], 19.5% of unvaccinated pregnant women required hospitalization and 2.7% required ICU admission after infection with the COVID-19 .
COVID-19 infection is extremely dangerous not only for the pregnant woman herself, but also for the fetus.
In the same study, the perinatal mortality rate of fetuses infected with the COVID-19 reached 22.6 cases per 1,000 births, nearly four times the background value of 5.6 cases .
Getting vaccinated can substantially reduce these risks. Taking the Scottish study as an example, after two doses of the vaccine, the proportion of pregnant women who were hospitalized after contracting the COVID-19 dropped to 5.1% , and even just one dose of the vaccine could reduce the hospitalization rate to 8.3%.
The ICU risk was reduced to 0.2%. All of the premature deaths in the study also occurred in the unvaccinated population.
Sadly, vaccination rates for pregnant women lag significantly behind the general population . When the average Scottish female two-shot vaccination rate reached 77.4%, the pregnant woman’s vaccination rate was only 32.3%
In addition to the obvious protective effect on the pregnant woman herself, scientists have previously speculated that after the pregnant woman is vaccinated, it may also transfer antibodies through the placenta, so that the fetus can obtain certain protection after birth by passive immunization.
This protection has been exemplified in many past disease studies.
In principle, the transport of substances between the mother and the fetus is carried out through the placenta – there is a strict “selection” of what substances can pass through the placenta, and the most important type of antibody – IgG can enter the fetus through the placenta.
The half-life of IgG antibodies is relatively long, and even after birth, passively infused antibodies during pregnancy can bring certain protection to the newborn.
Specific to the COVID-19, some previous studies have confirmed that after the mRNA COVID-19 vaccine is vaccinated, the specific IgG antibodies against the COVID-19 virus in the pregnant woman can enter the fetus through the placenta, and the COVID-19 from the mother can be Antibodies [2] [3].
Combining the results of other studies, such as the COVID-19 vaccine with higher antibody titer in clinical trials is more effective, and the input of a large number of neutralizing antibodies in animal models can also provide protection, etc., we can speculate that antibodies alone can also provide some protection.
On this basis, it can also be further speculated that the COVID-19-specific antibodies transferred from the placenta may provide protection for the newborn after leaving the mother .
But this is just speculation, and there is uncertainty with a lack of empirical evidence.
For example, we do not know whether the amount of antibodies transferred from the placenta is high enough to have a substantial protective effect.
For another example, how long can these antibodies from the mother survive, even if they have a protective effect, how long can they last.
On February 15, the results of a CDC study showed that after vaccination during pregnancy, the risk of neonatal hospitalization due to COVID-19s in the first six months of life was significantly reduced .
Confirmed with real efficacy data: antibodies from the mother can provide effective passive immune protection for newborns, providing more evidence for the benefits of vaccination for pregnant women.
The researchers collected 379 neonatal cases (aged less than 6 months) hospitalized with COVID-19 from July 2021 to early January 2022 (Delta-dominant period), and 203 hospitalized cases without COVID-19 infection.
Comparing the vaccination status of newborn mothers – the effect of only two doses of the mRNA vaccine was analyzed in the study, and it was found that the risk of neonatal COVID-19 hospitalization decreased by 61% after vaccination during pregnancy (61% effective in preventing hospitalization) :
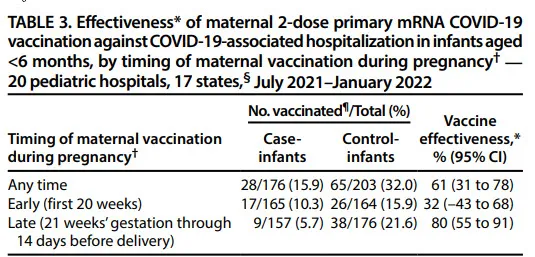
A 61% reduction in the risk of neonatal hospitalization is an extremely important outcome.
We have some misconceptions about the risk of Covid-19 in children. We often hear that minors or children are a low-risk group of COVID-19s, and even if they are infected, they are not at great risk.
There are two misunderstandings here. One is that compared with high-risk groups such as the elderly, the overall risk of severe illness for minors is lower.
But under a very large infection base, the number of children who end up in severe illness, hospitalization or even death is not a lot – this is the case with the data in the United States.
Second, the minors themselves are a very different group. Infants aged 0-4 and teenagers aged 15-17 are very physically different, and reflected in the COVID-19, the risks of severe illness are also different.
Since the outbreak of Omicron, the CDC’s tracking has shown that children under the age of 4 have begun to surge in COVID-19 hospitalizations , and the risk is close to that of ordinary adults and much higher than that of children and adolescents:
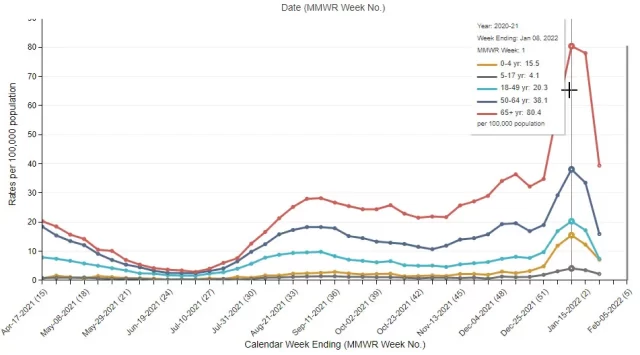
In this study of the protective effects of vaccination during pregnancy, about 25% of newborns hospitalized with COVID-19 were admitted to the ICU. Of the 176 cases for which disease data were available, 1 was severe enough to require ECMO, and 1 unfortunate death, all from the unvaccinated group of mothers.
Of course, this study only analyzed two mRNA vaccines. In theory, the amount of antibodies transported by the placenta correlates with the amount of antibodies in the mother.
mRNA vaccines are currently the type with the most antibody formation in the COVID-19 vaccine, so other vaccines may not be able to replicate the results of this study.
At the same time, the protective effect of vaccination in early pregnancy on neonates seems to be lower, which may be due to the fact that the passage of antibodies through the placenta into the fetus mainly occurs in the third trimester, and the antibody in the mother has declined by this time after the early vaccination.
However, this does not mean that pregnant women do not need to be vaccinated or postponed until the third trimester .
The protection of newborns by vaccination during pregnancy can only be said to be an extra blessing, and the most critical benefit is the protection of pregnant women themselves .
Vaccination greatly reduces the risk of hospitalization for pregnant women, and also reduces the risk of premature birth, which is the most important and critical benefit—and the best protection for children.
After all, when pregnant women are admitted to the ICU due to COVID-19 infection, the risk of COVID-19 hospitalization for newborns is really a bit remote.
Reference:
https://www.nature.com/articles/s41591-021-01666-2
https://www.jci.org/articles/view/150319
https://www.sciencedirect.com/science/article/pii/S2589933321001877?via%3Dihub
Vaccination of pregnant women significantly reduces the risk of neonatal COVID-19 hospitalization
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



