Why can mushrooms with hallucinogenic effects treat depression?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Why can mushrooms with hallucinogenic effects treat depression?
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Why can mushrooms with hallucinogenic effects treat depression?
On April 11, 2022, Richard E. Daws, a researcher at Imperial College London, published a research paper titled “Increased global integration in the brain after psilocybin therapy for depression” in the top international medical journal Nature Medicine.
Psilocybin, also known as psilocybin, is a neurotoxin with hallucinogenic effects. In the clinical trial described in this article, psilocybin showed antidepressant potential compared with the escitalopram-administered group [1] .

Depression affects the health of nearly 16% of the world’s population [2] , and social events caused by patients with major depressive disorder (MDD) indirectly arouse public attention to depression.
However, the underlying pathological mechanism of this disease has not been elucidated.
Major symptoms of MDD include low mood(decreased inner drive or feeling hopeless), anhedonia(reduced ability to experience pleasurable activities such as eating, sex, and social interactions), fatigue, irritability, poor concentration, poor sleep quality, decreased appetite, cognitive decline, and suicide.
Not only is depression often accompanied by anxiety disorders, but it is also strongly associated with dementia, type 2 diabetes, coronary artery disease, Parkinson’s disease, epilepsy, pain, and cancer. Unfortunately, the chronic effects of depression complicate the prognosis of many chronic diseases to the detriment of the world’s public health.
Therefore, we urgently need to find effective antidepressant drugs to improve this problem. psilocybin(see picture 1)Derived from a family of mushrooms known as “magic mushrooms,” which have been used in historical records to induce hallucinations.
However, some recent studies have shown that it is promising for the treatment of MDD, obsessive-compulsive disorder and tobacco addiction [3] .

Figure 1 Chemical structure of psilocybin
Two-group clinical trial of psilocybin in the treatment of depression
The first open-label, open-label clinical trial recruited 19 patients with treatment-resistant depression (TRD) , and 16 patients (mean age 42.75 years, 4 of whom were women) were finally included in the statistics , Clinical assessment was performed using the Beck Depression Inventory (BDI) .
After follow-up treatment, the imaging results demonstrated the antidepressant effect of psilocybin for the first time, and it has the characteristics of rapid treatment .
The BDI scale can obtain relevant information about the cognitive ability of patients with depression, and this cognitive ability change may be an important indicator of psilocybin antidepressant treatment.
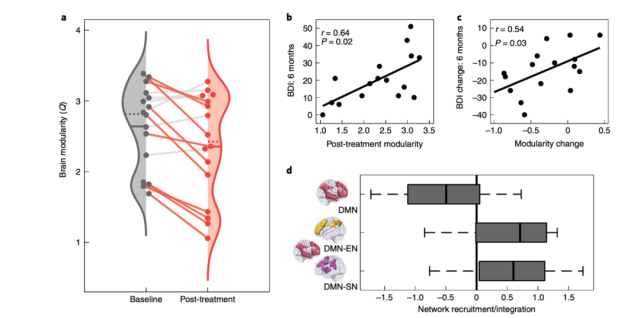
One day after psilocybin administration, brain modularity was reduced in TRD patients (see Figure 2a) ; implying an increase in overall network functional connectivity within the brain.
And through the Pearson correlation test, it showed that the long-term improvement of depressive symptoms was significantly correlated with the reduction of brain modularity (see Figure 2b,c) .
Decreased Default Model Network (DMN) means increased connectivity between the brain and cognitive-related networks such as Executive Network (EN) and Salience Network (SN) (see Fig. 2d) .
Figure 2 Results of the first open-label single-arm clinical trial
- a. Brain modular changes at each sample point before and after administration
- b. After administration, modularity was positively correlated with BDI scale scores
- c. Modular changes were positively correlated with BDI scale scores
- d. DMN values decreased, DMN and EN , SN connectivity increases
The second double-blind, randomized, controlled, safety-validated clinical trial recruited 59 patients with MDD, and 22 patients were finally included in the psilocybin administration group; 21 patients were included in microcrystalline cellulose (a type of Pharmaceutical excipients) capsules of placebo, or the traditional antidepressant escitalopram administration of the control group.
The results showed that brain modularity was reduced after 1 day of psilocybin administration, but not significantly after escitalopram administration, confirming the authors’ main hypothesis (see Figure 3a, Figure 3d) .
During brain scans using functional magnetic resonance imaging (fMRI) , “dynamic flexibility” is a measure of how frequently brain regions change their connections over time. Decreased “dynamic flexibility” is associated with symptoms of depression.
Also, there is a correlation between changes in brain module networks after psilocybin treatment and BDI scores(see Figure 2b); Changes in the EN region, with strong correlations with other frontal networks(see Figure 3c). However, there was no significant correlation in the escitalopram-administered group.
 a. The brain modularity of each sample point changed significantly before and after psilocybin administration. b. After psilocybin administration, the modularity was positively correlated with the BDI scale score c. The correlation between EN and other brain regions was significant d. There was no significant change in the brain modularity of each sample point before and after escitalopram administration e. There was no correlation between the modularity and BDI scale score after escitalopram administration f. The correlation of each brain area after administration Not obvious
a. The brain modularity of each sample point changed significantly before and after psilocybin administration. b. After psilocybin administration, the modularity was positively correlated with the BDI scale score c. The correlation between EN and other brain regions was significant d. There was no significant change in the brain modularity of each sample point before and after escitalopram administration e. There was no correlation between the modularity and BDI scale score after escitalopram administration f. The correlation of each brain area after administration Not obvious
Figure 3 Results of the second double-blind controlled clinical trial
The results of previous studies have shown that functional connectivity (FC) in depression is usually in a reduced state; increased DMN activity means decreased functional connectivity, which is associated with rumination symptoms in patients with depression [4,5] .
Depressed patients will keep thinking about the same problem over and over again, immersed in negative and unsolved problems, and generate a lot of negative emotions.
In conclusion, the acute effects of the hallucinogen psilocybin on brain activity showed benign changes in overall brain function, increased connectivity across brain regions, and reproducible changes.
Antidepressant Mechanism and Prospect of Clinical Evaluation
Serotonin is an important neuromodulatory transmitter with a unique ability to shape synapses.
Synapse formation is a well-known key mechanism for learning and memory, and synaptic dysfunction caused by neuronal atrophy and cell death is the pathological basis of depression [6] .
Antidepressant drugs commonly used in clinical practice, Selective Serotonin Reuptake Inhibitor (SSRI) drugs, indirectly increase the concentration of serotonin in the synaptic cleft by selectively inhibiting the recovery of serotonin. Activates the ability of serotonin to promote synaptic development.
These drugs are highly selective for serotonin and have little effect on adrenergic, dopamine, histamine and cholinergic nerves, and are suitable for various types of depression.
Treatment with psilocybin appears to increase the brain’s ability to interconnect higher-order functional areas. The effect of psilocybin to open up the “Ren and Du two meridians” is consistent with the “emotional release” of patients’ subjective feedback.
This enhanced “emotional release” effect may be unique to psilocybin therapy compared to SSRIs. The effects of psilocybin on cerebral cortical activity appear to be induced by direct stimulation of serotonin receptors in the cerebral cortex.
Cerebral Blood Flow (CBF) and Blood Oxygen-Level Dependent (BOLD) Resting-State Functional Connectivity ( Resting- State Functional Connectivity, RSFC) to detect changes in DMN and assess the degree of improvement in depressive symptoms [7] , see Figure 4.
 Figure 4 CBF imaging results
Figure 4 CBF imaging results
While this finding is encouraging, the current trials of psilocybin for depression are conducted in controlled clinical settings, with tightly controlled doses and doses of There are mental health experts to provide complete psychological counseling services.
Therefore, people with depression should not try psilocybin for treatment on their own. Taking hallucinogenic mushrooms or psilocybin privately without careful clinical trial safeguards will not have a positive effect on disease.
In conclusion, depression is a major public health problem, which brings huge burden and cost to society. Using the imaging method fMRI, the researchers proposed a potential index to assess the changes in depression, reflecting the changes in depression treated with psilocybin.
This result may help explain why psilocybin therapy holds promise as a new option for depression treatment.
References
[1] Daws RE, Timmermann C, Giribaldi B,, et al. Increased global integration in the brain after psilocybin therapy for depression [J]. Nat Med, 2022.
[2] Yang L, Zhao Y, Wang Y, et al. The Effects of Psychological Stress on Depression [J]. Curr Neuropharmacol, 2015, 13(4): 494-504.
[3] Geiger HA, Wurst MG, Daniels R N. DARK Classics in Chemical Neuroscience: Psilocybin [J]. ACS Chem Neurosci, 2018, 9(10): 2438-47.
[4] Hamilton JP, Furman DJ, Chang C, et al. Default-mode and task-positive network activity in major depressive disorder: implications for adaptive and maladaptive rumination [J]. Biol Psychiatry, 2011, 70(4): 327 -33.
[5] Feurer C, Jimmy J, Chang F, et al. Resting state functional connectivity correlates of rumination and worry in internalizing psychopathologies [J]. Depress Anxiety, 2021, 38(5): 488-97.
[6] Kraus C, Castrén E, Kasper S, et al. Serotonin and neuroplasticity – Links between molecular, functional and structural pathophysiology in depression [J]. Neurosci Biobehav Rev, 2017, 77: 317-26.
[7] Carhart-Harris RL, Roseman L, Bolstridge M, et al. Psilocybin for treatment-resistant depression: fMRI-measured brain mechanisms [J]. Sci Rep, 2017, 7(1): 13187.
Why can mushrooms with hallucinogenic effects treat depression?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.