First time: Study found elevated deformability of immune cells in people with depression
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
First time: Study found elevated deformability of immune cells in people with depression
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
First time: Study found elevated deformability of immune cells in people with depression.
Scientists evaluate the deformability of blood cells in patients with depression for the first time and find that the deformability of immune cells increases, affecting cell function.
Depression is mainly manifested by symptoms such as low mood, decreased interest, slow thinking, poor diet and sleep. According to the World Health Organization (WHO), more than 350 million people worldwide suffer from depression, which has become the fourth largest disease in the world, and the number of patients is still growing rapidly [1].
Depression is also associated with increased rates of cardiovascular disease, diabetes and Alzheimer’s disease .
More notably, more than 700,000 people commit suicide every year because of depression. However, the current social awareness of depression is far from enough.
There are also many people who equate depression with the negative emotions that come with being frustrated in life, unaware that it is a serious illness.
In addition, many people with depression delay their illness because they are not properly diagnosed.
Recently, researchers from the research group of Andreas Walther of the Technical University of Dresden in Germany published important research results in the journal Translational Psychiatry [2].
Depressed patients, especially those with persistent depressive disorder (PDD), have more deformable peripheral blood cells than healthy people.
Among them, lymphocytes, monocytes and neutrophils are the immune cells most affected by depression .
For the first time, the study found elevated deformability of immune cells in people with depression .
This change in the mechanical characteristics of immune cells suggests that depression is related to a sustained immune response in the body.
Precisely regulating the deformability of immune cells in patients with depression may be a new idea for the treatment of depression in the future .

The pathophysiological mechanisms of depression have not been elucidated until today.
Hyperactivation of the hypothalamus-pituitary-adrenal axis (HPA) and chronic low-grade inflammation are currently the two most recognized pathophysiological features associated with depression [3].
Many studies have found elevated levels of cortisol and pro-inflammatory cytokines in patients with depression, suggesting that depression is associated with activation of the immune system.
Studies in recent years have also confirmed that in the peripheral blood of patients with depression, various types of immune cells are significantly increased [4].
The activation of the immune system is not only reflected in the number of cells, but also reflected in the abnormal function of immune cells.
However, there is no direct evidence that patients with depression have abnormal immune cell function .
Inside the cell, there is an extremely complex network of protein fibers called the cytoskeleton.
The cytoskeleton gives cells the ability to actively deform and resist passive deformation, known as cell deformability.
Cell deformability is closely related to cell function and can be used as a good indicator to reflect cell function .
Andreas Walther’s team recruited 220 participants (18-68 years old) from the Dresden Burnout Study (DBS) cohort.
Groups were grouped by initial assessment of depression risk using the Patient Health Questionnaire (PHQ-9).
Subsequently, the researchers further refined the DIA-X-5 Composite International Diagnostic Interview to assess the type of depressive disorder.
Finally, the researchers took a 20 μl blood sample from the fingertips of the participants, and tested the deformability of blood cells with the help of a real-time cell deformability counter (RT-DC) (see Figure 1) to obtain the cell size and deformation rate of each cell type. .
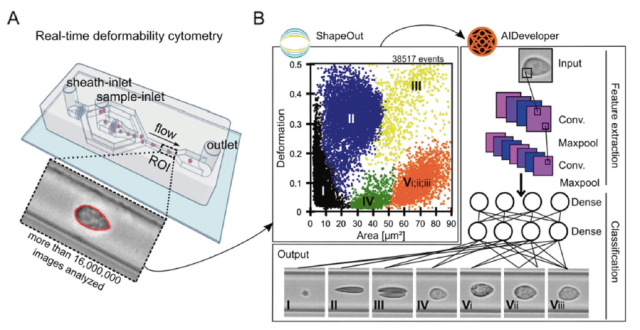 Figure 1. Schematic illustration of the real-time cell deformability counter and subsequent artificial intelligence-based hemocyte fractionation method.
Figure 1. Schematic illustration of the real-time cell deformability counter and subsequent artificial intelligence-based hemocyte fractionation method.
After excluding participants who did not cooperate or combined with mania, the enrollment was as follows: the case group (those with a PHQ-9 score > 10 points) a total of 69 cases; the control group (those with an age-sex-matched PHQ-9 score < 5 points) A total of 70 cases.
After further evaluation of the type of depressive disorder, the final enrollment results were: a total of 30 patients with lifelong persistent depressive disorder (LTPDD), a total of 15 patients with 1-year persistent depressive disorder (12-month PDD), and a total of 15 patients with lifelong depressive disorder (LTMDD). , a total of 12 cases of 1-year depression (12-month MDD), and a total of 62 cases in the healthy control group.
The results of the cytometer showed that the deformability of monocytes, granule-monocytes and neutrophils was significantly increased in the lifelong persistent depressive disorder group compared with the control group (see Figure 2);
in the 1-year persistent depressive disorder group In the 1-year depression group, the deformability of lymphocytes increased; in the lifetime depression group, there was no change in the deformability of various blood cells. significantly changed.
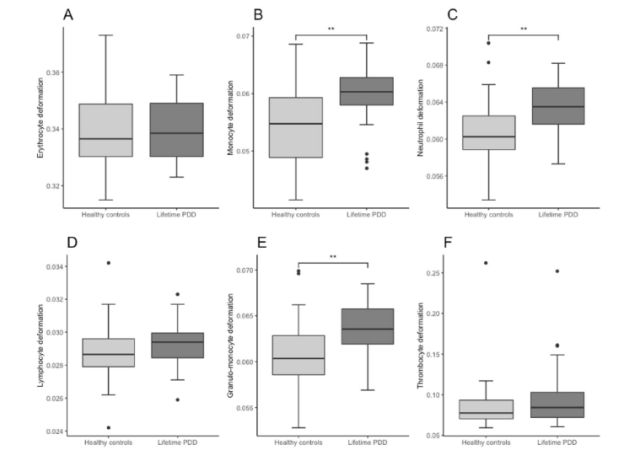 Figure 2. Boxplots of blood cell deformability in lifelong persistent depressive disorder and healthy controls
Figure 2. Boxplots of blood cell deformability in lifelong persistent depressive disorder and healthy controls
In order to confirm the correlation between the severity of depression and the enhancement of blood cell deformability, the researchers conducted a partial correlation analysis between each depression group and the control group, adjusting for age, gender, body mass index, and psychotropic drug factors (see Figure 3). .
RESULTS: In the lifetime persistent depressive disorder group, PHQ-9 scores were associated with increased monocyte, neutrophil, and granule-monocyte deformability .
In addition, PHQ-9 scores were independently associated with enhanced monocyte and erythrocyte deformability in 1-year persistent depressive disorder and 1-year persistent depressive disorder, respectively .
 Figure 3. Correlation between PHQ-9 score and blood cell deformability in each group
Figure 3. Correlation between PHQ-9 score and blood cell deformability in each group
So far, we can clarify that depression is associated with increased deformability of peripheral blood immune cells.
It is worth thinking about, why does this happen to the immune cells of depressed patients? The researchers speculate that this may be related to hyperactivation of the HPA axis and chronic low-grade inflammation .
Cortisol produced by activation of the HPA axis and pro-inflammatory factors produced by the inflammatory response can both affect the reorganization of the actin cytoskeleton to increase the deformability of cells [6].
In addition, increased cortisol and pro-inflammatory factors also affect lipid formation .
Lipids are an important component of cell membranes, and disturbance of lipid formation means that the stability of cell membranes may be reduced, thereby exhibiting increased cell deformability [7].
The present study is the first to assess the association between depression and cellular deformability of major blood cell types, clarifying the impact of depression on the mechanical characteristics of primary immune cells.
The researchers used a high-throughput real-time cell deformability counter combined with artificial intelligence image processing to provide the highest level of validity and reliability for clinical assessment of depression.
Of course, the limitations of the study are also obvious. The enrolled participants were not newly diagnosed patients who had never taken antidepressants, and the potential impact of drugs on cell deformability should not be underestimated.
In addition, the proportion of males was low, and there was a selection bias in terms of sex.
Changes in cellular mechanical characteristics are closely related to pathological processes and physiological functions, and the increased deformability of immune cells in patients with depression provides new insights into the pathophysiological mechanisms of depression.
The precise regulation of the mechanical characteristics of immune cells may become a new idea for the treatment of depression in the future.
references:
[1]. World Health Organisation (WHO). Depression and other common mental disorders
global health estimates. 2017.
[2 ].Walther A, Mackens-Kiani A, Eder J, et al. Depressive disorders are associated with increased peripheral blood cell deformability: a cross-sectional case-control study (Mood-Morph)[J]. Translational Psychiatry, 2022 , 12(1): 1-12.
[3]. Pariante CM. Why are depressed patients inflamed? A reflection on 20 years of research on depression, glucocorticoid resistance and inflammation. Eur Neuropsychopharmacol. 2017;27(6):554-559. doi:10.1016/j.euroneuro. 2017.04.001
[4]. Lynall ME, Turner L, Bhatti J, et al. Peripheral Blood Cell-Stratified Subgroups of Inflamed Depression. Biol Psychiatry. 2020;88(2):185-196. doi:10.1016/j.biopsych.2019.11. 017
[5]. Kubánková M, Hohberger B, Hoffmanns J, et al. Physical phenotype of blood cells is altered in COVID-19. Biophys J. 2021;120(14):2838-2847. doi:10.1016/j.bpj. 2021.05.025
[6]. Fay ME, Myers DR, Kumar A, et al. Cellular softening mediates leukocyte demargination and trafficking, thereby increasing clinical blood counts. Proc Natl Acad Sci US A. 2016;113(8):1987-1992. doi: 10.1073/pnas.1508920113
[7]. Ravetto A, Wyss HM, Anderson PD, den Toonder JM, Bouten CV. Monocytic cells become less compressible but more deformable upon activation. PLoS One. 2014;9(3):e92814. Published 2014 Mar 27. doi: 10.1371/journal.pone.0092814
First time: Study found elevated deformability of immune cells in people with depression
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



