Can Influenza Inhibit Cancer Lung Metastasis?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Can Influenza Inhibit Cancer Lung Metastasis?
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
“Nature Immunology”: Can Influenza Inhibit Cancer Lung Metastasis?
Researchers found that influenza can enhance the phagocytosis and cytotoxicity of alveolar macrophages and stimulate long-lasting anti-tumor immunity.
As the saying goes, “What doesn’t kill you makes you stronger”.
I believe everyone has heard of this sentence, but you may not think that this sentence also expresses the grievances and grievances between influenza, immunity and cancer.
Researchers from Zhejiang University School of Medicine , published an important research result in the famous journal “Nature Immunology” [1], which clarified the reason why influenza enhances the anti-tumor ability of the immune system . Wang Tao, a 2019 doctoral student in Yao Yushi’s team, is the first author of the paper .
They found that after the recovery of mice infected with influenza A virus (IAV), the resident alveolar macrophages (AMs) in the respiratory mucosa were trained by influenza virus to develop durable anti-tumor immunity (trained immunity, trained immunity) , this trained immunity suppressed lung metastasis of cancer cells even 120 days after infection .
Mechanistically, alveolar macrophages trained by influenza virus have enhanced phagocytosis and tumor cytotoxicity, and they will infiltrate into lung tumor lesions to exert anti-tumor effects, and this anti-cancer effect does not depend on T cells .
What’s even more amazing is that these influenza virus-trained alveolar macrophages are resistant to the tumor’s immunosuppressive microenvironment from the levels of epigenetics, transcriptome, and metabolism .

Screenshot of paper home page
We all know that whether we are infected with influenza virus or new coronavirus, our body will form immune memory after recovery, and our immune system will burst out a strong immune protection ability in the next round of pandemic.
Usually, when we mention immune memory, we automatically think of acquired immunity. In fact, a large number of studies in recent years have found that the body’s innate immunity can also produce memory after being stimulated.
Scientists named this immune memory “training immunity” [2]. Due to the lack of strict antigen/pathogen response specificity, trained innate immune cells theoretically have enhanced immune responses to various heterologous stimuli [2].
Although a large number of studies have explored the anti-infection function of trained macrophages in humans and experimental animals [3], the potential of trained macrophages in anti-tumor immunity is still unclear .
To understand the long-term effects of respiratory virus infection on lung anti-tumor immunity, Wang Tao et al. infected wild-type C57BL/6 mice with influenza A virus (IAV).
The influenza A virus successfully induced airway inflammation in mice, which recovered after about two weeks.
Thirty days after infection, they delivered fluorescently labeled B16 melanoma cells (B16-luc) into the lungs of mice by intravenous injection.
The results of the study showed that mice infected with influenza A virus had a significantly longer survival period and a lower lung tumor burden compared with uninfected mice (PBS).
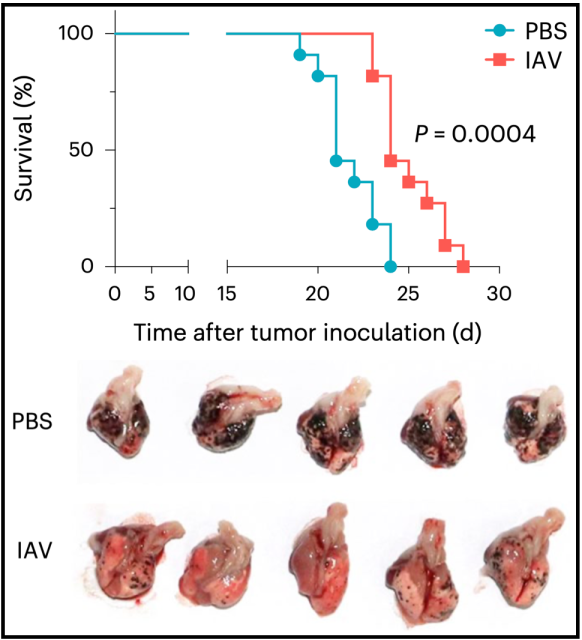
Mice infected with influenza A virus (IAV) have prolonged survival and lower lung tumor burden
What’s more, they found that the anti-tumor immunity induced by influenza A virus infection was very durable, and the enhancement of anti-tumor immunity was observed on the 60th day or even 120 days after infection ; and adenovirus infection can also induce similar anti-tumor immunity. Tumor Immunity Phenomena .
Notably, antitumor immunity induced by influenza A virus infection was not observed when melanoma cells were injected subcutaneously, but was observed when a breast cancer cell line that spontaneously metastasizes to the lungs was injected subcutaneously. Viral infection-induced antitumor immunity (less lung tumor burden).
Based on the above results, the researchers believe that respiratory virus infection can induce long-lasting lung-specific anti-tumor immunity.
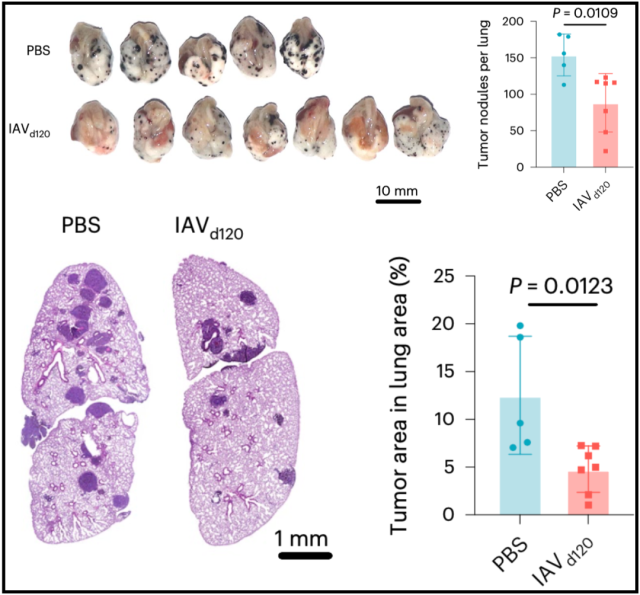
Antitumor immunity induced by influenza A virus infection lasts for 120 days
Having observed that influenza A virus infection induces anti-tumor immunity in the lungs, the next step was to understand how this happened.
found that the lung anti-tumor immune response induced by influenza A virus infection was independent of adaptive T cells and dependent on alveolar macrophages .
Thirty days after the mice were infected with influenza A virus, they compared the alveolar macrophages of uninfected or infected mice by various methods, and found that there were indeed huge differences between the two.
Specifically, alveolar macrophages from mice infected with influenza A virus had upregulation of gene transcription related to immune activation and effector function, and higher expression levels of MHC-II, and these macrophages were protected against influenza A virus.
After virus-independent antigen stimulation, more pro-inflammatory cytokines/chemokines are secreted, such as tumor necrosis factor (TNF), interleukin-6 (IL-6), and macrophage inflammatory protein 2 (MIP-2) wait .
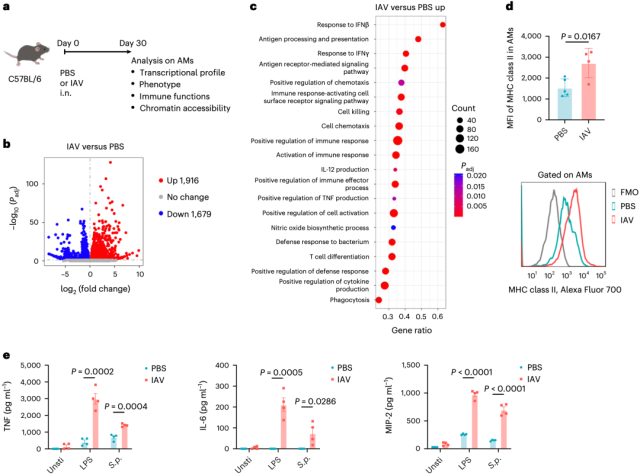
Effects of Influenza A Virus on Alveolar Macrophages of Mice
So where did these macrophages come from?
After a series of experiments, Wang Tao et al. confirmed that these alveolar macrophages were not derived from circulating monocytes, but tissue-specific resident macrophages . It is worth mentioning that they also found that alveolar macrophages decreased by nearly 90% in about a week after infection with influenza A virus, but the number of alveolar macrophages began to recover on the 9th to 11th day after infection.
That is to say, alveolar macrophages will proliferate rapidly during the recovery process, although influenza A virus infection will lead to a sharp decrease in alveolar macrophages. It is based on these proliferating alveolar macrophages that influenza A virus-induced tissue-specific training immunity can be formed .
In subsequent studies, Wang Tao et al. found that the phagocytosis and tumor cytotoxicity of alveolar macrophages trained by influenza A virus were enhanced, and this immune enhancement effect was dependent on interferon-γ (IFN-γ) and natural killing ( NK) cells .
More importantly, these alveolar macrophages have developed resistance to the tumor’s immunosuppressive microenvironment from the levels of epigenetics, transcriptome and metabolism. That is, they are immune to the tumor’s immunosuppressive capabilities.
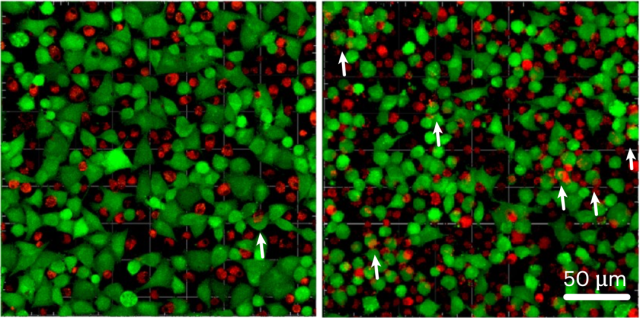
Enhanced phagocytosis
At the end of the study, Wang Tao et al. analyzed the data in several human lung cancer databases and found that the trained resident alveolar macrophages infiltrated in human lung cancer tissues were indeed related to anti-tumor immunity . This means that the mechanism found in the mouse model may also exist in humans.
In general, the research results of Yao Yushi’s team have given us a deeper understanding of the training immunity of innate immune cells.
Particularly intriguing is the prophylactic induction of antitumor immunity in tissue-resident macrophages as a potential anticancer strategy, especially for cancers with a high risk of lung metastases, such as melanoma and breast cancer .
references:
[1].Wang, T., Zhang, J., Wang, Y. et al. Influenza-trained mucosal-resident alveolar macrophages confer long-term antitumor immunity in the lungs. Nat Immunol (2023). https://doi .org/10.1038/s41590-023-01428-x
[2].Netea MG, Joosten LAB, Latz E, et al. Trained immunity: a program of innate immune memory in health and disease[J]. Science, 2016, 352(6284): aaf1098.
[3].Lérias JR, De Sousa E, Paraschoudi G, et al. Trained immunity for personalized cancer immunotherapy: current knowledge and future opportunities[J]. Frontiers in Microbiology, 2020, 10: 2924.
Can Influenza Inhibit Cancer Lung Metastasis?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



