How do tumors efflux T cells through lymphatic vessels?
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
How do tumors efflux T cells through lymphatic vessels?
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
How do tumors efflux T cells through lymphatic vessels?
Nature Immunology: First time Scientists reveal the mystery of tumor efflux of T cells through lymphatic vessels.
In clinical treatment, the most frustrating thing may be the immune rejection tumor.
This type of tumor appears to be surrounded by T cells, but the effect of immunotherapy is not satisfactory.
The reason is that these T cells around the tumor just watch and don’t do anything .
In order to break the trap set up by immune-rejecting tumors, scientists have put in a lot of effort.
Studies have found that collagen fibers produced by tumor-associated fibroblasts will deposit around the tumor parenchyma, forming a protective barrier, and T cells can only wait and see through the wall [1].
There are also research teams studying where the T cells surrounding tumors come from, and the team of Amanda W. Lund at NYU Langone Health Center is one of them.
Recently, Lund’s team published an important research result in the famous journal “Nature Immunology” [2], allowing us to once again see the means by which tumors deal with immune cells.
They found that under the control of tumors, tumor-associated lymphatic endothelial cells will produce the chemokine CXCL12, and the receptor CXCR4 on the surface of T cells (mainly expressing the stemness marker TCF1) binds and recognizes CXCL12, and then goes along the lymphatic vessels.
Leaving the inside of the tumor, it is sealed around the tumor .
It should be noted that this process is also regulated by tumor antigens . Specifically, high-affinity antigens can down-regulate CXCR4 and up-regulate the expression of CXCL12 decoy receptors, thereby reducing the sensitivity of T cells to CXCL12 and increasing the chance of T cells staying in the tumor. Unfortunately, there are a large number of low-affinity antigens in the tumor, as well as low-affinity antigen-presenting cells, so many T cells in the tumor are excluded from the tumor .
However, studies by Lund’s team have shown that inhibiting the activity of CXCR4 or the production of CXCL12 can allow T cells to remain in the tumor and enhance the therapeutic effect .

Screenshot of paper home page
In recent years, scientists have noticed that the presence of lymphatic vessels is associated with immune suppression.
In preclinical models, some scientists have also noticed that CD4 or CD8 positive T cells will leave the tumor microenvironment through lymphatic vessels [3]. However, the mechanism behind it is still unknown .
Lund’s team hypothesized that lymphatic vessels mediate the efflux of effector CD8-positive T cells, thereby limiting the accumulation of broadly functional T cells in the tumor microenvironment. Taking melanoma as the research object, they verified the above speculation.
Like other studies, they also observed immune rejection in a mouse model of melanoma: a large number of CD8-positive T cells gathered near the lymphatic vessels around the tumor, while there were very few T cells in the tumor .
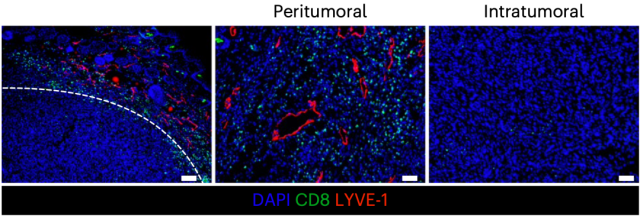
Immune rejection in a mouse model of melanoma
If the formation of tumor-associated lymphatic vessels is inhibited, T cells in the tumor increase .
Because circulating T cell levels remain unchanged and T cell proliferation levels are reduced in the lymphatic vessel-deficient tumor microenvironment, it can be argued that lymphatic vessels are indeed conduits for tumor efflux of T cells.
Based on experiments in mice, Lund’s team found that T cells with tumor antigen specificity were expelled from tumors, even T cells expressing high-affinity TCR were also expelled from tumors .
At the transcriptome level, intratumoral CD8-positive T cells were enriched for genes up-regulated during exhaustion, whereas CD8-positive T cells expelled outside the tumor were enriched for genes down-regulated during exhaustion.
Notably, expelled tumors were positive for the stemness marker TCF1, whereas T cells retained within the tumor were not.
We still remember a blockbuster research result published in Nature by Haydn Kissick’s team at Emory University School of Medicine in 2019 [4]: Stem cell-like CD8-positive T cells in tumors are the key to immunotherapy, and they will interact with Antigen-presenting cells interact to form independent anti-cancer “bases” .
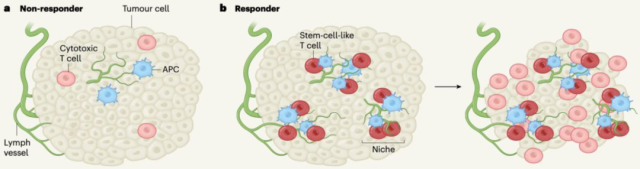
Stem cell-like T cells are the cornerstone of immunotherapy[5]
Combining these two studies, we will find that the tumor’s efflux through lymphatic vessels has removed the “base” of immune cells in the tumor.
After comparing human and mouse data, Lund’s team also found that T cells shed from the tumor microenvironment were more similar to T cells enriched in tumors of responders to immunotherapy .
Therefore, by inhibiting T cell efflux, it is possible to enhance the patient’s response to immunotherapy.
In order to find a way to inhibit T cell efflux, it is necessary to understand the mechanism of tumor-associated lymphatic vessels regulating T cell efflux.
The research results of Lund’s team showed that tumor-associated lymphatic endothelial cells produce chemokine CXCL12, and after CXCL12 binds to the receptor CXCR4 on the surface of T cells, it will promote T cells to leave the tumor along the lymphatic vessels and be sealed in the periphery of the tumor. And blocking the CXCL12-CXCR4 signaling pathway can keep T cells in the tumor.
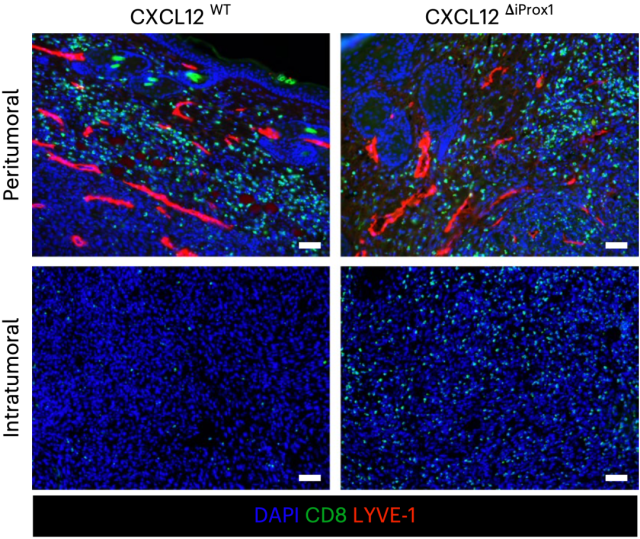
CXCL12 and T cell efflux
Interestingly, the expression level of CXCR4 depends on the affinity of TCR.
The stronger the affinity of TCR to antigen, the lower the level of CXCR4, the greater the possibility of T cells staying in the tumor; the lower the affinity of TCR to antigen, the lower the level of CXCR4.
The higher the level, the less likely the T cells are to remain within the tumor.
Lund and his colleagues believe that the antigens in the tumor microenvironment are extremely diverse, and differences in this diversity and affinity will lead to strong heterogeneity of effector T cells in the tumor.
The above mechanisms indicate that the CXCL12-CXCR4 signaling pathway is the key to improving the efficacy of immunotherapy.
Based on mouse studies, Lund’s team found that CXCR4 inhibitors can indeed improve the therapeutic effect of PD-L1 inhibitors, and even the specific elimination of CXCL12 in lymphatic vessels can significantly inhibit tumor growth.
In general, the study by the Lund team clarified the mechanism of tumor-associated lymphatic vessel efflux of T cells, as well as the types and characteristics of the effluxed T cells, which gave us a new understanding of cancer immunotherapy.
What’s more, they also identified a potential way to improve the efficacy of immunotherapy.
Lund and his colleagues said that in the future, they will conduct more in-depth research around tumor-associated lymphatic vessels to find more ways to prolong the residence time of T cells in tumors.
references:
[1].Grout JA, Sirven P, Leader AM, et al. Spatial positioning and matrix programs of cancer-associated fibroblasts promote T cell exclusion in human lung tumors. Cancer Discov. 2022. doi:10.1158/2159-8290.CD- 21-1714
[2]. Steele, MM, Jaiswal, A., Delclaux, I. et al. T cell egress via lymphatic vessels is tuned by antigen encounter and limits tumor control. Nat Immunol. 2023. https://doi.org/10.1038 /s41590-023-01443-y
[3].Li Z, Tuong ZK, Dean I, et al. In vivo labeling reveals continuous trafficking of TCF-1+ T cells between tumor and lymphoid tissue. J Exp Med. 2022;219(6):e20210749. doi: 10.1084/jem.20210749
[4].Caroline S. Jansen, Nataliya Prokhnevska, Viraj A. Master, et al. An intra-tumoral niche maintains and differentiates stem-like CD8 T cells[J]. Nature, 2019. DOI: 10.1038/s41586-019- 1836-5
[5].Kumar Vodnala S, Restifo NP. Identifying the source of tumour-infiltrating T cells. Nature. 2019;576(7787):385-386. doi:10.1038/d41586-019-03670-6
How do tumors efflux T cells through lymphatic vessels?
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



