Lancet: Poor countries with higher postoperative mortality of cancer patients
- Aspirin: Study Finds Greater Benefits for These Colorectal Cancer Patients
- Cancer Can Occur Without Genetic Mutations?
- Statins Lower Blood Lipids: How Long is a Course?
- Warning: Smartwatch Blood Sugar Measurement Deemed Dangerous
- Mifepristone: A Safe and Effective Abortion Option Amidst Controversy
- Asbestos Detected in Buildings Damaged in Ukraine: Analyzed by Japanese Company
Lancet: Poor countries with higher postoperative mortality of cancer patients
Lancet: Poor countries with higher postoperative mortality of cancer patients. Compared with patients in high-income countries, patients in upper-middle-income and lower-middle-income countries tend to have more advanced disease, but researchers have found that cancer staging is not sufficient to explain changes in mortality or postoperative complications.
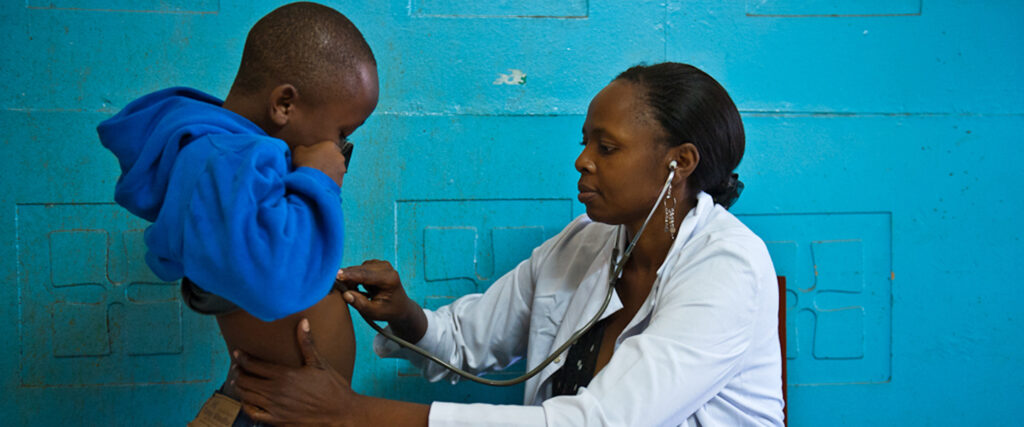
[Article from the U.S. News website “Eureka Alert” January 26, 2021] Title: Postoperative mortality of cancer patients in low-income countries is higher.
A global observational study published in The Lancet by a research team led by the University of Edinburgh explored the overall differences in complications and deaths after three common cancer operations, and found that cancer patients in low-income, low- and middle-income countries have undergone surgery The probability of death may be four times that of high-income countries, and low-income countries are unlikely to have post-operative care infrastructure and oncology treatment services.
Between April 2018 and January 2019, researchers recruited 15,958 patients from 428 hospitals in 82 countries who had undergone breast, colorectal, or gastric cancer surgery. These patients came from high-income, middle-to-high income As well as low- and middle-income countries, 53% (8,406 people) of patients have received breast cancer surgery, 39% (6,215 people) have received colorectal cancer treatment, and 8% (1337 people) have received gastric cancer Surgical treatment.
Researchers analyzed common deaths or major complications within 30 days after surgery. The mortality rate of gastric cancer patients in low- and middle-income countries (33 deaths out of 326 patients, and the probability of death is 3.72) is the highest in high-income countries (out of 702 patients). The mortality rate of colorectal cancer patients in low- and middle-income countries (63 deaths among 905 patients, 4.59 deaths) is more than 3 times that of high-income countries (94 deaths among 4142 patients). The mortality rate of colorectal cancer patients in high-income countries is twice that of patients in high-income countries (47 deaths out of 1102 patients); there is no difference in the mortality rate of patients in different countries 30 days after breast cancer surgery.
Patients in all income groups had similar postoperative complications, but compared with patients in high-income countries (121 deaths out of 693 patients), patients in low/low-middle-income countries died of severe complications within 30 days (96 deaths out of 133 patients, 6.15% chance of death) is 6 times more likely than in high-income countries (121 deaths out of 693 patients), and the mortality rate of patients in high-middle-income countries is almost that of high-income countries 4 times (58 deaths out of 151 patients, 3.89 chance of death).
Compared with patients in high-income countries, patients in upper-middle-income and lower-middle-income countries tend to have more advanced disease, but researchers have found that cancer staging is not sufficient to explain changes in mortality or postoperative complications.
Researchers have evaluated the hospital facilities and practices of different income groups and found that hospitals in high-middle-income countries and low-income/low-middle-income countries have post-operative care infrastructure (such as designated post-operative rehabilitation areas and continuously available intensive care facilities) And cancer care pathways (such as oncology services) are less likely. Further analysis shows that the lack of post-operative care infrastructure is associated with low/low-middle income countries (7-10 deaths per 100 major complications) and upper-middle-income countries (5-8 per 100 major complications) Deaths) related to the increase in the number of deaths.
Mr. Malcolm West, academic leader at the University of Southampton, commented: “I am honored to contribute to this landmark study. The death of postoperative complications due to ineffective rescue is an important global problem. As a knot Rectal surgeon, I have found this worrying situation that patients in low- and middle-income countries (LMIC) have a higher degree of cancer progression than high-income countries.
Interestingly, the incidence of advanced cancer alone does not fully explain the high mortality and complication rates we have seen. The top priority is to improve the global health care system (especially in low- and middle-income countries) to detect and intervene when complications occur and save lives after cancer surgery. “
Professor Ewen Harrison of the University of Edinburgh said: “Our study provides in-depth data on patient complications and deaths within 30 days after cancer surgery for the first time in the world. The link between postoperative care and reduced mortality after major complications shows that improvement Nursing systems to detect and intervene when complications occur can help reduce mortality after cancer surgery.”
The author also believes that the study has limitations. Researchers only study the early results after surgery, and will study long-term results and other cancers in the future. In the case of limited resources, it may be difficult to obtain and understand the results, which will affect the team’s discovery of the surgical effect. Further detailed analysis is still needed to provide more reliable evidence about the association between patient prognosis and hospital facilities.
(source:internet, reference only)
Disclaimer of medicaltrend.org



