Hormonal contraceptives is not associated with children’s brain tumors
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Hormonal contraceptives is not associated with children’s brain tumors
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Hormonal contraceptives is not associated with children’s brain tumors.
JAMA: Danish study of 1.18 million children shows that maternal use of hormonal contraceptives is not associated with offspring’s risk of central nervous system tumors.
Sex hormones are also carcinogens [1].
Previous large-scale population cohort studies have found that taking estrogen and progesterone increases the risk of breast cancer in menopausal women [2]; while taking estrogen alone also increases the risk of endometrial cancer in women. In addition, some studies have shown that the risk of childhood non-lymphocytic leukemia can be increased by nearly three times when the mother takes hormonal contraceptives during the perinatal period [3].
Central nervous system tumors are the most common and deadly childhood tumors after childhood leukemia. Globally, the incidence of childhood central nervous system tumors is increasing year by year [4]. However, epidemiological studies have found that the increased incidence of the disease cannot be simply attributed to improved diagnosis and the influence of traditional risk factors (including familial inheritance, exposure to toxicants, and ionizing radiation).
So, does the mother’s use of hormonal contraceptives increase the risk of offspring suffering from central nervous system tumors?
To date, five studies have assessed the relationship between peri-pregnancy intrauterine sex hormone exposure and the risk of childhood CNS tumors.
Of these, four were case-control studies and concluded that the two were not associated . However, a fifth case-cohort study found an increased risk of central nervous system tumors in children after perinatal use of hormonal contraceptives [5] .
What is right and wrong?
Recently, the team of Susanne K. Kjaer from the Research Center of the Danish Cancer Society, using a cohort study based on the national population in Denmark, made a final call to this disparate issue and drew a complete stop.
They combined population data from the Danish Medical Birth Registry, the Danish National Prescription Registry and the Danish Cancer Registry, and tracked 1.18 million Danish children born between 1996 and 2014. They counted the mother’s perinatal sex hormone use and whether the children had central nervous system disease.
In the case of systemic tumors, it was found that maternal use of hormonal contraceptives did not increase the risk of central nervous system tumors in children.
The research results have been published in the first issue of the international top medical journal JAMA in 2022 [6].

Screenshot of JAMA official website paper
The Danish Medical Birth Registry records birth-related information for all Danish nationals. First, the researchers retrieved data on all live births of children born in Denmark from January 1, 1995 to December 31, 2014, excluding cases where the mother’s pregnancy time was unknown or missing, and established a population of more than 1.18 million Danish children. national cohort.
In Denmark, hormonal contraceptives can only be purchased with a doctor’s prescription . The researchers then used maternal hormonal contraceptive use from the Danish National Prescription Registry. In this study, hormonal contraceptives were defined as estrogen, progestin combined, or progestin alone. Routes of administration include oral or parenteral drugs including injections, implants, IUDs, contraceptive patches and vaginal rings.
Second, the study divided the 1.18 million children into three groups using the first 3 months of pregnancy as a boundary: ” recent use ” ( use within the first 3 months of pregnancy, including use during pregnancy ), ” previous use ” ( pre- pregnancy use) Stop taking it for more than 3 months ) and ” never use ” three groups, accounting for 11.5% , 65.7% and 22.8% , respectively .
Thanks to Denmark’s mandatory cancer reporting policy, the Danish Cancer Registry compiles cancer-related information for all citizens. Accordingly, the researchers counted the incidence of central nervous system tumors in children in these three groups. Finally, by comparing the hazard ratio (HR) and the incidence difference (IRD) of childhood central nervous system tumors, the study concluded.

Inclusion process for study cohorts
The results showed that a total of 725 children developed central nervous system tumors during an average follow-up period of up to 12.9 years .
There were 342 female patients, accounting for 47.2%. Among them, there were 220 children with central nervous system tumors in the “never use” group, with an adjusted incidence rate of about 5.3/100,000-years; 84 children in the “recently used” group, with an adjusted incidence rate of 5.0/100,000 people Years; 421 children in the “previous use” group, with an adjusted incidence rate of 4.5/100,000-years.
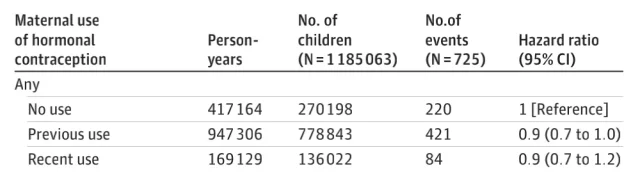
The situation of children suffering from central nervous system tumors in each group
The hazard ratio for developing a central nervous system tumor was 0.95 [95%CI, 0.74-1.23] in the “recent” and “previous” groups of sex hormone-exposed children compared with the “never” group without sex hormone exposure, respectively . and 0.86 [95%CI, 0.72-1.02], the difference in incidence was −0.3 [95%CI, −1.6-1.0] and −0.8 [95%CI, −1.7-0.0], respectively.
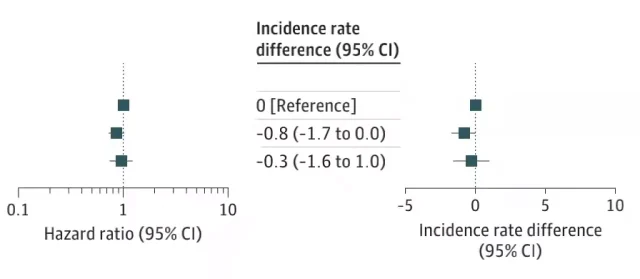
Research result
In other words, among Danish children, there was no significant relationship between maternal use of hormonal contraception and the risk of developing CNS tumors in the child!
In addition, the researchers found that the use of hormonal contraception, whether combined oral, non-oral, oral progestin only, or non-oral products, or recent or past use, was significantly associated with CNS compared with no use of hormonal contraception. The increased risk of systemic tumors was not statistically significant .
In this regard, H.Irene Su, a professor of obstetrics and gynecology at the University of California, San Diego, mentioned in a JAMA editorial in the same period [7]: “Women can use hormonal contraception with confidence, and their offspring will not have an increased risk of central nervous system tumors.”
This cohort study uses population information from an entire country, spans nearly 20 years, covers millions of children, and integrates multiple systems of birth records, drug use and cancer registries.
The data is complete and complete, with both scale and precision, which greatly increases the results. generalizability and credibility of conclusions.
However, the study also has some imperfections. First, because childhood CNS tumors are relatively uncommon, and in Denmark, with a population of less than 6 million, there are not too many cases available for group analysis, which may limit the statistical precision of some values;
second, due to the observational design of the study , the possibility of residual or unknown confounding cannot be completely ruled out; in addition, due to the large number of comparisons between groups, there may be a risk of Type 1 error.
At present, Denmark is the only country in the world that registers all its citizens. Like other information, all medical records of Danes from birth to death are registered and available for inquiry.
The tradition of data registration in detail, with a long history, variety and complete functions, has made Denmark a paradise for epidemiologists and an Eden for etiology research.
references
[1] https://www.cancer.gov/about-cancer/causes-prevention/risk/hormones
[2] Collaborative Group on Hormonal Factors in Breast Cancer. Type and timing of menopausal hormone therapy and breast cancer risk: individual participant meta-analysis of the worldwide epidemiological evidence. Lancet. 2019;394(10204):1159-1168. doi: 10.1016/S0140-6736(19)31709-X
[3] Hargreave M, Mørch LS, Andersen KK, Winther JF, Schmiegelow K, Kjaer SK. Maternal use of hormonal contraception and risk of childhood leukaemia: a nationwide, population-based cohort study. Lancet Oncol. 2018;19(10) :1307-1314. doi:10.1016/S1470-2045(18)30479-0
[4] Steliarova-Foucher E, Fidler MM, Colombet M, et al. Changing geographical patterns and trends in cancer incidence in children and adolescents in Europe, 1991-2010 (Automated Childhood Cancer Information System): a population-based study. Lancet Oncol. 2018;19(9):1159-1169. doi:10.1016/S1470-2045(18)30423-6
[5] Linet MS, Gridley G, Cnattingius S, et al. Maternal and perinatal risk factors for childhood brain tumors (Sweden). Cancer Causes Control. 1996;7(4):437-448. doi:10.1007/BF00052670
[6] Hargreave M, Mørch LS, Winther JF, Schmiegelow K, Kjaer SK. Association Between Maternal Hormonal Contraception Use and Central Nervous System Tumors in Children. JAMA. 2022;327(1):59-66. doi:10.1001/jama .2021.22482
[7] Spector LG, Moertel CL, Su HI. Maternal Contraceptive Use and Central Nervous System Tumors in Offspring. JAMA. 2022;327(1):39-40. doi:10.1001/jama.2021.21809
Hormonal contraceptives is not associated with children’s brain tumors
(source:internet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



