General evaluation of PENG block used in hip surgery
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
General evaluation of PENG block used in hip surgery
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- What is the difference between Atorvastatin and Rosuvastatin?
- How long can the patient live after heart stent surgery?
General evaluation of PENG block used in hip surgery.
PENG block is a new type of regional nerve block proposed in recent years.
Many articles have reported its application in hip surgery and hip fracture pain, which has attracted the attention of researchers.
At present, the commonly used regional analgesia techniques for hip surgery include femoral nerve block, iliac fascia block and lumbar plexus block.
Because of the complex nerve distribution in the hip, the above methods are still difficult to meet the needs of surgical anesthesia.
In 2018, GIron-Arango and others proposed for the first time ultrasound-guided intra-articular nerve (PENG) block with local anesthetic injection at the myofascial plane between the iliopsoas muscle and the posterior pubic body as a new regional analgesic technique .
This issue brings a Scoping Review published in “Regional Anesthesia & Pain Medicine” to discuss the effectiveness and safety of PENG block in hip surgery and hip fracture analgesia.

Background and methods
One of the difficulties in analgesia of hip pain is its complex innervation. In an anatomical study, Short et al. proved that the sensory nerve innervation of the anterior capsule of the hip joint includes the articular branches of the femoral nerve, the obturator nerve, and the accessory obturator nerve.
In addition, the “high” branch of the femoral nerve plays a greater role in the sensory innervation of the anterior capsule of the hip than previously thought.
In almost all dissected cadavers (92%), the femoral nerve has a “high” branch on the cephalic side of the inguinal ligament, so it is difficult to block this with sub-inguinal techniques (such as iliac fascia block or femoral nerve block) A nerve.
In addition, techniques such as iliac fascial space block often cannot adequately block the obturator nerve, which also provides sensory innervation for the anterior capsule of the hip.
A recent review of various regional analgesia techniques such as femoral nerve block, iliac fascia block, and lumbar plexus block by Cochrane et al. showed that the numerical pain score (NRS) decreased by an average of 3.4 points after the block was completed 30 minutes; although This is a statistically significant reduction in pain, but two international guidelines question whether the pain reduction in patients with femoral neck fractures from the currently widely used nerve block is clinically relevant compared with systemic analgesia.
In 2018, GIron-Arango et al. described ultrasound-guided peripheral joint capsule nerve block (PENG block) for the first time.
Their study found that the NRS score of PENG block in patients with hip fractures was reduced by an average of 7 points, and there was no Causes motor block.
The author conducted a comprehensive and systematic review of the literature according to the PRISMA guidelines. The key words are “pericystic nerve block”, “autonomic nerve block”, “nerve block”, “plane block”, “PENG block”, “inguinal iliac fascia block”.
Eligible articles were written in English, describing the application of PENG block in adult or pediatric patients with fracture or hip joint pain caused by surgery. There is no limit to the number of patients included.
Taking into account the first publication date of the PENG block, a search was conducted on articles published after January 2018.
Studies describing the use of PENG block for other indications (such as femoral shaft fractures, pelvic fractures, periprosthetic femoral fractures, urology, soft tissue or vascular surgery), studies without an English version, and studies where the full text is not available are excluded.
Research results
The database screened 345 articles, 20 of which met the inclusion criteria, and a total of 74 patients. All 20 articles are case reports or case series reports, published from November 2018 to April 2020. See Table 1 for details.
Table 1 Overview of PENG block literature
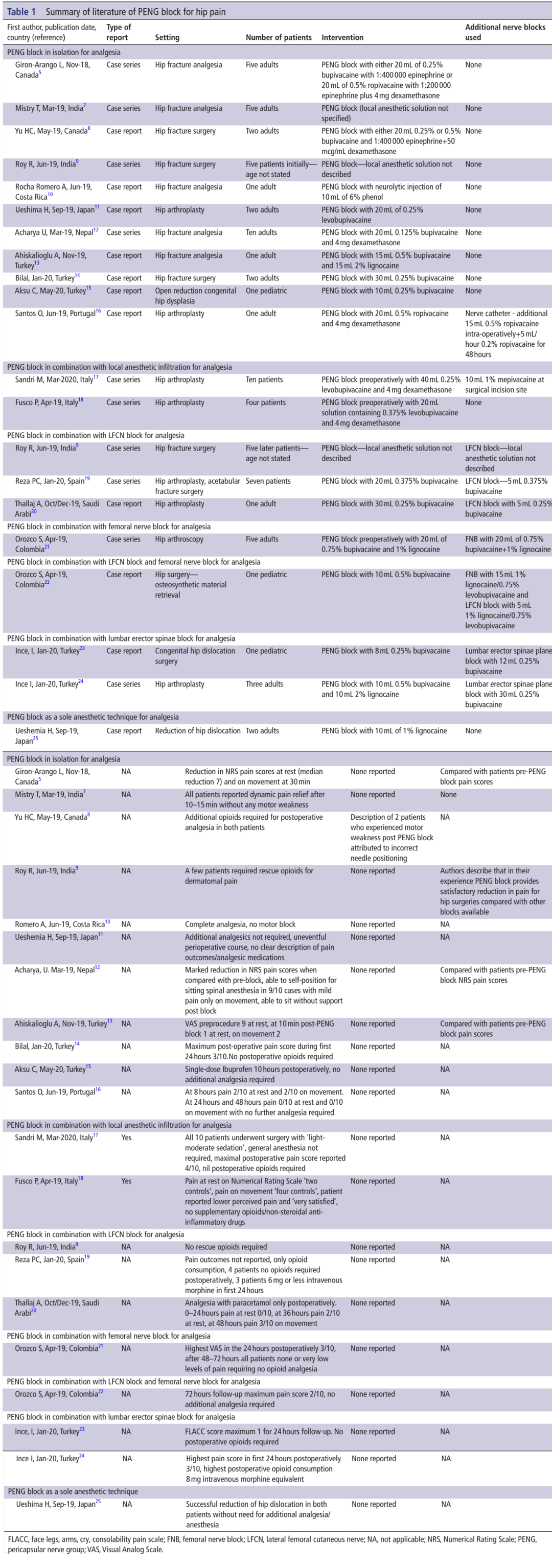
Analgesia and anesthesia effect
PENG block alone: In 11 studies, a total of 35 adult patients and 1 pediatric patient only used PENG block for analgesia, including hip dislocation reduction, hip fracture analgesia, and hip surgery.
These studies indicate that PENG block provides analgesia, which may reduce or eliminate the need for oral or intravenous opioids. In a hip fracture surgery study involving 5 patients, a small number of patients had pain in the distribution area of the lateral femoral cutaneous nerve.
In addition, in 2 adult patients with hip dislocation reduction surgery, the patient was not combined with general anesthesia, other nerve blocks, or sedation.
PENG block combined with other regional analgesic techniques: In 9 studies of a total of 32 adult patients and 1 pediatric patient, PENG block combined with local anesthetic infiltration or other nerve blocks, such as femoral nerve block or lateral thigh With cutaneous nerve block, these patients underwent hip arthroscopy, hip replacement, hip fracture surgery, or hip prosthesis removal.
All reports indicate that analgesia is good within 72 hours after surgery, and there is no need for opioids. According to reports, a child with congenital hip dysplasia, combined with PENG block and lumbar erector spinae block, had a maximum postoperative NRS score of only 1 without additional opioids; 3 cases of hip arthroplasty The patients also used PENG block combined with lumbar horizontal erector spinae block.
The maximum NRS score was 3 points after 24 hours, and the maximum intravenous morphine equivalent was 8 mg.
Technical problems of PENG block
Ten studies reported the use of low-frequency ultrasound probes, four studies used linear high-frequency ultrasound probes, and six studies did not specify which ultrasound probe was used.
There is also no study comparing the effects of different ultrasound probe choices. In 19 studies, patients received a single nerve block.
In addition to the study by Santos et al., which reported an adult patient undergoing hip replacement surgery with a continuous nerve block, the patient did not need a continuous nerve block within 72 hours after surgery.
Further analgesia. At present, there is no research report on the effective time of PENG block, the effect of different local anesthetic concentrations, and the effect of adjuvants in local anesthetics.
Motor weakness:
A study reported 2 patients with quadriceps weakness after PENG block.
The two patients encountered technical difficulties in the implementation of PENG block, which may be due to the spread of local anesthetics beyond the PENG block area. , Resulting in femoral nerve block, but quadriceps weakness was recovered within 48 hours.
Adverse events:
None of the studies reported systemic toxicity of local anesthetics, allergic reactions, permanent nerve damage, or other serious adverse events of PENG blockade.
Discussion and Conclusion
In the above review, the author believes that the current evidence for recommending PENG block is insufficient. Based on the existing evidence, PENG block can provide analgesia, but because the literature so far is limited to case reports and case series reports, there is a high publication bias, so it is not yet possible to conclude whether PENG block is safe and effective.
Theoretically speaking, PENG block has potential advantages over traditional hip regional analgesia (such as femoral nerve or iliac fascial space block): PENG block can cover more extensively and completely dominate the hip Sensory nerves, so as to achieve more effective regional analgesia, and may reduce postoperative pain.
While improving patient satisfaction, reduce postoperative opioid consumption, thereby reducing opioid-related adverse events and long-term dependence on opioids.
In addition, if a larger sample size of research proves that PENG block has no movement disorders, patients can be mobilized to participate in rehabilitation training early, which will help early recovery; currently available literature reports are not enough to recommend PENG block as a hip replacement The only method of anesthesia for surgery or other operations.
Technically speaking, the easily recognizable anterior inferior iliac spine, iliac pubic bulge, and iliopsoas ultrasonographic signs also make the PENG block at least comparable to other nerve blocks.
In view of the fact that the current literature does not describe any serious adverse events of PENG block, the author has raised some concerns about the safety of PENG block: PENG block may have potential risks for patients with coagulation disorders or receiving anticoagulant therapy.
In addition, during the implementation of PENG block, there is a possibility that the puncture path passes through the femoral nerve or the lateral femoral cutaneous nerve to cause injury.
In order to avoid permanent damage caused by nerve transection, the author recommends that the femoral nerve be carefully scanned and identified before the PENG block is performed.
However, the diameter of the lateral femoral cutaneous nerve is smaller and it is more difficult to identify on ultrasound.
Finally, if a more medial approach or a medial to lateral approach is used, it may cause damage to the pelvic segment of the ureter.
The author also pointed out that due to the retrieval method, articles related to PENG block published in languages other than English were omitted. In addition, due to the heterogeneity of the current reports of PENG block in indications, combination with other nerve blocks, different local anesthetics used, follow-up and difference in results, it is impossible to determine its efficacy based on current data.
Therefore, the current research is to describe and summarize the existing evidence in the form of a scope review to determine the areas of future research.
In view of the fact that the existing literature is limited to case reports and case series reports, randomized controlled trials are needed to compare PENG block with other nerve blocks (such as iliac fascial space block, femoral nerve block, lumbar horizontal erector spinae block Block or a combination of multiple blocks) to provide evidence of whether the PENG block technique can effectively block hip pain.
The author also mentioned that there are currently several registered randomized controlled trials comparing PENG block with placebo block and other nerve blocks for hip pain in patients, with the purpose of providing better results for PENG block in the treatment of hip pain. Good evidence.
Therefore, a large-scale cohort study is needed to explore its safety.
In short, from the current literature, the author believes that PENG block as a new type of hip analgesia is not only feasible, but also promising, but more clinical trials and controlled studies are needed to determine its safety And effectiveness.
Expert Comments:
PENG block is a new type of regional nerve block proposed in recent years. Many articles have reported its application in hip surgery and hip fracture pain, which has attracted the attention of researchers.
The research team conducted a systematic search for this hot spot and found that since the introduction of the blocking method, only cases and case series have been reported, and no relevant RCT studies have been retrieved.
Therefore, the research team conducted a general evaluation of the safety and effectiveness of PENG block in hip surgery and hip fracture pain.
The team believes that PENG block has more potential advantages:
1. The ultrasound image of PENG block is simple and easy to identify, and there is no obvious difference from traditional hip block;
2. PENG block can cover the sensory nerve innervating the hip more widely and completely, provide more effective regional analgesia, and effectively relieve pain;
3. The effective analgesic effect reduces the consumption of opioids and the occurrence of related adverse events;
4. The current literature does not see obvious quadriceps dyskinesia, which is conducive to early activities and promotes early recovery;
5. There are no reports of adverse events related to nerve block in the current literature.
The limitations of this article have been clearly mentioned by the author: the team only selects documents written and published in English, and there is a possibility that the search may be missed; secondly, due to the heterogeneity of the blocked reports, it is impossible to determine the exact results based on current data.
In addition, given that the block is a newly proposed concept and lacks a large sample size, multi-center RCT study, compared with the traditional block method, whether the PENG block has more advantages in the effect of hip pain, More high-quality evidence is still needed, and we look forward to further exploration and verification by researchers.
General evaluation of PENG block used in hip surgery
(source:internet, reference only)
Disclaimer of medicaltrend.org



