Stem cells can reverse premature ovarian failure
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Stem cells can reverse premature ovarian failure
- Should China be held legally responsible for the US’s $18 trillion COVID losses?
- CT Radiation Exposure Linked to Blood Cancer in Children and Adolescents
- FDA has mandated a top-level black box warning for all marketed CAR-T therapies
- Can people with high blood pressure eat peanuts?
- What is the difference between dopamine and dobutamine?
- How long can the patient live after heart stent surgery?
Stem cells can reverse premature ovarian failure.
Everyone has a heart for beauty, and many women dream of staying young forever.
But in fact, with the passage of time, when you see bags under your eyes and white hair in the mirror, do you feel extremely panic and sigh that the beauty is easy to grow old?
In fact, while the appearance is getting old, the most important reproductive organ of women, the ovary, is also slowly declining in function. Maybe its performance is not as obvious as the appearance of aging, but as long as you observe carefully, you can find some clues as soon as possible!
How to find the clues of ovarian recession?
1. Changes in body weight and posture
Among the many signs of aging in women, weight change is often very common and sensitive, which is often referred to as “fat”.
The aging of the ovary is significantly earlier than the aging of the whole body. Most women will gain 4.5 kg in weight during menopause, and will gain 0.9-1.4 kg per year after aging.
The body’s basal metabolism is different, and the posture will be very different.
A Japanese study shows that women’s aging starts from the abdomen.
Once you enter the aging of the ovary, you will find that the graceful curve of youth has quietly disappeared, abdominal fat has begun to accumulate, waist circumference has increased, lower limbs have become thinner, and elegant necks have begun to shorten, mostly manifested as weight gain.
2. Shortening of the menstrual cycle
As the saying goes, menstruation is the “barometer” of women’s health, “Anyone who sees a woman’s disease, ask the scriptures first” .
A shortened menstrual cycle is one of the easiest signs of ovarian decline.
Because with the increase of age, the number of remaining follicles in the ovary decreases, and the number of available follicles decreases accordingly, so the level of inhibin B secreted by granulosa cells in the early follicular phase decreases, the level of FSH increases, and FSH advances in advance Elevation accelerates follicular development, leading to earlier recruitment of the dominant follicle, shortening the follicular phase, and clinical manifestations of a shortened menstrual cycle.
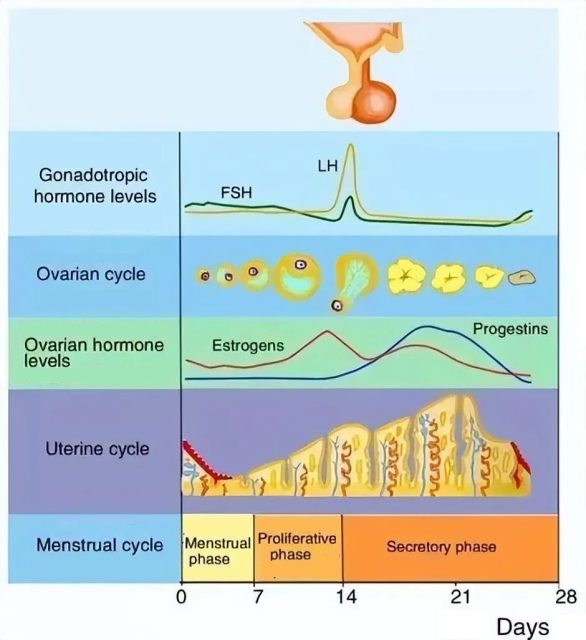
(Picture: The formation principle of the menstrual cycle, and changes in the ovary and endometrial lining)
The shortening of the menstrual cycle, that is, the shortening of the follicular phase, means that the ovarian reserve function is decreased.
If your cycle was 35-40 days in the past, and gradually shortened to 25-30 days, you should be alert to the aging of the ovaries.
Once a woman is nearing menopause, ovulation becomes very irregular, the menstrual cycle becomes more irregular, and menopause occurs when the follicles are depleted.
3. Always fail to conceive
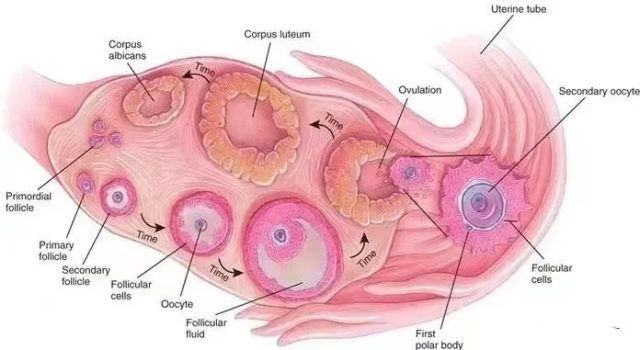
When a woman is still a fetus, the ovary contains about 6 to 7 million oocytes at 20 weeks of its embryo.
A baby girl is born with only 1 to 2 million oocytes left, and by puberty, only 300,000 to 500,000 oocytes are left.
During the reproductive years, a woman will release approximately 400 to 500 mature eggs in her lifetime.

With age, women’s oocyte reserve becomes less and less, and ovarian function gradually declines. The age of 35 is an important turning point.
One review found that women who were infertile at age 35 had their fertility reduced by age 30. Then you will experience infertility, shortening of the menstrual cycle, irregular menstruation, etc., and eventually menopause.
The ovary is a warm house for human beings to nurture new life. However, some women are still in childbearing age, and premature ovarian failure leads to infertility and the possibility of losing reproductive life.
Disease Overview of Premature Ovarian Failure
Premature ovarian failure (POF) refers to ovarian failure due to various causes before the age of 40 in women, and is considered an “incurable disease” leading to infertility.
The diagnostic criteria of the disease refer to: amenorrhea for at least 4 months before the age of 40, and 2 or more blood FSH>40U/L (the interval between two examinations is more than 1 month), estradiol <73.2pmol/L . The incidence of the disease is more than 1% in women of reproductive age.
And in recent years, it has shown an upward and younger trend.
The two major threats to women’s reproductive health from premature ovarian failure are reduced estrogen levels and loss of fertility.
Reduced estrogen levels increase women’s risk of osteoporosis and coronary heart disease .
Women who are in childbearing period have early amenorrhea and loss of fertility, and are prone to psychological problems such as depression and anxiety.
With the progress of stem cell research, it provides a new way for humans to understand the occurrence and development of diseases and develop new treatment methods.
Stem cell therapy has made great progress in the field of basic research, and some research results have begun to be applied in various clinical trials such as tumor diseases, autoimmune system diseases, nervous system diseases, cardiovascular diseases, etc.
Many clinical data, many related reports on stem cell clinical research and application have been published.
A variety of stem cells are used to treat premature ovarian failure (POF)
Stem cells have the ability to repair and regenerate themselves, and recent studies on animal models of POF have shown that stem cell therapy can improve ovarian structure and function, so stem cell transplantation may be an effective treatment for premature ovarian failure (POF).
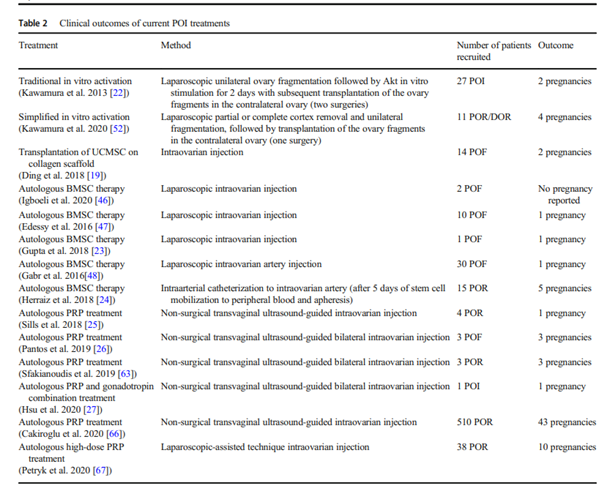 Table 1 (from literature [1]): Clinical outcomes of current POI treatments
Table 1 (from literature [1]): Clinical outcomes of current POI treatments
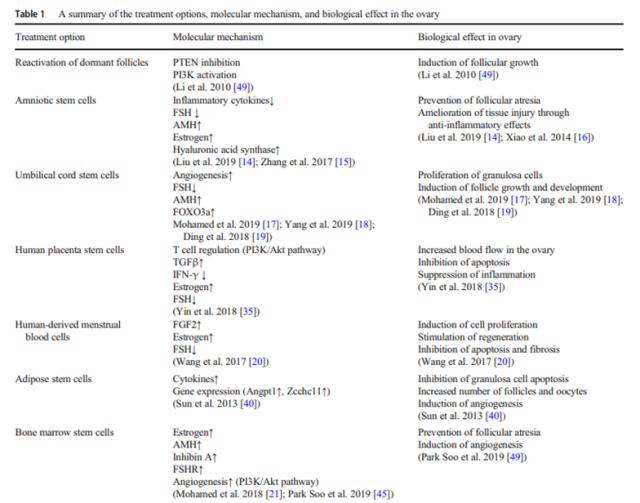
Table 2 (from literature [1])
NO.1 Human Amniotic Stem Cells (hAMSC)
Human amniotic stem cells (hAMSCs) are stem cells isolated from the amniotic membrane. Human amniotic stem cells (hAMSCs) possess multiple differentiation abilities and anti-inflammatory effects similar to other pluripotent mesenchymal stem cells (MSCs).
Studies have found [3] that transplantation of human amniotic stem cells (hAMSC) in experimental mice can reduce inflammatory cytokines, increase estrogen and reduce FSH levels, thereby maintaining continuous and healthy growth of follicles, reducing follicle atresia rate and restoring fertility.
NO.2 Umbilical cord mesenchymal stem cells (UCMSC)
Umbilical cord mesenchymal stem cells (UCMSCs) are multipotent, non-hematopoietic progenitor cells that can differentiate into multiple cell lineages.
Animal experiments have shown [4] that umbilical cord mesenchymal stem cell (UCMSC) transplantation can restore the ovarian function and reproductive potential of POI mice, significantly reduce the level of FSH and increase the level of serum AMH.
The mechanism of action of umbilical cord mesenchymal stem cells may be due to the increase of ovarian angiogenesis, which promotes the proliferation of granulosa cells and the growth and development of follicles.
NO.3 Placenta-derived stem cells (hPMSCs)
Human placenta-derived mesenchymal stem cells (hPMSCs) are also pluripotent, non-hematopoietic progenitor cells with highly differentiated and proliferative potential.
Compared with other types of stem cells, human placenta-derived mesenchymal stem cells (hPMSCs) are easily obtained.
In animal experiments [5] , mice injected with placenta-derived stem cells (hPMSC) intravenously restored ovarian endocrine function mainly through two pathways: increasing mouse transforming growth factor beta (inhibiting inflammation and contributing to the recovery of ovarian function) and reducing interference hormone gamma (inhibits ovulation and promotes follicular atresia) .
NO.4 Bone marrow mesenchymal stem cells
Bone marrow mesenchymal stem cells (BMSCs) are low-immunogenic adult stem cells that, like other stem cells, have proliferative and pluripotent differentiation potential and, under appropriate conditions, can differentiate into bone, cartilage, and adipocytes.
It has the effect of enhancing endogenous cell function and regulating immune response, and can be used to repair tissue damage.
Furthermore, bone marrow mesenchymal stem cells (BMSCs) are easily isolated and grown in vitro. Several clinical trials have shown [6] that women with POI have increased baseline estrogen levels, improved menopausal symptoms and even successfully conceived through autologous bone marrow mesenchymal stem cell transplantation.
Summary: Mesenchymal stem cells have broad prospects for the treatment of premature ovarian failure
Premature ovarian failure (POF) greatly affects the physical and mental health of young women.
At present, hormone therapy is mainly used to alleviate the symptoms of estrogen deficiency, but the effect is not good. Stem cells have the potential for self-improvement and regeneration, which can improve ovarian function, increase the number of follicles, increase sex hormone levels, reduce granulosa cell apoptosis, and can be used to treat premature ovarian failure (POF) and infertility.
Mesenchymal stem cell transplantation has broad application prospects in the treatment of premature ovarian failure (POF).
It is believed that with the progress of research, mesenchymal stem cells will bring good news to more patients with premature ovarian failure!
References:
[1] Ulin, M., Cetin, E., Hobeika, E., Chugh, RM, Park, HS, Esfandyari, S., & Al-Hendy, A. (2021). Human Mesenchymal Stem Cell Therapy and Other Novel Treatment Approaches for Premature Ovarian Insufficiency. Reproductive sciences (Thousand Oaks, Calif.), 28(6), 1688–1696. https://doi.org/10.1007/s43032-021-00528-z
[2] Shareghi-Oskoue, O., Aghebati-Maleki, L., & Yousefi, M. (2021). Transplantation of human umbilical cord mesenchymal stem cells to treat premature ovarian failure. Stem cell research & therapy, 12(1) , 454. https://doi.org/10.1186/s13287-021-02529-w
[3] Xiao, GY, Liu, IH, Cheng, CC, Chang, CC, Lee, YH, Cheng, WT, & Wu, SC (2014). Amniotic fluid stem cells prevent follicle atresia and rescue fertility of mice with premature ovarian failure induced by chemotherapy. PloS one, 9(9), e106538. https://doi.org/10.1371/journal.pone.0106538
[4] Mohamed, SA, Shalaby, SM, Abdelaziz, M., Brakta, S., Hill, WD, Ismail, N., & Al-Hendy, A. (2018). Human Mesenchymal Stem Cells Partially Reverse Infertility in Chemotherapy -Induced Ovarian Failure. Reproductive sciences (Thousand Oaks, Calif.), 25(1), 51–63. https://doi.org/10.1177/193371911769970532
[5] Yin, N., Zhao, W., Luo, Q., Yuan, W., Luan, X., & Zhang, H. (2018). Restoring Ovarian Function With Human Placenta-Derived Mesenchymal Stem Cells in Autoimmune -Induced Premature Ovarian Failure Mice Mediated by Treg Cells and Associated Cytokines. Reproductive sciences (Thousand Oaks, Calif.), 25(7), 1073–1082. https://doi.org/10.1177/193371911773215647
[6] Igboeli, P., El Andaloussi, A., Sheikh, U., Takala, H., ElSharoud, A., McHugh, A., Gavrilova-Jordan, L., Levy, S., & Al-Hendy , A. (2020). Intraovarian injection of autologous human mesenchymal stem cells increases estrogen production and reduces menopausal symptoms in women with premature ovarian failure: two case reports and a review of the literature. Journal of medical case reports, 14(1), 108. https://doi.org/10.1186/s13256-020-02426-5
Article source: Some pictures and texts come from Boya Life
Stem cells can reverse premature ovarian failure and retain women’s youthful footsteps!
(sourceinternet, reference only)
Disclaimer of medicaltrend.org
Important Note: The information provided is for informational purposes only and should not be considered as medical advice.



