Dynamic reorganization of the tumor microenvironment in the progression of prostate cancer
- Normal Liver Cells Found to Promote Cancer Metastasis to the Liver
- Nearly 80% Complete Remission: Breakthrough in ADC Anti-Tumor Treatment
- Vaccination Against Common Diseases May Prevent Dementia!
- New Alzheimer’s Disease (AD) Diagnosis and Staging Criteria
- Breakthrough in Alzheimer’s Disease: New Nasal Spray Halts Cognitive Decline by Targeting Toxic Protein
- Can the Tap Water at the Paris Olympics be Drunk Directly?
Dynamic reorganization of the tumor microenvironment in the progression of prostate cancer
Dynamic reorganization of the tumor microenvironment in the progression of prostate cancer. Prostate cancer is the second most common malignant tumor in men worldwide. The incidence and mortality of prostate cancer in some countries have been rising sharply in recent years, and it has become the sixth malignant tumor with the sixth incidence and the fourth mortality among men.
Prostate cancer is the second most common malignant tumor in men worldwide. The incidence and mortality of prostate cancer in some countries have been rising sharply in recent years, and it has become the sixth malignant tumor with the sixth incidence and the fourth mortality among men. In 2015, the incidence of prostate cancer in Shanghai exceeded that of liver cancer for the first time, and it became the fourth highest incidence of male malignant tumors in Shanghai, which is close to the developed countries in the West, which seriously threatens the lives and health of men.
Prostate cancer has a large clinical heterogeneity. Most prostate cancers have slow clinical progress, but some still grow relatively quickly, and can rapidly develop bone and lymph node metastasis and are resistant to androgen deprivation therapy, forming castration-resistant prostate cancer ( castration-resistant prostate cancer, CRPC), the latter currently lacks effective treatments, and is the main cause of death in patients with prostate cancer. The molecular heterogeneity of prostate cancer and the heterogeneity of the microenvironmental cell population are the root causes of clinical heterogeneity. So far, no studies have systematically and comprehensively explained it.
On January 9, 2021, Ren Shancheng of Shanghai Changhai Hospital, in cooperation with Ho Housheng from the University of Toronto and Wang Jianhua from Fudan University Cancer Hospital, published in Nature Cell Biology the title: Single cell analysis reveals onset of multiple progression associated transcriptomic remodellings in prostate cancer The first unit of the article is the Department of Urology, Shanghai Changhai Hospital.
The study used single-cell transcriptome sequencing technology to analyze the gene expression of 111,914 single cells in 27 tissue samples including normal prostate, primary prostate cancer, and lymph node metastasis, and systematically mapped the prostate cancer Transcriptome atlas, which clarifies a variety of cell subgroups and transcription level changes related to disease progression in the tumor microenvironment, analyzes the high heterogeneity of prostate cancer, determines the therapeutic target and the aggressive tumor biomarker Development provides an open mind.
The researchers used single-cell sequencing technology to perform single-cell transcriptome sequencing on 12 cases of prostate cancer primary tumors and 1 case of prostate cancer lymph node metastasis samples. A total of 36,424 single-cell data sets were obtained, which were annotated by 20 cell type markers The main cell populations such as epithelial cells, fibroblasts, monocyte-macrophage cell lines, endothelial cells, mast cells, and T cells are included.
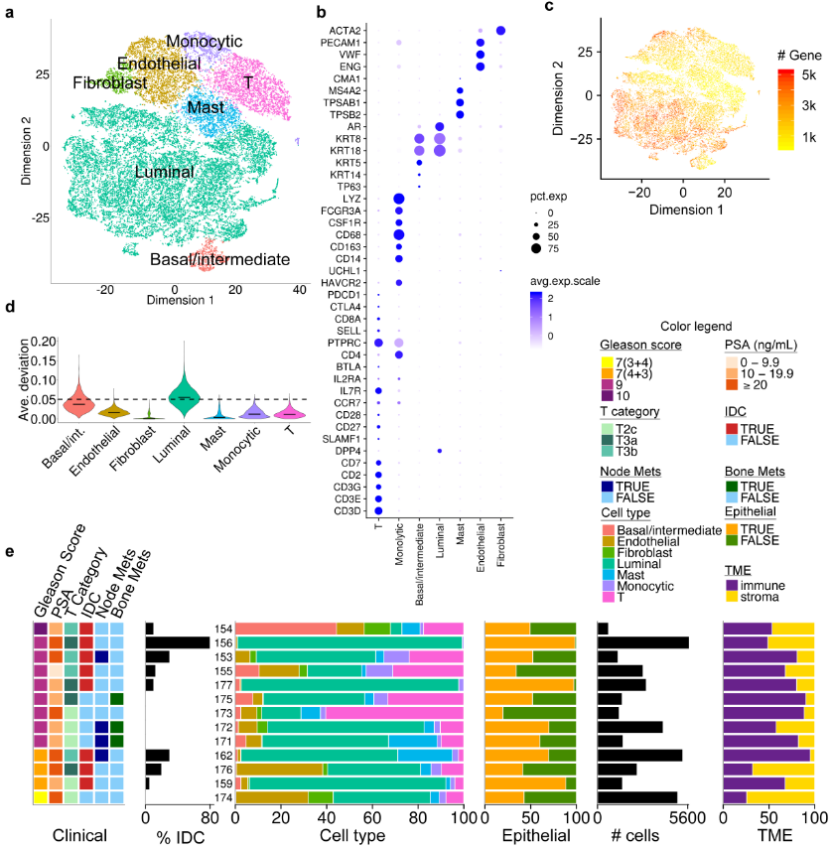
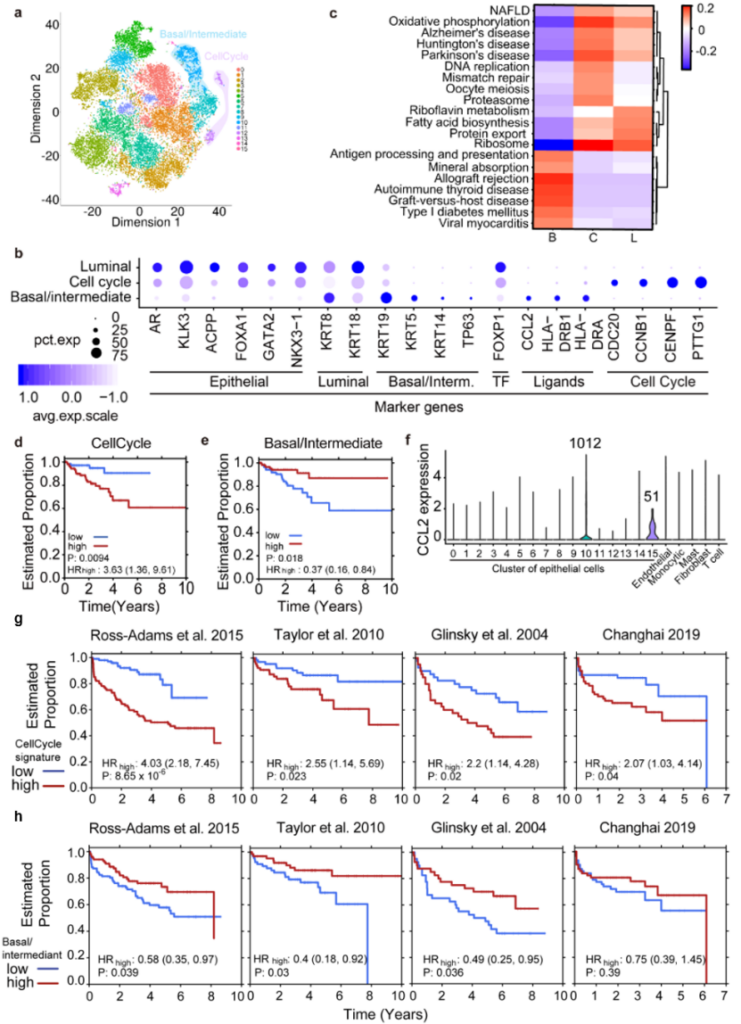
16 subgroups can be obtained by further grouping epithelial cells. The researchers combined the PAM50 classification of breast cancer and previous studies of prostate epithelial cells, and annotated the Basal/intermediate epithelial cell subset (Cluster 10), whose molecular characteristics are related to the better prognosis of prostate cancer, and specifically express transcription factors CCL2; Another subgroup of epithelial cells (Cluster 12) was found to be in the G2/M phase of mitosis, which was named CellCycle cells. Its molecular characteristics are negatively correlated with the prognosis of prostate cancer patients. In addition, the researchers also verified that these two molecular types are related to the prognosis of prostate cancer patients in multiple independent public data sets.
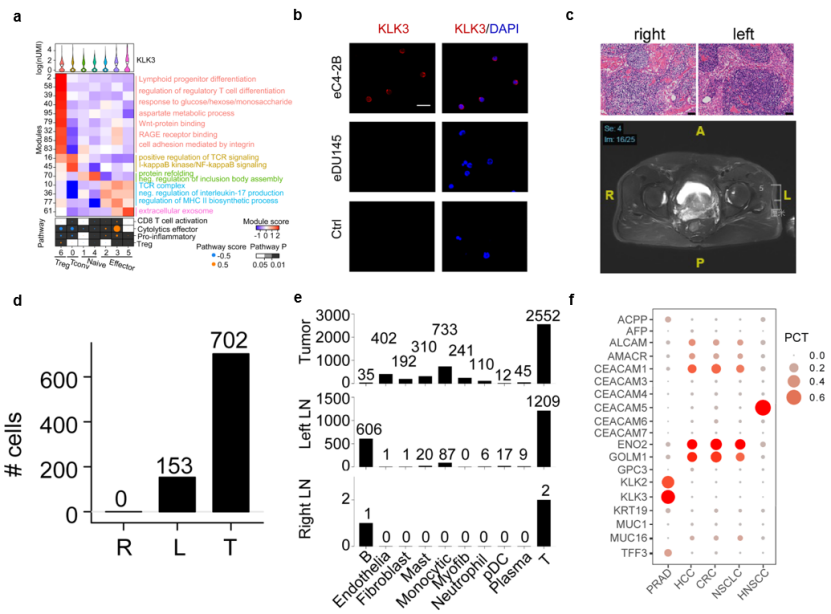
The researchers further studied the infiltrating T cells in prostate tumors and subdivided them into 7 cell subgroups. KLK3 is the gene encoding the prostate-specific antigen PSA. It is a commonly used molecular marker in prostate clinical practice. It is generally believed to be expressed only in prostate cancer cells. However, researchers found that KLK3 is in a subgroup of regulatory T cells (Cluster6) and two effector T cells. Cell subsets (Cluster 3 and 5) are specifically expressed, and the extracellular vesicles and exosomal pathways of the latter are activated, suggesting that tumor-secreted vesicles mediate the transfer of KLK3 to T cells (Figure 1E). The researchers also found T cells expressing PSA/KLK3 through RNA fluorescence in situ hybridization and immunofluorescence experiments, which proved the feasibility of this signal transmission pathway (Figure 1F).
Among the cases involved in the study, the imaging and postoperative pathology of a high-risk prostate cancer patient showed that the left and right external iliac lymph nodes were negative.
Through single-cell transcriptome sequencing, researchers found that there are malignant epithelial cells in the left lymph node tissue, and T cells generally express KLK3, that is, the left lymph node has developed clinically unrecognizable micrometastasis; and despite the right No malignant epithelial cells were found in the lateral lymph node tissues, but T cells have high expression of KLK3, suggesting that the tumor microenvironment cells have formed a “pre-metastatic niche” structure.
This phenomenon is not only present in prostate cancer. Researchers also used single-cell public databases to find that in renal cell carcinoma, colorectal cancer, non-small cell lung cancer, head and neck squamous cell carcinoma and other tumors, T cells are expressed correspondingly The number of tumor markers suggests that it is a widespread phenomenon that tumor cells use their own markers to influence the function of immune cells.
The researchers further studied endothelial cells (EC) and found that some of them highly expressed tumor-associated fibroblasts (CAF) related characteristic genes, so they were named activated endothelial cells (aECs).
The researchers further performed single-cell transcriptome sequencing on 3 additional normal prostate and indolent prostate cancer samples from radical bladder surgery and 5 tumor tissue samples from CRPC patients. Through pseudo-chronological analysis, it was found that the proportion of aEC varies with the tumor. Progression to CRPC gradually increased, most of the aEC cell subsets were derived from CRPC samples, indicating that aEC cell subsets are closely related to the progression of prostate cancer to CRPC.
To verify this finding, the researchers used flow sorting to isolate aEC cell subpopulations from prostate (cancer) samples from patients with primary prostate cancer, CRPC, and bladder cancer, and found that most aEC cell subpopulations were derived from CRPC samples. Researchers found that aEC cell subsets can increase the invasion ability of prostate cancer cells through co-culture. These experiments have confirmed that aEC cell subsets play an important role in the development of prostate cancer.

The study revealed the changes of cell subgroups in the microenvironment at various stages of the development of prostate cancer through single-cell transcriptome sequencing technology, updated the understanding of tumor markers, and discovered molecular typing markers at the single-cell level of prostate cancer and Cell subtypes related to tumor progression are of great value for the development of new treatment strategies for prostate cancer and tumor biomarkers.
Nature Cell Biology published news and expert opinions on the topic of Prostate cancer hijacks the microenvironment at the same time, and highly praised the study for revealing the previously unknown changes in the prostate cancer microenvironment, which opened up multiple paths for the treatment of prostate cancer metastasis.
(source:chinanet, reference only)
Disclaimer of medicaltrend.org



